Wearable electronics seem to be the “in thing” in engineering these days. It is no surprise since they have the advantages of being lightweight and easy to use. And it’s not a secret that scientists love a challenge!
The latest in these wearable devices promises to be a useful innovation. A team from the University of California San Diego has created a skin patch that can monitor blood flow via ultrasound signals.
Usually, blood flow ultrasounds depend on technician skills and they take a lot of time. However, this patch can be stuck on the skin or chest and can check the cardiovascular system for anomalies in blood flow, like poor circulation or blockages, so that they can be managed upon early detection.
This, of course, is a huge advantage, as materials science and engineering Ph.D. student (UC San Diego) and co-author of the study Sai Zhou explains:
“Just stick it on the skin, then read the signals. It’s not operator-dependent, and it poses no extra work or burden to the technicians, clinicians, or patients. In the future, patients could wear something like this to do point of care or continuous at-home monitoring. القمار ”
The ultrasound device
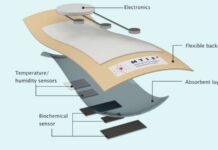
According to the study published in Nature Biomedical Engineering, the patch is a sheet of polymer containing multiple ultrasound transducers. Moreover, the tiny transducers are each connected to a computer, creating a system called a phased array. شرح موقع bet365
This system enables the patch to take two types of ultrasounds by focusing its beams in different ways.
The first type is based on synchronizing all the transducer beams in one area. Consequently, the device acts as a powerful ultrasound machine that can detect blood flow 14 centimeters deep into the skin.
The second type of ultrasound is even more unique. The individual transducers can be programmed to send signals to areas not directly beneath the patch. تعلم اسرار الروليت According to Professor Sheng Xu from the UC San Diego Jacobs School of Engineering, this technology is very difficult to create with wearable devices.
“If you want to sense signals at a different position, you have to move the sensor to that location. With this patch, we can probe areas that are wider than the device’s footprint. This can open up a lot of opportunities,” he says.
Source: Nature Biomedical Engineering
http://dx.doi.org/10.1038/s41551-021-00763-4