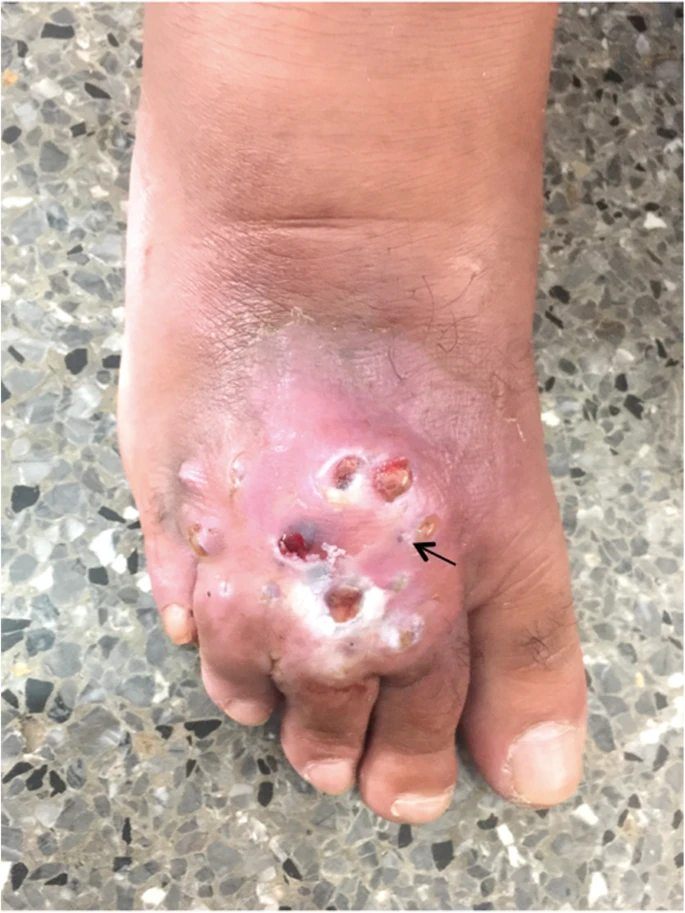
A 64-year-old man developed a fistulated nodule on the dorsum of his right foot that discharged dark-coloured grains, a second time around.
He first presented to the hospital with a similar complaint nearly 10 years ago. A nodule appeared on his right dorsal foot that became inflammatory and turned into a polyfistulized discharging tumour. Back then, he did not have any history of foot injury or travel to an endemic area. Doctors diagnosed him with Madurella mycetomatis infection of the foot and started his treatment with itraconazole. After receiving it for nearly two years and not showing significant improvements, the doctors replaced itraconazole with terbinafine 500mg/day. Moreover, they debrided the affected areas. The result turned out good and the lesion resolved completely.
Madurella makes a comeback!
This time, the nodule appeared 6 months ago in the same location. It was attached to the underlying tissue and had seropurulent (also hematic) discharge along with dark grains coming out from various openings. Doctors also noticed enlarged inguinal lymph nodes on the right side. However, the patient did not have a fever or any signs of malaise.
Doctors included fistulized osteitis, profound mycosis, leprosy and cutaneous metastatic lesion on their list of differentials. Hence, they subjected the lesion to multiple investigations to reach a definitive diagnosis. The X-ray was normal. On biological examination, the nodule showed no signs of bacterial infection. They also performed a biopsy during which they noticed seropurulent discharge along with blackish grains coming out from the lesion. This finding suggested mycetomatis.
Culture Investigation and diagnosis of Madurella mycetomatis
Doctors analyzed the biopsy specimen for histology. It revealed an inflammatory cell reaction. Although bacterial analysis turned out negative, analysis of the specimen for possible mycosis dropped significant findings. First, on direct microscopic examination, doctors clearly observed septate hyphae containing chlamydoconidia. Second, fungal culture on Sabouraud agar (for three weeks) revealed Madurella mycetomatis.
After confirming the diagnosis, doctors performed an MRI to determine the extent of the disease. Imaging showed involvement of flexor and extensor tendons. However, the disease had not infiltrated the underlying bone.
What is the disease About?
Mycetoma is a granulomatous disease that affects the cutaneous and subcutaneous tissues. The causative agent is usually a filamentous bacteria or a fungi that inhabits the soil. It gets into the body through vegetative trauma such as a thorn prick. This explains why the disease is more commonly seen in farmers and other people who work out in fields.
Epidemiologically, the disease peaks in tropical and subtropical regions. It mostly affects young adults and shows a predominance in male population. Females rarely develop the disease. The classic manifestations include a triad of painless swelling that becomes fistulised and discharges seropurulent material and blackish grains. The purulence reflects a super-added infection that often leads to fatal sepsis. Although the disease usually involves the foot, it can also affect arm, forearm, head and thorax etc.
Pathophysiology and Diagnosis
The disease occurs in four phases. It starts off with the incubation period which usually takes around 6 months, as in our patient. Next, the patient develops pain and discomfort. In the third phase, a painless nodule develops that grows into an inflammatory lesion and emits seropurulent discharge in the fourth phase. The fistulation and blackish grains are characteristic of a parasitic cause. Hence, doctors use it to identify typical madurella infestation.
The diagnosis depends mainly on clinical manifestations. However, tests that can be used begin with direct microscopic examination. The tissue specimen is treated with KOH and seen under a microscope. Direct examination of the grains can help establish the etiology. Next, doctors can employ cultures and PCR based assays to determine specific species and establish appropriate treatment plans. Early treatment, nevertheless, is of paramount importance. If delayed, the disease spreads to involve the underlying bone and muscles causing widespread destruction.
Treatment of Madurella mycetomatis
The treatment for mycetomatis should be started as soon as possible to avoid amputation. Treatment in case of a bacterial infection (actinomycetoma) is usually less robust than for a fungal one (eumycetoma). Moreover, eumycetoma requires long term medical therapy (at least an year). For bacterial infections, doctors usually employ trimethoprim-sulphamethoxazole. However for eumycetoma, doctors use various antifungals such as ketoconazole, itroconazole, amphotericin B etc. after identifying the exact species through PCR and cultures.
Our patient was treated with terbinafine 750mg/day because of its positive results during the previous attack. Moreover, doctors did tumorectomy to reduce the size of lesion and improve the efficacy of medicine. One thing however that we need to keep in mind is that relapses are common. Thus, doctors should keep the patient on follow-up even after complete remission. The disease can show up again after as long as 10 years, as in our case. Hence, prevention becomes the best policy against mycetomatis. Wearing protective shoes when working out in fields and farms can make a significant difference.