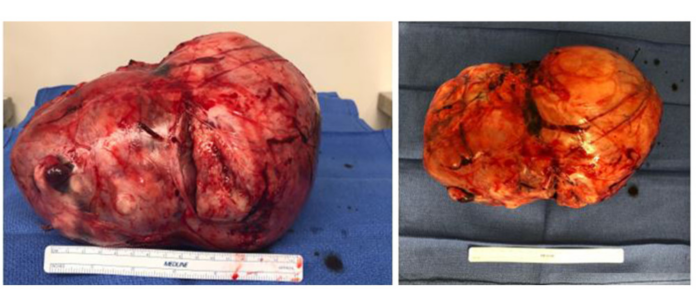
Recurrent hypoglycemia caused by a solitary fibrous tumour
This article describes the case of a 94-year-old man who presented to the emergency department for evaluation after multiple falls within 24 hours. Doctors diagnosed the patient with a massive abdominal tumour. His medical history did not reveal any signs of fever, chills, recent medication changes, abdominal pain, cough or malaise. He also didn’t have any recent medication changes that would lead to disorientation and falls. الربح الحقيقي In addition, the patient did not have a past medical history of falls either and was generally physically active. He also played gold regularly.
The patient experienced atrial fibrillation in the past and was put on metoprolol and anticoagulation. He also had a history of a large solitary fibrous tumour that was managed conservatively by his primary care physician with serial imaging. The patient did not have a known history of diabetes mellitus and was not taking any medications that would lead to hypoglycemia.
Previously. the doctors had referred the patient for a core-needle biopsy and diagnosed the tumour. At the time the tumour measured, 9.1 x 13.5 x 11.4 cm on CT scan. At the time the doctors did not pursue surgical resection because of the patient’s age and the nature of the tumour. Another reason surgery wasn’t pursued was because the tumour was asymptomatic.
Investigations and findings
On physical examination, the patient appeared to be mildly anxious and hypertensive. His height was 175 cm, whereas his weight was 72.5 kg. Further examination of the abdomen was significant for a contender, large, palpable, left-sided abdominal mass. On the way to the hospital, the patient’s blood glucose was 45 mg/dl which normalised after administration of 1 ampule of IV glucose.
By the time the patient reached the emergency department his blood glucose level had fallen to 75 mg/dl and shortly after admission to 38 mg/dl. Other accompanying symptoms included confusion and gait disturbances. Doctors advised a CT scan of the abdomen which showed a well-defined, large, complex mass in the left upper quadrant. The tumour had grown significantly in a year, since the initial diagnosis. During the patient’s hospitalisation, the patient suffered from multiple hypoglycemic episodes, especially at night, while sleeping and when oral feeding was halted. He was, therefore, put on a complex carbohydrate diet with oral and intravenous dextrose for symptom control. كيف تلعب بينجو
Extensive laboratory workup was done which showed low levels of fasting insulin and C-peptide. In addition, contrast-enhanced CT scan and MRI were consistent with the initial diagnosis of a solitary fibrous tumour. The patient opted for a course of surgical resection because the hypoglycemic symptoms could not be controlled with conservative treatment. قانون لعبة البوكر Immunohistochemistry of the tumour confirmed the diagnosis of a solitary fibrous tumour. The patient experienced post-operative complications including prerenal azotemia, narcotic-induced delirium and respiratory depression. He achieved normoglycemia 24 h after the surgical resection and was discharged to inpatient rehabilitation. Subsequently, the patient was discharged without any further reported hypoglycemic episodes.
Source: American Journal of Case Reports



