Case Presentation
A 24-year-old male was admitted to the emergency room with complaints of dyspnea that had progressively gotten worse throughout the past week. The patient’s family history and medical background were unremarkable. However, it was discovered that in the two weeks before the hospital admission, he had been consuming 8 to 10 cans of energy drinks each day (3.5 to 4 L/d). Three days after his first energy drink, he claimed to have experienced fatigue and dyspnea. During a physical examination, orthopnea, bilateral diffuse rales, and 2+ pretibial edema were all present.
Investigations
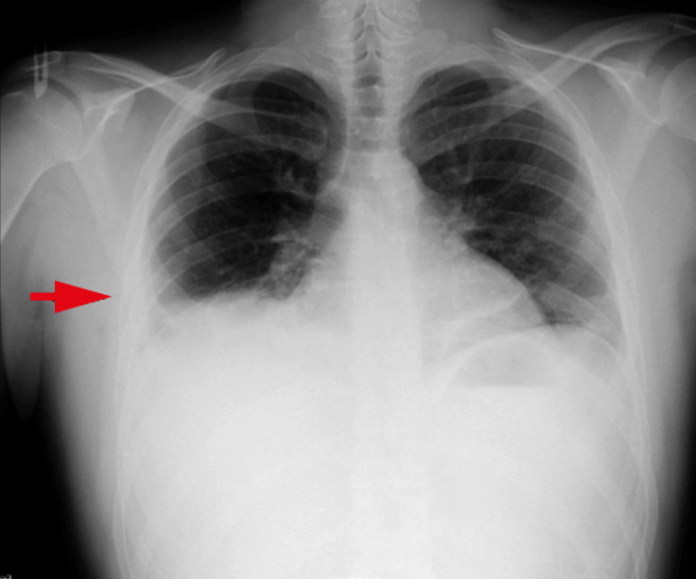
The electrocardiogram (ECG) revealed sinus rhythm, a heart rate of 110 beats per minute, and T-wave inversion in leads V4 to V6. A consolidated area in the right lower quadrant was seen on the chest X-ray. Computed tomography of the thorax showed pleural effusion and pulmonary edema. Left ventricular echocardiography revealed a left ventricular ejection fraction of 25%, end-diastolic diameters of 62 mm and an end-systolic diameter of 52 mm, an interventricular septum of 7 mm, and a posterior wall of 6 mm, as well as dilated left ventricular dimensions and global left ventricular hypokinesia
Both the size and functionality of the right ventricle were normal. After receiving a diagnosis of acute heart failure, the patient was admitted to the hospital. Furthermore, after diuretic treatment and symptom relief, the etiologic investigation was carried out. Coronary angiography showed that the coronary arteries were healthy. A cardiovascular MRI was performed two months following the diagnosis. It showed a cardiac output of 4.3 mL, an end-diastolic volume of 229 mL, an end-systolic volume of 169 mL, an interventricular septum of 7 mm, and an ejection percentage of 26%. The systolic function was also diminished, and the left ventricle was dilated. There was no pathological improvement found.
In cine imaging, right ventricular functions were normal. At the control visit six months later, there was no improvement in the echocardiographic data.
Discussion
Overconsumption of energy drinks has been linked to grave cardiovascular and neurological problems. There have been various reported seizure cases from a neurological perspective. The most often reported cases involving the cardiovascular system include palpitations, arrhythmias, and coronary events.
The maximum daily caffeine intake is 400 mg/d, with caffeine levels of 4 g/d and 10 g/d deemed hazardous and deadly, respectively. Guarana, another low-amount component, has been utilized as a heart stimulant since ancient times. More caffeine than coffee beans is found in guarana, which also contains xanthine alkaloids, including theobromine and theophylline. However, L-carnitine has been proven to lessen angina and ventricular arrhythmias, whereas taurine has been demonstrated to cause atrial and ventricular arrhythmias by reducing the action potential. Together, these two amino compounds are present in energy beverages and have opposite effects.
The effects of energy drinks can be amplified by alcohol and other concurrent drugs. The half-life of caffeine is extended by 72% when combined with alcohol.
This patient was a social drinker. He did not report the use of concurrent vasospastic causes like cocaine, though. Hypertrophic cardiomyopathy and Prinzmetal’s angina were ruled out as diagnoses.
After the acute infectious phase, an improvement in heart functioning is typically anticipated.
The patient underwent 96 hours of rhythm Holter monitoring. Dysrhythmia couldn’t be found. However, his admission ECG was in sinus rhythm, and at the 6-month follow-up, there had been no change in ejection fraction despite rate control and the best medical care. Endomyocardial biopsy, the gold standard in the diagnosis of cardiomyopathy, could aid in the differential diagnosis.