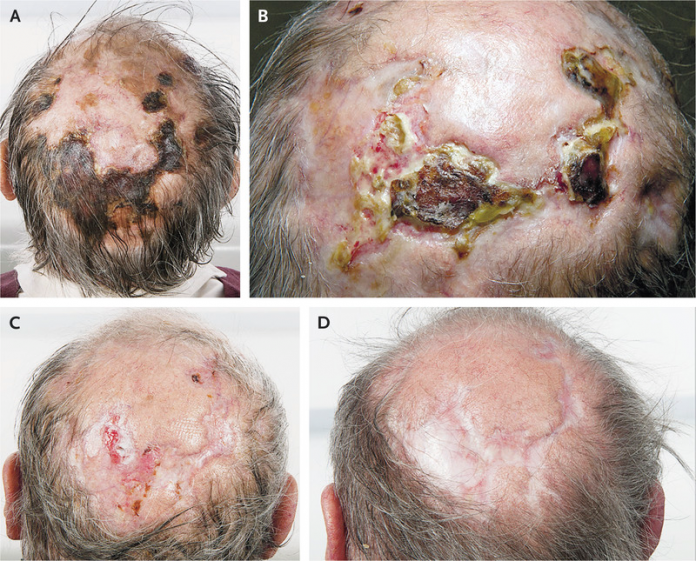
A 74-old man presented with symptoms of scalp ulceration, jaw claudication and a 3-month history of headache. The scalp ulcerations were seen to be worsening over time. In addition to these symptoms, the patient did not report of any visual loss or polymyalgia rheumatica. On examination, the scalp had necrotized areas. However, both the temporal arteries were non-tender, even though they were difficult to palpate.
According to the patient’s lab tests, the erythrocyte sedimentation rate and C-reactive protein were 64 mm per hour and 45 mg per litre. Based on clinical examination and test results, the patient was diagnosed with giant cell arteritis.
Giant cell arteritis
Common symptoms of giant cell arteritis include symptoms of polymylagia rheumatics, fever, visual changes, jaw claudication and headache. Test results usually reveal an erythrocyte sedimentation rate typically greater than 50 mm/hour. The first case of scalp necrosis was reported in 1946. Necrotic changes in giant cell arteritis are considered to be a secondary manifestation from occlusive inflammation of the artery, to tissue ischemia. Lesions heal completely in most cases with steroid therapy. However, even though scalp necrosis is a very rarely encountered complication of giant cell arteritis, it is quite well-documented. In addition to this, the condition requires prompt recognition and an initiation of steroid therapy.
The first-line treatment of scalp necrosis as a complication of giant cell arteritis is steroid therapy. The patient was started on treatment with glucocorticoids, 60 mg of prednisolone once a day and was administered with topical dressings, daily. The patients symptoms decreased considerably over the next few months and scalp lesions started to heal.
The prednisolone dose was tapered off until it reached 20 mg per day, by 10 mg each month. Moreover, until the lesions healed completely, the dose was tapered more slowly. The medications were then discontinued. Early recognition and treatment is important for scalp necrosis caused as a complication of giant cell arteritis. If left untreated, it can lead to potentially life-threatening complications.
References
Akram, Q., & Chinoy, H. (2016). Scalp necrosis associated with giant-cell arteritis. New England Journal of Medicine, 374(6), e6.