The Use of Ketamine
Depression, suicidal thoughts, post-traumatic stress disorder (PTSD), and substance abuse can often occur together, creating significant challenges for healthcare professionals. Ketamine, primarily used as an anesthetic, has shown promise in reducing symptoms of these conditions.
Ketamine produces noticeable changes in brain function, as observed through brain imaging and brainwave recordings. It increases the production of important growth factors in the brain, reversing the harmful effects of stress on brain cells. Additionally, ketamine strengthens the connections between brain cells, potentially aiding in the recovery of neural networks damaged by chronic stress associated with conditions like depression, PTSD, and substance abuse. These effects can be long-lasting due to ketamine’s ability to promote the growth of new brain cells.
These changes in brain function can manifest as a shift in mindset and the ability to think differently. This can lead to individuals making positive changes in their lives to align with this new perspective.
Case Presentation
This study focuses on two patients who sought ketamine treatment for conditions that had not responded to other therapies. One patient suffered from PTSD and suicidal thoughts, while the other had severe depression. Researchers closely monitored these patients throughout their treatment using brainwave recordings, symptom assessments, and detailed accounts of their experiences. They analyzed the extent and duration of changes in both symptoms and brain activity before and after treatment.
This research focuses on three key brainwave measurements: alpha wave frequency, alpha wave distribution, and P300 amplitude. Alpha waves are a type of brainwave associated with relaxation. Alpha wave frequency, typically between 8 and 12 cycles per second, can provide insights into brain function and overall health. A consistent alpha wave frequency in an individual can act as a reliable marker of their brain’s natural rhythm. Slowing of alpha wave frequency has been observed in conditions like dementia and may also be present in people with PTSD and depression.
The distribution of alpha wave activity across the scalp is also important. In some cases, people with PTSD or depression may show an imbalance in alpha wave activity between the left and right sides of the brain. P300 is a type of brainwave response measured in response to a surprising or unexpected stimulus. A weaker P300 response can be observed in conditions like dementia, head injuries, substance abuse, depression, PTSD, and heart disease.
Procedure
Before receiving ketamine treatment, patients underwent a comprehensive evaluation, including an assessment of suicidal thoughts. They then underwent a baseline brainwave recording using a standard procedure. This involved listening to a series of sounds and measuring the brain’s response to an occasional unexpected sound.
Case 1: Results
The first patient was a 56-year-old man with a history of alcohol abuse and PTSD. He had experienced severe suicidal thoughts for many years. Despite numerous treatment attempts, his symptoms persisted. He then decided to try ketamine treatment.
Before his first ketamine infusion, the patient underwent a baseline brainwave recording. While he exhibited symptoms of PTSD and severe suicidal thoughts, his initial brainwave patterns did not show the typical abnormalities associated with these conditions. Specifically, his brainwave activity across different frequency ranges appeared normal, and there was no noticeable imbalance in activity between the left and right sides of the brain. Furthermore, his P300 response was within the normal range for his age.
