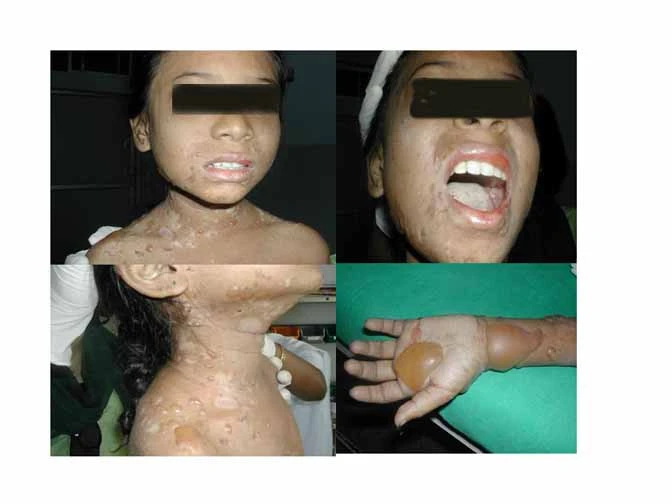
This article describes the case of a 13-year-old girl who presented with unusual Systemic Lupus Erythematous (SLE).
She presented with complaints of recurrent fever and associated fatigue and arthralgia. She also reported hair loss and had red bullous lesions on her face and neck. According to her, the lesions were 2 months old. She also complained of an episode of generalized seizure prior to her presentation.
On examination, the doctors saw bullae and vesicles over her face, neck, back and even in the groin. They were in different stages of eruption. Those with crusts represented the older ones. However, for completely healed lesions, doctors did not notice any crusting or scarring. Her Nikolsky’s sign was negative. Moreover, there was no Reynaud’s phenomenon. Her abdominal examination showed no palpable organs and hepatosplenomegaly. Her fundoscopic examination was also normal. There were no signs of hypertensive retinopathy. Furthermore, her neurological assessment was also normal.
Investigations revealed a haemoglobin level of 90g/L. Her ESR was 55mm at one hour and her CRP turned out negative. The complement products, C3 and C4, were low. Tests also revealed an elevated ANA titer and increased dsDNA. Furthermore, urine microscopy revealed microscopic hematuria and protein loss, indicative of renal insufficiency. Her 24-hour urinary protein came out to 20mg/m2/hr. Her CSF analysis did not show any anomaly with all the pressures observed within the normal range.
Skin Biopsy and Diagnosis of SLE
Doctors performed a biopsy of skin lesions. They found dense inflammatory infiltrate in the dermis near the dermo-epidermal junction. Similarly on direct immunofluorescence, they found antibody complexes (including IgA, IgG, IgM and C3) at the epidermal basement membrane. Doctors diagnosed her with bullous systemic lupus erythematosus with renal involvement. However, based on renal compromise, they did not proceed with a renal biopsy.
Bullous SLE: An insight
Bullous SLE is characterized by bullous lesions on the skin. These lesions represent non-scarring eruptions which on histology show dense neutrophilic infiltrate in the upper dermis. Moreover, these lesions show characteristic antibodies deposited at the basement membrane of the epidermis, on direct immunofluorescence. The antibodies include IgG, IgM, IgA and C3 and can deposit in both linear and granular patterns. The important thing to consider here is that less than 5 percent of SLE patients develop these bullous skin lesions or develop isolated bullous SLE.
Patients with bullous SLE can also have circulating antibodies against collagen type 7, as demonstrated by indirect immunofluorescence. These antibodies bind collagen type 7, the predominant anchoring protein that binds the epidermal basement membrane to the dermis. Thus, by affecting the pivot protein, these antibodies lead to sub-epidermal blister formation.
Differential Diagnosis
Differentials for bullous lesions include bullous pemphigoid, dermatitis herpetiformis and pemphigus Vulgaris etc. However, bullous SLE can be diagnosed based on histological features such as neutrophilic infiltrate in the upper dermis near its junction with the epidermis and characteristic antibody patterns at the epidermal basement membrane. Another striking feature confined to bullous SLE alone is its response to dapsone. It responds pretty well to dapsone and complete resolution of lesions is seen in most of the cases. Some cases may additionally require cytotoxic agents like cyclophosphamide and azathioprine etc. Cyclophosphamide is especially effective against dapsone-resistant bullous SLE.
Treatment of Bullous SLE
For bullous SLE, dapsone remains the first line of treatment. Almost all the cases result in complete remission. The new lesions stop developing in as less as 12-48 hours and all the older lesions resolve within a few days as well. Only small doses (25-50 mg/day) are required for treatment with dapsone. Other drugs that can be employed include methotrexate and cyclophosphamide etc. Methotrexate shows good efficacy against skin lesions whereas, in patients that do not respond to dapsone, cyclophosphamide becomes the drug of choice. Anyhow, the disease usually remits within one year.
Our patient did not have the antibody against type 7 collagen on histology. However, she had renal disease and CNS involvement in addition to bullous SLE. Thus, doctors started her treatment with dapsone and prednisolone. They additionally gave her cyclophosphamide, 500mg/m2, as an infusion for her skin lesions. Fortunately, the treatment garnered positive results within a week. However, upon the parents’ request to try alternative medicine too, doctors discharged the patient.