Glucose monitoring is one of the most common tests in the world. In the case of diabetics, it is usually self-administered, sometimes multiple times a day. However, the currently available glucose monitoring systems are based on the molecule’s concentration in blood. This indicates constant invasive or traumatic procedures, either through pricking a needle or embedding a long-term sensor in the body.
Recently, a team from the Pennsylvania State University has demonstrated a non-invasive monitor that uses sweat to measure glucose levels. If approved for commercial use, the device may cover the market gap that exists for such devices.
While such non-invasive devices are usually based on enzymatic reactions, the team wanted to avoid such a method because of the deteriorating nature of biological proteins over time. Therefore, they found a new approach.
A Graphene glucose monitor
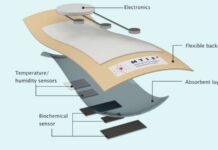
The monitor is a flexible, low-cost device, the size of a quarter. It is mainly made of Laser Induced Graphene (LIG), a one-atom-thick material that is easy to shape.
However, according to Penn State’s Professor of Engineering Science and Mechanics Huanyu “Larry” Cheng, the lead researcher for this project,
“The challenge here is that LIG is not sensitive to glucose at all.” “So, we needed to deposit a glucose-sensitive material onto the LIG.”
So how did the team create such a device?
The answer is nickel. And gold.
Nickel is a glucose-sensitive element, a perfect match for a sweat-based glucose monitor because sweat carries a very small amount of glucose. However, it can cause hypersensitivity to the wearer; therefore the researchers combined it with gold to make it less reactive.
They also created a small microfluidic chamber to safely house an alkaline solution needed to react with the glucose molecules. The reaction creates an electric signal equal to the amount of glucose in the sweat.
The researchers demonstrated the device’s capability when attached to a volunteer’s arm using a safe adhesive one hour after a meal and 3 hours afterward. They asked the volunteer to engage in light exercise to induce sweating. The device’s result was then compared with a commercially available glucose monitor. Both levels were similar.
The team now wants to explore indications for the device’s use beyond glucose monitoring.
“We want to work with physicians and other health care providers to see how we can apply this technology for daily monitoring of a patient,” Cheng said. “This glucose sensor serves as a foundational example to show that we can improve the detection of biomarkers in sweat at extremely low concentrations.”
Source: The Pennsylvania State University
https://www.psu.edu/news/research/story/monitoring-glucose-levels-no-needles-required/
Biosensors and Bioelectronics
https://linkinghub.elsevier.com/retrieve/pii/S0956566321006436