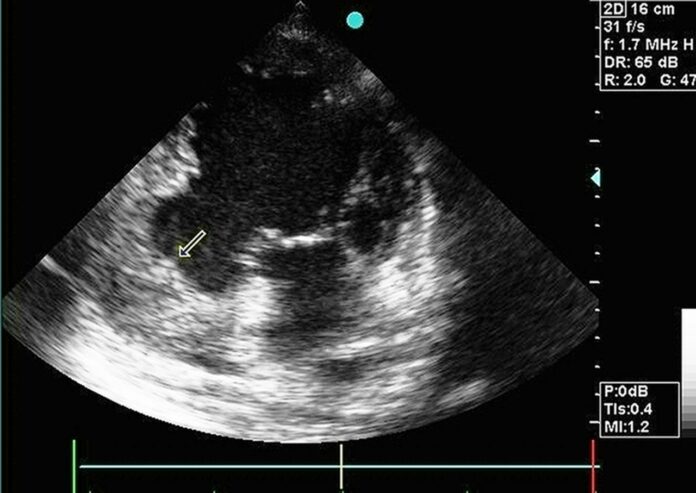
Large basal inferior wall aneurysm with thrombus
This article describes the case of an 80-year-old man diagnosed with large basal inferior wall aneurysm with thrombus. The patient presented with a 3- to 4-month history of shortness of breath on exertion. His medical history revealed that he was non-diabetic, non-hypertensive and a non-smoker. He did not have a history of acute coronary event. Doctors advised an ECG which showed significant Q waves in inferior leads with minimally elevated, ‘coved’ ST segment. The patient’s history was not significant for acute coronary event.
Doctors advised an echocardiogram which showed hypokinesis of the inferior wall and a large basal aneurysm measuring 4.9 x 4.4 cm with a thrombus. However, “spontaneous echo contrast” was absent in left ventricle (LV) near the aneurysm.
Studies have shown that basal inferior wall aneurysms constitute nearly 3% of all left ventricular aneurysms
Although the presence of a large thrombus in these aneurysms is a rare. Uncommon causes of LV aneurysms include cornoary artery disease, connective tissue diseases, such as sarcoidosis and systemic lupus, Chaga’s disease and HIV, chest trauma, coronary artery fistula, myocarditis, arrhythmogenic right ventricular dysplasia and hypertrophic cardiomyopathy. The conditions present with congestive heart failure, ventricular arrhythmias and thrombo-embolic events. It is therefore, important to differentiate between true and pseudo aneurysms or contained rupture.
In patients with pseudoaneurysm, early surgery is indicated and anticoagulation is contraindicated, especially in the initial phase. In cases of true aneurysms, anticoagulation is given for a minimum of 3 months. True aneurysms can be differentiated from pseudoaneurysms with the presence of thrombus within the cavity, evidence of myocardial thickening and a mouth size of more than half of the maximum diameter. In addition, a contrast echocardiogram is preferable compared to plain echocardiogram in patients with poor acoustic windows to identify aneurysms.
For identifying and assessing these aneurysms preoperatively, cardiac MRI (CMR) is the most specific investigation. Patients with and without symptoms have 10-year survival rates of 46% to 90%.
Source: BMJ



