As the end to the COVID-19 pandemic continues to evade us, scientists also continue to work on treatments for the disease. As such, a potentially new and interesting contender has emerged from the Rosalind Franklin Institute in the UK.
To date, research on antibody transfusion has primarily focused on taking antibodies from recovered COVID-19 patients. However, research on animal-derived antibodies is now gaining traction.
Llama antibodies, to be exact.
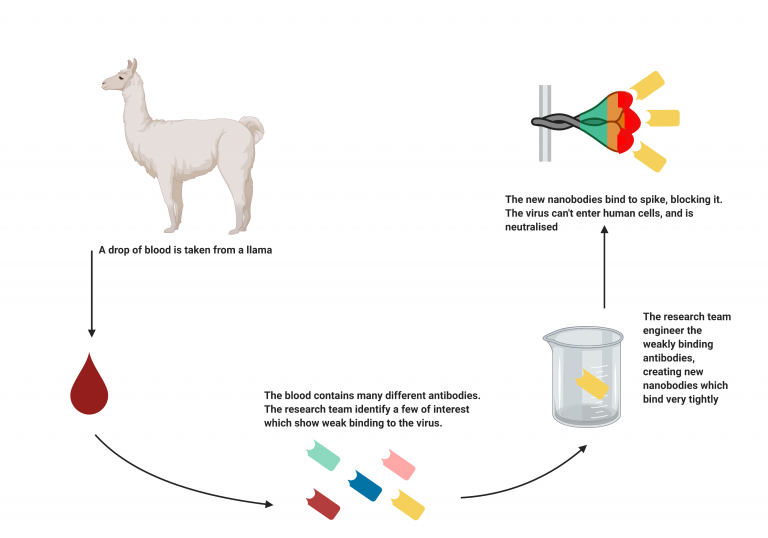
Along with regular double-chained antibodies, Llama’s, camels, and alpaca’s produce a unique single-chained antibody called nanobodies. Previously, researchers from the Rosalind Franklin Institute tested these molecules in a cell culture containing COVID-19 and found that they worked extremely well in neutralizing the virus by binding to it tightly.
These antibodies came from a llama named Fifi, who lives at the University of Reading. Researchers injected the SARS-CoV-2 spike protein into Fifi. Although she did not get sick, her immune system did produce various antibodies. The scientists then found that four types of nanobodies bound weakly to the virus. After purifying them, they combined the molecules into chains to make them more virile.
These chains were effective against the alpha and beta variants, along with the original strain.
The scientist also checked their efficacy on hamster models and found that one of the chains, C5-trimer, decreased the effects of COVID-19 in already infected animals i.e. they lost less weight and had a lower viral load in their respiratory system as compared to control models.
But why llama antibodies?
These short-chained molecules have several advantages over human antibodies that have generated researcher’s interest in them.
According to the study published in Nature Communications, compared to human antibodies, which require mammalian cells to manufacture, these small and stable molecules are easily mass-produced using E-coli. They do not require cold storage, which means that manufacturers can easily transport them to remote areas.
Furthermore, as corresponding author Professor Ray Owens, head of the protein production at the Rosalind Franklin Institute explained:
“They are cheaper to produce and can be delivered directly to the airways through a nebulizer or nasal spray, so can be self-administered at home rather than needing an injection. This could have benefits in terms of ease of use by patients but it also gets the treatment directly to the site of infection in the respiratory tract.”
Now, the authors are looking forward to conducting clinical trials. They hope that their findings are useful to fight future infections quickly.
Source: The Rosalind Franklin Institute
https://www.rfi.ac.uk/llama-antibodies-have-significant-potential-as-potent-covid-19-treatment/