Case Report
Pyoderma gangrenosum (PG) is a chronic inflammatory neutrophilic dermatosis that affects an estimated 3-10 million people worldwide each year. It is distinguished by erythematosus nodules or pustules. That progress to severe ulcers with violaceous weakened margins in the lower extremities.
PG can occur on its own or in conjunction with other systemic disorders. Up to 86% of patients have reported a link to systemic diseases such as chronic inflammatory bowel disease, inflammatory arthritis, and hematological abnormalities. The physiopathological mechanisms behind this dermatosis are still somewhat speculative.
However, an immune-mediated mechanism appears to be plausible for the upregulation of pro-inflammatory cytokines. And positive responses to immune-modulatory medications in PG patients. However, its link to granulomatosis with polyangiitis (GPA) has been infrequently described. This report describes an unusual occurrence of GPA coupled with PG.
Case Presentation
A 26-year-old Tunisian guy came in with a 2-month history of bilateral nasal blockage and red discharge. Nasal endoscopic examination indicated mucosal hyperemia, crusting, and granulation. A craniofacial computed tomography (CT) scan showed mucosal thickening in the right maxillary sinus. Nasal biopsies revealed persistent inflammation with necrosis. Serum anti-neutrophil cytoplasmic antibody (ANCA) against PR3 was negative. Clinical, radiological, and histological findings supported the diagnosis of localized GPA.
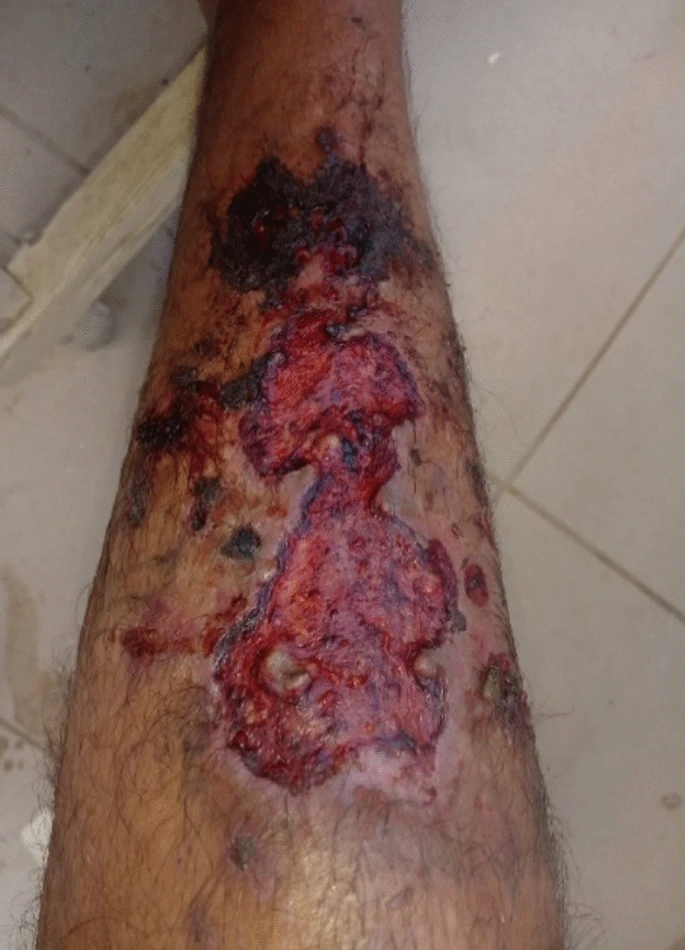
The patient was treated with intravenous methylprednisolone (1 g/day for 3 days) that was gradually tapered, followed by intravenous cyclophosphamide pulses on days 1 and 14, and was then lost to follow-up. Three years later, he was readmitted with major complaints of bloody crusting rhinorrhea, anosmia, persistent nasal obstruction. And a 4-month history of a big ulcer in his right lower leg.
Investigation:
A CT scan indicated full lysis of the nasal septum and conchae, as well as a rupture in the hard palate. His physical examination revealed a 20 cm lesion with necrosis and pus. Laboratory testing for erythrocyte sedimentation rate, cell blood count, creatinine, electrolytes, aspartate aminotransferase, and alanine aminotransferase were all normal. Pus culture was unfavorable. A skin biopsy revealed a thick inflammatory infiltration created by polymorphonuclear neutrophils with broken nuclei generating leukocytoclastic lesions coupled with lymphocytes and histiocytes without any evidence of malignancy.
The diagnosis of PG with localized GPA was established. He was also begun on three methylprednisolone pulses, followed by oral corticosteroids and a cyclophosphamide regimen, with quick recovery.
Discussion:
GPA is a systemic necrotizing vasculitis that affects tiny arteries, primarily in the upper and lower respiratory tracts and the kidney. Skin involvement is less common, estimated at 10-15% of cases, and more common in systemic variants. Skin lesions in GPA can be characterized as specific or nonspecific, according on the underlying histological abnormalities.
Specific skin lesions have histological characteristics of vasculitis or granulomas. However, nonspecific cutaneous manifestations lack any of the distinguishing characteristics. The most common clinical signs of skin involvement in GPA include palpable purpura or petechia, livedo reticularis or racemosa, papules, and subcutaneous nodules. Several examples of pyoderma gangrenosum-like ulcers with big, painful lesions and undefined margins have been documented.
However, few examples of real PG in individuals with GPA have been described. The lack of specialized diagnostic techniques makes it difficult to distinguish between real PG ulcers and PG-like ulcers. In fact, both illnesses share many characteristics, including the clinical presentation of single or several painful ulcers with elevated, undermined erythematous margins, primarily situated in the lower extremities.
The treatment of PG is still empirical and depends on the severity and extent of the lesion, as well as the underlying condition. Systemic corticosteroids are the primary treatment for both PG and GPA. Immunosuppressive drugs, including methotrexate, cyclophospamide azathioprine, mofetil mycophenolate, and rituximab, are suggested based on the level and pattern of organ involvement in patients with GPA.