Case Report
Atrial flutter (AFL) is a frequent supraventricular arrhythmia characterized by rapid atrial activation with no discernible P waves. And an ordered pattern of conduction. While traditional AFL is characterized by a sawtooth pattern on electrocardiography (ECG). An atypical cases can show irregular conduction, making differential diagnosis difficult. In rare circumstances, atrial waves may be difficult to detect on an ECG, confounding the diagnosis.
In clinical practice, identifying AFL from other atrial tachyarrhythmias, such as atrial fibrillation (AF) or focal atrial tachycardia (AT), is critical for effective treatment.
Misdiagnosis or categorization confusion may result in ineffective treatment methods. As different atrial tachyarrhythmias necessitate different therapeutic approaches, such as rate control, antiarrhythmic medications, catheter ablation, or anticoagulant therapy. Traditional diagnostic methods, including as surface ECG and Holter monitoring, may not always yield definitive results, especially in patients with varied conduction patterns. In such cases, intracardiac electrophysiology studies (EPS) play an important role in verifying the diagnosis and guiding suitable treatment.
This report describes a case of complex AFL in which typical ECG results were ambiguous, resulting in diagnostic ambiguity and treatment planning issues. The final diagnosis was made using EPS, which validated the arrhythmia mechanism and offered direction for targeted management. This research emphasizes the diagnostic significance of EPS in difficult cases of atrial arrhythmia. And gives information on crucial electrophysiological findings for distinguishing atypical AFL from other tachyarrhythmias.
Case Presentation
A 60-year-old Chinese woman with rheumatic mitral stenosis. And a previous mitral valve replacement/maze surgery for atrial fibrillation reported recurrent fatigue while taking therapeutic warfarin (INR 2.1).
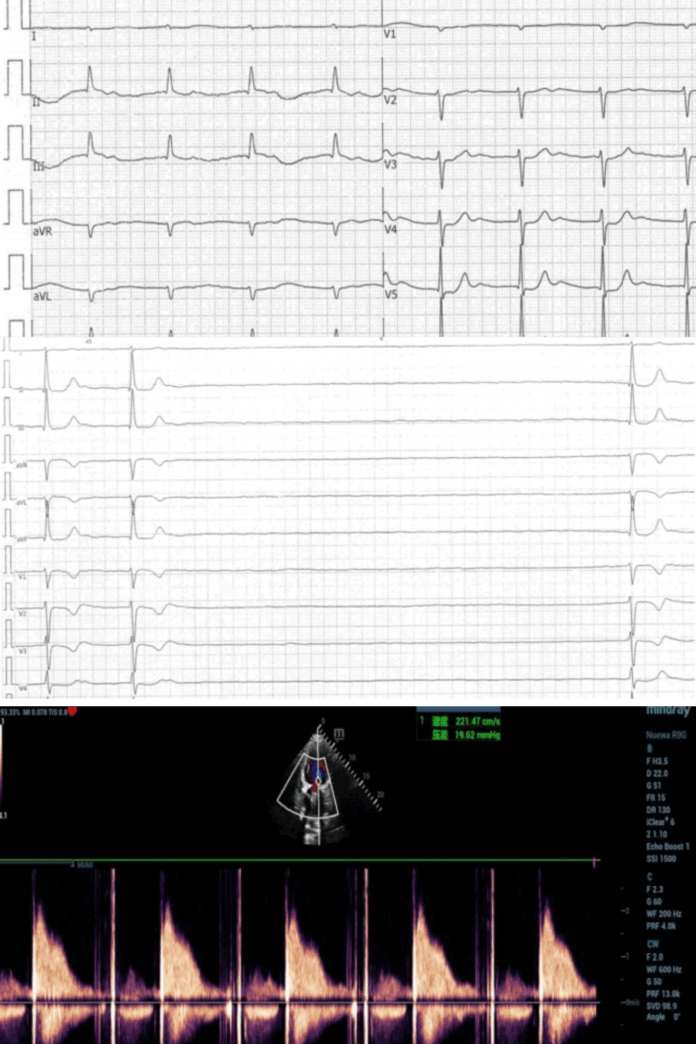
Despite technical optimizations such as improved calibration. The initial assessment revealed symptomatic bradycardia (47 bpm) with complete absence of atrial activity on the 12-lead ECG.
The modified Lewis lead configuration (right arm (RA) electrode at sternal manubrium, left arm (LA) at right fourth intercostal space, and left leg (LL) unchanged) again failed to identify P waves (Fig. 1). Subsequent 24-hour Holter monitoring indicated ventricular pauses of up to 7.7 seconds (Fig. 2), whereas transthoracic echocardiography revealed a monophasic mitral inflow pattern (isolated E wave without A wave; Fig. 3, indicating atrial mechanical standstill.
The diagnostic impasse was addressed with an invasive electrophysiological evaluation. Intracardiac mapping revealed (1) cavotricuspid isthmus-dependent atrial flutter with counterclockwise activation, and (2) widespread right atrial low-voltage zones indicating significant fibrosis.
Radiofrequency ablation of the cavotricuspid isthmus resulted in bidirectional conduction block, which successfully terminated the arrhythmia despite a brief 6082 millisecond sinus arrest post-ablation. The post-procedural rhythm stabilized at 59 bpm, with no surface-detectable P waves on the modified Lewis lead ECG, indicating continued atrial electromechanical dissociation. The patient experienced significant clinical improvement and was discharged without needing a permanent pacemaker implant.
Discussion and conclusion
This case demonstrates the intricate relationship between advanced cardiac anatomical alterations. And the diagnostic issues they present, notably in the diagnosis and treatment of atrial arrhythmias. Traditional diagnostic procedures such as surface ECGs, as well as more advanced methodologies like as the modified Lewis lead ECG, may fail to detect atrial activity in patients with severe atrial fibrosis.
This failure is often due to the presence of significant scarring. And low-voltage areas within the atrium, as confirmed by the electrophysiological study (EPS) in this patient. The EPS was pivotal, not only in identifying these structural abnormalities. But also in uncovering the underlying atrial flutter that was not apparent on the initial ECG.
Based on the ECG findings of absent P waves and a ventricular rate of 47 bpm. The differential diagnosis included junctional rhythm, atrial quiet, atrial fibrillation with atrioventricular block (AF with AVB). And atrial flutter (AFL) or atrial tachycardia (AT) with unseen P waves. Given the regular rhythm and the arrhythmia’s effective termination with cavotricuspid isthmus ablation, cavotricuspid isthmus-dependent atrial flutter is the most probable diagnosis.
This instance emphasizes the importance of extensive electrophysiological testing before continuing with pacemaker installation in individuals with unexplained bradycardia and arrhythmias. By accurately detecting the atrial flutter and treating it with suitable ablation, the necessity for a pacemaker was eliminated, eliminating the risk of pacemaker syndrome and emphasizing the need of precision in cardiac arrhythmia treatment. Such findings are critical for improving our knowledge and treatment of complicated arrhythmias in the presence of substantial atrial fibrosis, ensuring that therapies are both appropriate and successful.