Breast Cancer
Breast cancer remains the most prevalent cancer among women globally, surpassing even lung cancer in 2020 with a staggering 2.26 million new cases reported. Sadly, liver metastasis, the spread of cancer cells to the liver, affects about half of women with metastatic breast cancer. This contributes significantly to breast cancer-related deaths. While treatments like systemic chemotherapy and liver surgery can improve survival, the prognosis for women with liver metastases remains challenging.
The survival rates following treatment for liver metastases vary widely. Some studies have shown promising results, with 3-year and 5-year survival rates ranging from 49% to 94% and 5% to 78%, respectively. However, other studies have reported less optimistic outcomes.
Several factors can significantly influence the success of treatment. The characteristics of the primary tumor play a crucial role. Smaller tumors, the absence of lymph node involvement, low-grade tumors, and early-stage breast cancer are generally associated with better outcomes. The time interval between the initial breast cancer diagnosis and the discovery of liver metastases is another critical factor, with a longer interval often linked to better survival. The extent of the disease also impacts outcomes, with patients with liver-limited disease, tending to have better outcomes. The response to pre-surgery treatment is another important consideration. This is because patients who respond well to systemic therapy before liver surgery typically have improved survival rates. Finally, the presence of estrogen receptors (ER) and progesterone receptors (PgR) in the liver metastases can be a positive prognostic factor.
Despite these potential benefits, the use of liver surgery combined with systemic therapy has been limited. Historical treatment approaches, resource constraints, and the lack of clear, evidence-based guidelines have hindered the wider adoption of this approach.
Furthermore, the presence of liver metastases at the time of initial breast cancer diagnosis carries a significantly worse prognosis, with a median survival of only 12 months. In some cases, patients develop disseminated intrasinusoidal metastatic liver disease (DISML). This is a condition where cancer cells spread extensively within the liver, leading to acute liver failure and ultimately death.
Case Presentation
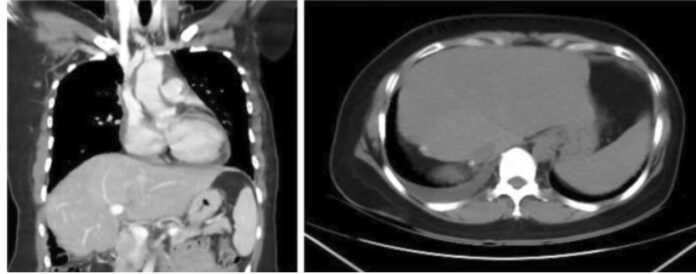
A 51-year-old woman was diagnosed with breast cancer in May 2020. The cancer, classified as an invasive carcinoma, had already spread to both her lungs and liver. Despite the advanced stage of the disease, the patient underwent a mastectomy to remove the breast tumor and received chemotherapy.
Following chemotherapy, imaging tests revealed multiple small tumors in her liver. A surgical procedure was then performed to remove one of these liver tumors. After the surgery, further imaging tests showed no remaining evidence of cancer in the liver. The patient continues to receive hormonal therapy as part of her ongoing treatment.
Importantly, the patient remains in good health with no signs of the cancer returning. This case demonstrates a successful outcome for a patient with advanced breast cancer, highlighting the potential for effective treatment strategies, including surgery, for carefully selected patients with liver metastases.
Discussion
Despite advancements in systemic treatments for metastatic breast cancer (MBC), the median survival for patients typically ranges from 18 to 24 months. For select individuals, surgical removal of liver metastases can offer a viable treatment option. Optimal outcomes are achieved when these surgeries are performed in specialized centers by highly experienced surgeons. This is often following a careful multidisciplinary evaluation, similar to the management of other complex cancers.
A comprehensive review of studies on liver metastasis resection in MBC demonstrated a median overall survival of 35.1 months and a median disease-free survival of 21.5 months. Importantly, patients who underwent resection showed significantly longer overall survival (82 months) compared to those receiving only systemic therapy (31 months). This highlights the potential survival benefit of combining surgery with systemic treatment.
Several factors influence the success of liver surgery for breast cancer. Patients with estrogen receptor (ER) and/or progesterone receptor (PgR)-positive breast cancer liver metastases may benefit significantly from surgery. This is particularly due to the potential for effective hormone therapy. Characteristics of the primary breast cancer, are also associated with better outcomes following liver surgery. This includes small tumor size, absence of lymph node involvement, low grade, and early stage. Conversely, patients with triple-negative breast cancer, an aggressive form of the disease, may not derive as much benefit from liver surgery due to limited treatment options.
The response to preoperative systemic therapy plays a crucial role in determining the success of liver surgery. Successful eradication of microscopic metastatic disease through systemic therapy can enhance the effectiveness of subsequent liver surgery.
The presence of HER2 overexpression in liver metastases has also been linked to improved survival outcomes. The majority of patients with HER2-positive breast cancer receive targeted therapy. However, the potential for combining local therapy (like surgery) with these targeted treatments offers promising avenues for improving outcomes. Traditional treatment approaches for liver metastases, such as systemic chemotherapy and arterial injection chemotherapy, have shown limited success in significantly prolonging survival.
Conclusion
In conclusion, liver resection, when performed in appropriate patients and combined with effective systemic therapy, has the potential to significantly improve survival outcomes for individuals with breast cancer and liver metastases. However, further research is crucial to identify the most suitable candidates for this aggressive treatment approach.
Breast cancer that spreads to the liver presents a significant challenge for doctors, with limited treatment options and often a poor outcome. However, this case demonstrate that surgery to remove liver metastases can offer hope for some patients. A multidisciplinary approach, where surgeons, medical oncologists, and other specialists work together, is crucial for optimizing treatment. This collaborative approach allows for personalized treatment plans based on each patient’s individual needs and the specific characteristics of their cancer. By working together, healthcare professionals can improve the effectiveness of both surgery and systemic therapies. Thus, ultimately improving the chances of successful treatment for patients with breast cancer that has spread to the liver.