Case Presentation
A 26-year-old healthy Caucasian Moroccan woman visited the oral surgery department at the consultation and treatment center in Rabat. She complained of a painless swelling on the left side of her face that had appeared four days earlier. She also mentioned experiencing weight loss and fatigue over the past month.
Examination
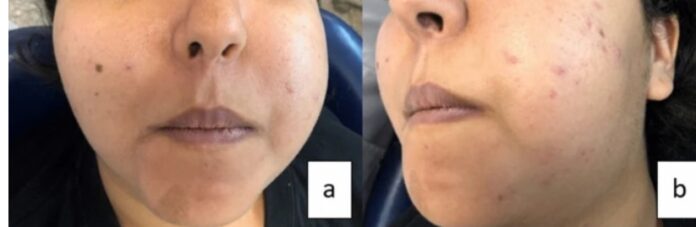
Upon examination, there was noticeable swelling on the left side of her face, causing facial asymmetry and affecting both the maxillary and mandibular areas. The swelling felt soft and the skin appeared normal in color. In the cervical lymph node areas, a medium-sized, mobile, and painless lymphadenopathy was detected. The patient also reported paresthesia (a tingling or numb sensation) on the left mandible and lower lip, which had started a month prior but was gradually improving.
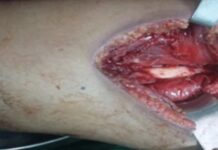
Intraoral examination revealed a tumor-like mass that was reddish, firm, and ulcerated in some areas. This mass was located on the left mandibular ridge, extending from tooth 38 to tooth 43, but it did not involve the floor of the mouth. A similar mass was observed on the maxillary ridge, extending from tooth 28 to tooth 24 and affecting the vestibular, palatine, and left hard palate areas. The patient’s teeth showed no signs of cavities or mobility, except for a slight palatal displacement of teeth 23, 24, and 25. She also exhibited a limited ability to open her mouth, measuring only one and a half fingers wide.
Investigation
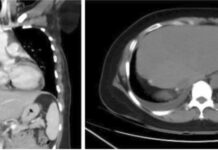
Radiographic imaging through orthopantomography revealed a widening of the periodontal ligament space in several teeth, including 25, 26, 28, 38, 35, and 44. There was also a radiopaque mass in the right maxillary sinus occupying most of the sinus. A CT scan showed nearly complete filling of the right maxillary sinus, which extended into the homolateral nasal fossa through the sinus ostium, creating a double sac structure resembling an antrochoanal polyp. Additionally, there was significant mucosal thickening at the floor of the left maxillary sinus.
A full blood analysis was conducted, and while most results were within normal ranges, the polymorphonuclear eosinophil count was elevated. Given the rapid growth of the tumor, its physical characteristics, the widening of the periodontal ligament space, and the paresthesia, a malignant tumor was suspected.
An incisional biopsy was performed by a maxillofacial surgeon. Histopathological examination revealed a diagnosis of Burkitt lymphoma (BL), characterized by the diffuse proliferation of medium-sized cells and a distinctive “starry sky” pattern created by numerous macrophages. Immunophenotyping indicated a high proliferative index of 100%, as shown by Ki-67 staining. The tumor also tested positive for CD10 and CD20 markers, as well as the MYC oncogene translocation, which is commonly associated with BL. However, tests confirmed that the lesion was not linked to Epstein–Barr virus (EBV), and no other disease locations were identified.
Management
The patient was referred to an oncology hospital, where she began chemotherapy treatment. The regimen included cyclophosphamide and vincristine. One year after starting chemotherapy, the tumor had completely disappeared. The affected areas on the maxillary vestibular, palatal, and mandibular regions showed no signs of the previous lesions. Following this recovery, the patient was referred to a periodontology service for gingival care.
Burkitt Lymphoma
Burkitt’s lymphoma (BL) is an aggressive cancer of B cell lymphocytes and a subtype of non-Hodgkin’s lymphoma (NHL). It is one of the fastest-growing tumors in humans, often affecting children and young adults. BL accounts for about half of malignant tumors in children and 70% of pediatric NHL cases. However, in adults, it is rare, making up only 1–5% of NHL cases, with men being more commonly affected. The tumor frequently targets gnathic bones, especially the maxilla, appearing as a radiolucent image on scans. Histologically, it shows a diffuse growth pattern with uniform medium-sized cells and prominent nuclear features. BL can rapidly develop in the mouth, often forming a mass in the maxilla or presenting as a facial tumor. Here, we describe a rare case of an adult female with isolated oral BL affecting both the maxilla and mandible—an uncommon clinical presentation.
Forms of Burkitt Lymphoma
Two other forms of BL have been identified: sporadic BL and immunodeficiency-associated BL. Sporadic BL, found worldwide, is most common in the West and typically manifests as an intra-abdominal mass. Only about 20% of these cases are associated with EBV. Jaw and sinus involvement occur in 12–30% of cases. Immunodeficiency-associated BL, linked to HIV, is nearly 1,000 times more common in HIV-positive individuals. The variant seen in Moroccan patients mostly involves the abdomen and, less commonly, the jaw.
Oral BL can mimic dental conditions, presenting as swelling, tooth mobility, or mass-like lesions. It may cause tooth displacement, pain, and firm, nonfluctuant swelling. The posterior mandible is the most frequently affected area, although maxilla involvement is rare. BL grows rapidly, often doubling in size within 24 hours, making early diagnosis critical. Radiographic findings vary, with X-rays showing diffuse bone loss and teeth appearing to “float.” Computed tomography can detect osteolytic lesions and bone destruction.
Microscopically, BL is characterized by monomorphic medium-sized cells with a distinctive “starry sky” pattern due to macrophages containing apoptotic debris. Key markers include CD20, CD79a, and MYC, with nearly 100% positivity for Ki-67, indicating high proliferation. BL must be differentiated from other malignancies like carcinomas, sarcomas, and leukemias through histopathological analysis.
Conclusion
Treatment for Burkitt Lymphoma relies on chemotherapy, with monoclonal antibodies like rituximab improving outcomes. Prognosis depends on the patient’s age, disease stage, and timely diagnosis. In one reported case, the lesion progressed rapidly within a month, highlighting the need for urgent intervention.
This case highlights the importance of recognizing oral BL’s atypical presentations, as symptoms can overlap with dental or other conditions. Blood tests and imaging, alongside immunohistochemical profiling, are essential for accurate diagnosis and effective treatment. Early recognition and intervention significantly improve outcomes in this aggressive malignancy.