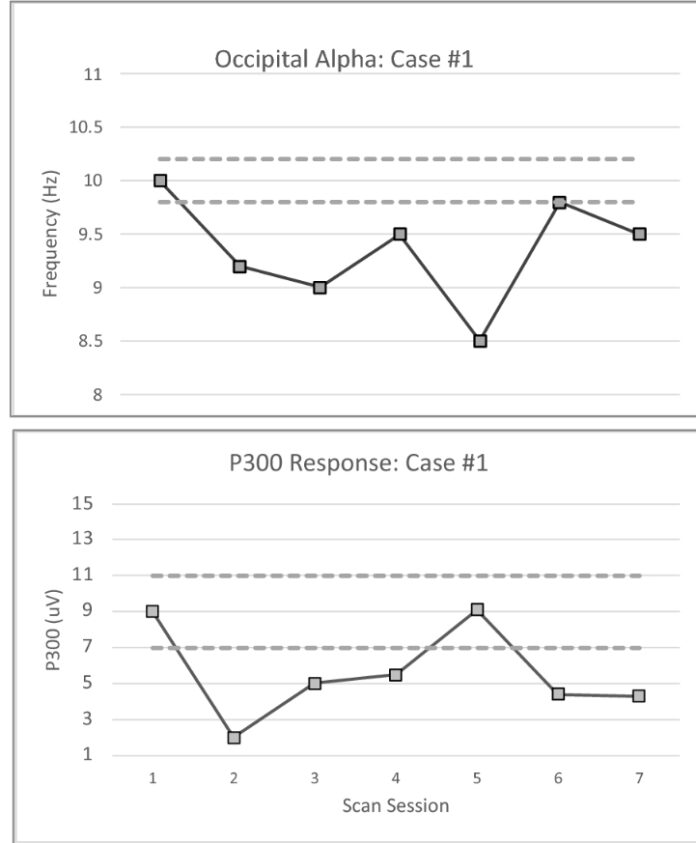
The patient’s brainwave activity underwent significant changes after the first ketamine infusion. Notably, the P300 response, which reflects how the brain processes unexpected information, weakened dramatically. Simultaneously, the dominant frequency of brainwaves (alpha waves) slowed down, and their distribution shifted towards the front of the brain. These changes were unexpected and significant, as alpha wave frequency is generally considered a stable trait in individuals. This pattern of changes resembled those observed in people recovering from a concussion. Surprisingly, these changes persisted for 16 days after the infusion, along with a remarkable improvement in the patient’s symptoms.
Similar brainwave patterns were observed in the second scan, with an even more pronounced shift in alpha wave activity towards the front of the brain. These changes, along with the improvement in symptoms, continued for up to 58 days after treatment. Subsequent scans revealed a gradual return to normal alpha wave distribution while symptoms continued to improve. However, the dominant frequency of brainwaves remained lower than before, and the P300 response remained unstable.
Case 2: Final Scan
The final scan, conducted 78 days after the last ketamine infusion, showed a return to normal brainwave frequencies and distribution. However, the P300 response still hadn’t fully recovered. Despite this, the patient reported a significant and sustained improvement in symptoms, with his score on the suicidal ideation scale dropping dramatically from 40 out of 50 to just 2 out of 50. Throughout the entire treatment course, the patient consistently reported an overall improvement in his condition.
Case 2: Results
The second patient was a 52-year-old woman with a history of alcohol abuse and a diagnosis of depression and bipolar disorder. After years of unsuccessful treatments, she decided to try ketamine infusions.
Before starting treatment, the patient underwent a baseline brainwave recording. While she experienced anxiety and depression, her initial brainwave patterns were generally normal. However, her dominant brainwave frequency (alpha wave frequency) was slightly higher than expected for her age. Following the first ketamine infusion, the patient reported feeling more hopeful, peaceful, and relaxed. While she still experienced some anxiety, she felt more optimistic about the future.
After the final infusion, the patient reported a significant improvement in her overall well-being. She described feeling transformed and noticed a marked improvement in her interactions with others. These positive changes were accompanied by a significant increase in her brain’s response to unexpected stimuli (P300 amplitude), as measured by brainwave recordings. It’s important to note that this increase in brainwave response was the opposite of what was observed in the first patient, whose brainwave response to unexpected stimuli decreased following ketamine treatment.
Discussion: Ketamine
Ketamine infusions appeared to improve symptoms of PTSD, depression, and suicidal thoughts in these patients, accompanied by noticeable changes in brainwave activity. In the first patient, who struggled with PTSD and suicidal thoughts, the most striking change was a significant decrease in the brain’s response to unexpected stimuli after the first ketamine infusion. This decrease, along with a reduction in suicidal thoughts, could be interpreted as a “reset” of the brain or a shift in how the patient perceived the world. These changes in brain activity and symptoms persisted for 78 days after treatment, suggesting long-lasting effects of ketamine.
The second patient, who had depression, showed a different pattern of brainwave changes. While her depression symptoms improved, her brain’s response to unexpected stimuli increased significantly. These varying brainwave responses in the two patients suggest that the effects of ketamine may differ depending on the individual and their specific condition.
Conclusion: Ketamine
In conclusion, ketamine infusions seemed to be effective in improving symptoms and inducing lasting changes in brain function in these patients with treatment-resistant conditions. These findings highlight the potential of ketamine as a promising treatment option for individuals struggling with severe depression and PTSD.