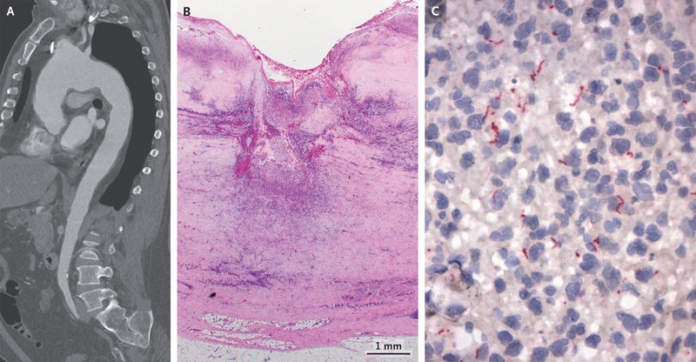
Syphilitic aortitis with left upper back pain
Aortitis is described as an inflammation of the aorta and is characterized by a cluster of large-vessel diseases that may have various or unknown etiologies. The inflammation is most commonly caused by infections or immunologic or connective tissue disorders. However, the inflammation can also occur in response to an injury or trauma. Additionally, it is significant to rule out vasculitis because the primary treatment for vasculitis is immunosuppressive therapy and that can aggravate the infectious process.
Inflammation of the aorta can further cause aortic dilation which may further result in aortic insufficiency. It can also cause fibrous thickening of the aorta and ostial stenosis of major branches that may result in reduced or absent pulses, in addition to low blood pressure and absent pulses in the upper extremities. This may possibly be because of central hypertension because of renal artery stenosis.
Similarly, based on the other vessels involved, it may cause ocular disturbances, claudication, neurologic deficits and other vascular impairments. Infections of the aorta may include viral infections, eg, herpes, hepatitis B and C and varicella-zoster virus, fungal infection, eg, aspergillus, mucormycosis, tuberculosis, Neisseria and syphilis as with this case. This article describes the case of a 61-year-old man who presented to the emergency with a 2-day history of left upper back pain which was diagnosed as syphilitic aortitis.
Case study
A 61-year-old male patient presented to the emergency with a complaint of left upper back pain with a history of 2 days. The patient’s physical examination and vital signs were within normal range. Doctors further advised a CT scan which showed cervical and thoracic spine, findings of which were consistent with a degenerative spinal disease with aneurysmal dilatation of the aortic arch, descending the thoracic aorta.
The patient was further referred for a CT angiography which showed an aneurysmal dilatation of the aortic arch and descending thoracic aorta. The dilatation of the ascending aorta measured 4.7 cm in diameter, whereas 5.5 cm in diameter for the aortic arch and 3.8 cm in diameter for the thoracic aorta. However, there were no observable signs of aortic dissection or rupture. The aneurysm was surgically repaired with a graft because of the high risk of rupture because of the size of the aneurysm and its rapid expansion which also caused pain in the patient’s back.
The patient was further referred for a pathological examination, findings of which were consistent with necrotizing aortitis and transmural neutrophilic and lymphoplasmacytic infiltrates. The immunohistochemical analysis further showed the presence of spirochetes and the rapid plasma reagin titer was elevated to 1:8. Moreover, for further evaluation, the patient was referred for a fluorescent treponemal-antibody absorption test that was reactive. The 61-year-old was negative for HIV. Based on these findings, doctors diagnosed the patient with syphilitic aortitis and treatment with penicillin G was initiated.
Doctors discharged the patient on the 8th postoperative day when he complete the antimicrobial therapy course [1].
Aortitis was first described in 1905
Ophthalmologist Mikito Takayasu first described aortitis in 1905 in a 21-year-old Japanese woman who presented with a peculiar retinal arteriovenous anastomosis. Onishi later described a patient with similar fundoscopic findings and absent radial pulses. Whereas an Italian pathologist, Giovan Morgagni reported the first case with signs and symptoms of Takayasu arteritis. In 1948, another condition characterized by absent pulses accelerated carotid sinus reflex, and peripapillary arteriovenous anastomosis was described by Shimizu and Sano, and was referred to as the “pulseless disease”. Later in 1964, the name “Takayasu’s disease” was coined by Caccamis [2].
Presentation
Many patients with aortitis report ischemia of the upper extremities which may present with claudication or numbness of the arm at the time of disease. However, claudication of the lower limbs is a less common symptom. Aortitis is also characterised by neurologic symptoms that are caused by a decrease in cerebral blood flow in the carotid and vertebral arteries. The neurologic symptoms may include dementia, stroke, transient ischemic attack, convulsion, headache, orthostasis, syncope and vertigo. Additionally, visual impairment is most often bilateral because of central retinal hypoperfusion. Whereas 48% of the patients with vertebral artery involvement and 40% with common carotid artery involvement present with visual aberrations.
Interestingly, in a minority of the cases of syphilitic arteritis, the lesions were also found to resemble erythema nodosum or pyoderma gangrenosum on the lower extremities. Interestingly, pyoderma gangrenosum is a common finding in Japan, whereas erythema nodosum is more commonly found in the United States and Europe. In some cases, the narrowing of the arteries may also result in angina pectoris which may lead to myocardial infarction, heart failure and sudden death. Studies have further shown that patients with aortitis may present with atypical symptoms that may cause a delay in diagnosis. “Red flags” for aortitis may include atypical features such as unexplained lower back pain or pain in the lower extremities. However, in this case, the patient presented with the complaint of upper back pain.
References
- Miller, S.A. and Ladich, E.R., 2022. Syphilitic Aortitis. New England Journal of Medicine, p.e55.
- Pearlman, J.D., 2019. Aortitis. Medscape.



