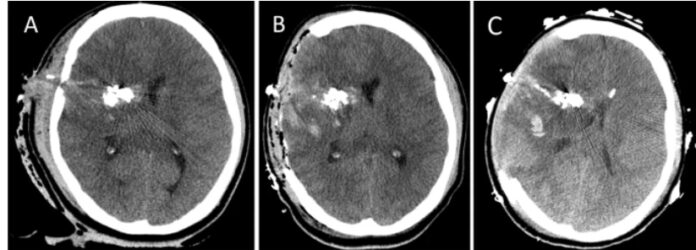
Case Presentation
A young Hispanic man in his early twenties, with no significant past medical history, presented to the hospital after sustaining a gunshot wound to the head. His initial condition was critical, with a low Glasgow Coma Score, indicating severe brain injury. A brain scan revealed a penetrating injury to the right frontal lobe, causing significant brain swelling and bleeding.
Management
Doctors performed emergency surgery to relieve pressure within the skull. This included the removal of a portion of the skull bone and the placement of a device to drain excess fluid.
Following surgery, the patient exhibited significant neurological deficits, including limited eye movements, reduced breathing reflexes, and weakness in all four limbs. Over the course of his extended hospital stay, he gradually improved, regaining some movement and responsiveness on his right side. However, complications arose when a feeding tube became dislodged, leading to an infection. Thus, doctors inserted a second feeding tube to ensure adequate nutrition.
Complications
This patient’s recovery following a severe head injury was a complex process. Initially, he suffered from communicating hydrocephalus, a condition where excess fluid accumulates within the brain. This required the placement of a shunt. A shunt is a medical device that diverts excess fluid from the brain to another part of the body. However, managing the shunt proved challenging, with repeated adjustments and replacements necessary due to infections and ongoing difficulties in regulating fluid flow.
Despite these complications, the patient demonstrated gradual neurological improvement. He regained some movement and responsiveness, particularly on his right side. However, new challenges emerged. He developed intermittent fevers, likely related to infections, and experienced significant respiratory difficulties, including rapid breathing, low blood oxygen levels, and an irregular heartbeat. Medical imaging revealed significant lung collapse and fluid accumulation in the chest. This necessitated the insertion of a chest tube to drain the fluid and improve lung function.
A further complication arose when the skin overlying the craniectomy site, where a portion of the skull bone had been removed, began to sink inward (called the sinking skin flap syndrome). Doctors addressed this by adjusting the pressure within the shunt system. This adjustment effectively re-expanded the sunken skin flap.
Discharge
Doctors discharged the patient from the hospital after 58 days and transferred him to a specialized rehabilitation center. At this point, he could slightly move his left arm and leg, but had more movement on the right side. He was alert and able to communicate clearly. Over the next few months, he successfully came off his breathing tube and feeding tube. While he experienced some lasting weakness and stiffness on his left side, he remained mentally sharp. Two and a half years later, he underwent surgery to repair the damaged area of his skull. Thus, his brain function remained stable.
Decompressive Craniectomy
Decompressive craniectomy is a surgical procedure used to relieve pressure within the skull. This is often necessary when brain swelling occurs due to conditions like brain injury or bleeding. However, this procedure can sometimes lead to a complication called sinking skin flap syndrome, where the skin overlying the surgical site sinks inward. This can cause various neurological problems.
Hydrocephalus, a condition where excess fluid builds up within the brain, is a common complication of brain injury. To treat hydrocephalus, doctors often insert a shunt, a thin tube that drains the excess fluid from the brain to another part of the body, such as the abdomen (ventriculoperitoneal shunt – VPS). When the abdomen is not suitable for shunt placement, an alternative is the ventriculopleural shunt (VPLS), which drains fluid into the chest cavity. While less common than VPS, VPLS has shown promising results in both children and adults.
A potential complication of VPLS is the development of fluid accumulation in the chest cavity (pleural effusion). While this can often be treated with a chest tube to drain the excess fluid, managing the potential complications of this procedure requires careful consideration.
Discussion
This case report describes a patient who developed sinking skin flap syndrome after a chest tube was inserted to treat a pleural effusion that occurred following VPLS placement. It highlights the importance of understanding how fluid dynamics within the body can be affected by these procedures and the potential for unexpected complications.
Sinking skin flap syndrome (SSFS) is a known complication after brain surgery where a portion of the skull is removed (craniectomy). While the exact cause isn’t fully understood, several factors likely play a role. This includes changes in pressure within the skull, decreased blood flow to the brain, and shifts in cerebrospinal fluid (CSF) flow. In this case, the patient developed SSFS after undergoing a procedure to drain fluid from the chest (chest tube placement) following the insertion of a ventriculopleural shunt (VPLS).
Several factors may have contributed to the development of SSFS in this patient. The sudden decrease in pressure within the chest cavity caused by the chest tube suction likely played a significant role. This may have led to increased drainage of CSF from the brain, resulting in a drop in pressure within the skull and causing the skin to sink inward. To address this complication, doctors increased the shunt pressure to reduce the flow of CSF, and the chest tube suction was adjusted. This intervention successfully resolved the issue.