An 85-year-old man was brought to the emergency
room with a short history of loss of consciousness, followed by a collapse. By
the time the patient reached the emergency department, he had regained
consciousness.
The man gave a history of passing dark stools for the past two weeks
The patient had a positive history of breast cancer and nodular melanoma. He was being treated with goserelin and letrozole for breast cancer. For nodular melanoma, a wide local excision had been performed on his right arm along with the dissection of the axillary lymph nodes 5 months earlier. ربح مال حقيقي من النت
On physical examination, he was pale, and his
vitals were:
Heart rate -110 beats per minute
Blood pressure – 115/70.
The complete blood count result revealed a hemoglobin level of 7.6 g per deciliter (normal range, 11.5 to 15.5); therefore, he was transfused one unit of red cells.
Upon endoscopy, numerous polypoid, umbilicated nodules were seen in the stomach with evidence of recent, but not active, bleeding.
Histopathological evaluation was consistent with metastatic melanoma.
Computed tomography showed thickened stomach wall lining, with evidence of metastases in the brain, lung, and liver.
Due to the dissemination of the disease, palliative treatment with radiation, and pembrolizumab was initiated. At the three month follow-up, his melena had further worsened with multiple associated complications.
He was shifted to hospice care and, unfortunately,
died shortly.
Melanoma, also known as malignant melanoma, is the cancerous growth of the pigment cells, called melanocytes. Typically, melanoma is cutaneous, i.e., it occurs in the skin, but it may involve other parts, including oral cavity, gastrointestinal tract.
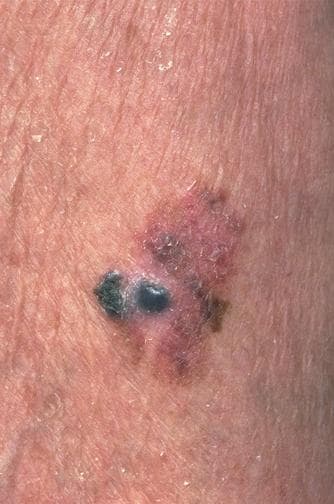
Image Source: Medscape©
The gastrointestinal tract is the most common non-cutaneous metastatic location of the melanoma, 60% of the patients with metastatic melanoma show involvement of the digestive system.
Metastasis to the GI tract is most commonly to the small bowel (51–71%); other affected GI organs can be stomach (27%) and colon (22%).
Mostly, patients with GI metastasis remain asymptomatic or develop symptoms late in the course of the disease when complications have already developed. However, any patient with a history of melanoma presenting with manifestations of anemia or GI symptoms should be evaluated for GI metastases.
CT scan, PET scan, and endoscopy remain the
diagnostic modalities of choice. Endoscopy with biopsy is an indispensable investigation.
Surgical resection of metastatic disease has a substantial
impact on overall survival. However, many patients have a widely disseminated disease
making it inoperable; in that case, palliative treatment with chemotherapy,
radiotherapy, and immunotherapy may have a role in improving the quality of
life.
References:
Amanda H.W. Lim, M. B. (2020, January 30). Gastrointestinal Bleeding from Metastatic Melanoma. Retrieved from The New England Journal of Medicine: https://www.nejm.org/doi/full/10.1056/NEJMicm1909170
Silva, S., Tenreiro, N., Melo, A., Lage, J., Moreira, H., Próspero, F., & Avelar, P. (2018). Metastatic melanoma: An unusual cause of gastrointestinal bleeding and intussusception-A case report. International journal of surgery case reports, 53, 144–146. كيف تربح المال من الانترنت مجاناً https://doi.org/10.1016/j.ijscr.2018.10.057
Patti R., Cacciatori M., Guercio G., Territo V., Di Vita G. Intestinal melanoma: a broad spectrum of clinical presentation. بوكر اون لاين حقيقي Int. J. Surg. Case Rep. 2012;3:395–398




