One week’s history of pain, redness, and swelling in the fifth finger led to a diagnosis of an otherwise concealed disease.
A 42-year-old woman came to the outpatient department with complaints of swelling and pain in her left hand’s fifth finger for the past 1-week. The patient recalled no trauma or previous infection. However, the history revealed that she is a known case of systemic lupus erythematosus for which she was being treated with mycophenolate mofetil and prednisone.
Physical Examination:
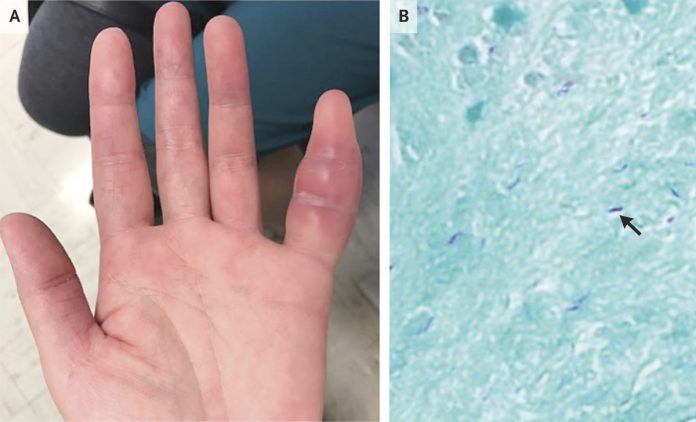
On examination, the patient’s affected finger was warm, erythematous with soft tissue swelling. The findings were most prominent between the proximal and distal interphalangeal joints, sparing the fingertip (Panel A).
Imaging Studies:
Both plain Radiography and magnetic resonance imaging (MRI) confirmed the findings of physical examination, i.e., soft tissue swelling. However, no bony abnormalities were appreciated on the imaging studies.
Histopathological evaluation of the specimen of the deep dermis after Fite staining revealed numerous acid-fast bacilli (Panel B, arrow). Tissue culture grew Mycobacterium tuberculosis.
Chest radiography was unremarkable (normal).
Since the patient was taking immunosuppressive drugs for her SLE, she had undergone a routine purified protein derivative (PPD) skin test, for the detection of tuberculosis, before starting immunosuppressive therapy; however, the result was negative.
Upon further inquiry, she revealed that her husband had recently traveled to China, and since his visit, he had been suffering from a cough.
When his cough was evaluated, he was diagnosed with active pulmonary tuberculosis.
This history of close contact with a TB patient rang the bells, so she was started on a four-drug antituberculosis drug regimen for a total of 9 months. The antituberculosis drugs resolved her symptoms completely.
The history of close contact, along with immunosuppressive therapy for SLE and the resolution of symptoms with antituberculosis drugs, confirmed that the patient was suffering from a rare extrapulmonary manifestation of tuberculosis.
References
Jennifer Mandal, M. a. (2018, September 20). Tuberculosis of the Finger. Retrieved from The New England Journal of Medicine: https://www.nejm.org/doi/full/10.1056/NEJMicm1800879