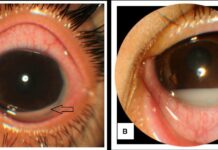
Case report of fat embolism syndrome in 57-year-old patient.
This article highlights the case of 57-year-old male patient diagnosed with fat embolism syndrome. The patient presented to the emergency with a history of fall and right hip pain. His medical history revealed hypertension and old left basal ganglia hemorrhage, for which he underwent right hip surgery. Doctors diagnosed him with a fracture in the right femoral neck and referred him for elective surgery. He was scheduled for a total hip arthroplasty. العب بلاك جاك اون لاين A carotic duplex ultrasound and trasncranial Doppler ultrasound were performed before surgery. The investigation findings showed no significant abnormalities.
However, during surgery the patient developed sudden hypertension for which he was resuscitated with 500 ml of normal saline load. In addition, when the patient was weaned off anaesthetic drugs an hour after surgery, he became unresponsive. العاب ماكينات القمار مجانا He was unable to follow any command or answer any question on evaluation by the consultant physician. لعبة كريكت There was no spontaneous eye opening. His vitals were normal with respiratory rate 35 breaths per minute and 90% to 95% O2 saturation while he was breathing through a non breathing bag with oxygen flow of 8 litres per minute. The patient’s pupils were equal, round and reactive to light with 3 mm to 2 mm constriction. He had normal vestibulo-ocular and gag reflexes. Examination of the lung revealed crepitation at both lower lung areas and tachypnea. In addition, heart examination showed persistent tachycardia.
The patient was diagnosed with fat embolism syndrome which commonly occurs 48 hours after trauma or during surgical procedures. Although most patient are generally asymptomatic. And only a small number of patient exhibit signs and symptoms involving the lungs, brain and skin.
Doctors advised a CT of the brain without intravenous contrast.
The CT scan showed no evidence of acute intracranial hemorrhage, mass lesion or territorial infarction. An MRI protocol stroke assessment was performed two hours after scan. MRI findings showed multiple, scattered, small ill-defined high signal intensity lesions and restricted diffusion. After surgery the chest radiograph showed improvement. In addition, the transcranial Doppler ultrasound revealed microembolic signals for 30 minutes on the 1st, 3rd, 7th and 10th day after surgery. Doctors advised evaluation of right and left shunt by trasncranial Doppler ultrasound and echocardiogram with intravenous injection of agitated saline. The tests were performed on the 1st and 7th day. No abnormalities were seen.
Six days after surgery the patient appeared drowsy but he could open his eyes and was responsive to verbal stimuli. All other examinations were also unremarkable. Heparin was infused subcutaneously every 12 hours to prevent deep vein thrombosis. He was further referred to a physical therapist for early rehabilitation. He was discharged on the 7th day with stable vital signs.
References