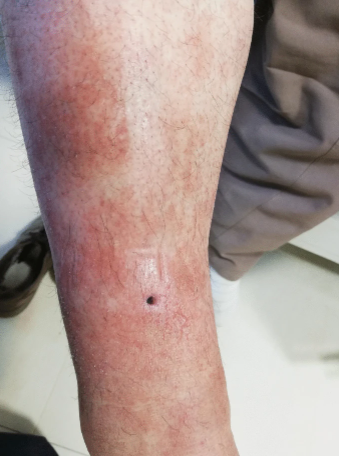
Case Presentation
A 46-year-old Kurdish male mosque worker by profession; presented to the clinic with complaints of pain in various parts of his body, including the right leg, lower back, right hand, and neck. He mentioned experiencing symptoms such as redness in his right buttock and thigh, in addition to skin lesions that appeared on his left shin. These symptoms started gradually and progressively worsened over a period of three weeks, causing stiffness in the affected areas. He also complained of difficulty and pain in walking which had significantly impaired his ability to move around normally.
The patient had a history of cervical disc herniation surgery for cervical disc herniation, which occurred two years prior to his presentation. After the surgery, the doctors treated him with acetaminophen and chlordiazepoxide, but unfortunately, there was no improvement in his symptoms. He also had a history of smoking, having consumed 20 packs of cigarettes per year. However, he quit smoking eight years ago. The patient’s family history was positive for diabetes mellitus and hypertension. The patient also admitted to using a small amount of inhaled opium.
Examination
During the examination, the patient’s vital signs were stable. A surgical scar from his previous neck surgery was visible, and the patient reported experiencing pain during neck movements. Moreover, the Lasegue test, which evaluates nerve irritation in the leg, was positive for the patient’s right leg. He also complained of pain in his right buttock. Upon examination, doctors observed an area of redness with firm swelling measuring 8 × 15 cm.
Investigations
The results of the preoperative magnetic resonance imaging (MRI) scans revealed the following findings: cervical lordosis with spondylolysis changes, along with posterior bulging disks in the C3-C4, C4-C5. Moreover, the C5-C6 levels were causing compression of the thecal sac. There was also evidence of myelomalacia in the cervical cord at the C4 level. Additionally, there was a hemangioma in the T1 vertebral body.
The pelvic MRI showed multiple small areas of low signal intensity in both femoral heads, which indicated benign sclerotic lesions. On the other hand, the brain MRI showed no abnormalities. The MRI of the patient’s back revealed a decrease in lordosis and dehydration, as well as bulging in the L4-L5 level and a bared base observed in the L4-L5 and central L5-S1 regions.
A triphasic whole-body scan demonstrated enteropathy involving various locations. This included the upper part of the right sacroiliac joint, the left anterior superior iliac spine, the right pelvic brim, both patellae, the right tibia tuberosity, and both medial malleoli.
Osteopoikilosis: A Summary
Osteopoikilosis is a rare bone disease, which was first described by Albers-Schonberg in 1915. It has an estimated prevalence of 1 per 50,000 individuals. Osteopoikilosis is classified as an autosomal dominant osteosclerotic dysplasia and is characterized by a unique radiological appearance. It is also known by other names such as disseminated condensing osteopathy, spotted bone disease, and osteopecilia. There are three forms of the disease: speckled type, striated type, and mixed type. Autosomal dominant osteopoikilosis is associated with various mutations in the LEMD3 gene. The primary pathology of this condition includes disruption in the bone maturation process, classifying it as a form of bone dysplasia.
The Buschke-Ollendorff syndrome, which often occurs simultaneously with osteopoikilosis, involves skin involvement. Skin biopsies and pathological examinations reveal increased fibroelastins in the middle and deep dermis. Rare complications associated with this syndrome include spinal canal stenosis, dacryocystitis, and malignant transformation.
Bone densitometry typically shows typical results. The condition is characterized by the presence of elastic connective tissue in this widespread syndrome. In the current case, the patient presents with multiple disc lesions in the spine, extensive multifocal skin lesions, positive findings for dermatomyositis and multifocal enthesopathy, and accompanying neurological symptoms.
Discussion: Osteopoikilosis
Some studies have indicated that the disease is equally prevalent in men and women, while others have suggested a higher prevalence in men. There have been reports of this syndrome coexisting with other conditions such as dwarfism, dystocia, coarctation of the aorta, double urethra, spinal canal stenosis, tuberous sclerosis, scleroderma, dystocia, precocious puberty, endocrine disorders (such as diabetes mellitus), fibromyalgia, facial anomalies, reactive arthritis, discoid lupus erythematosus (DLE), familial Mediterranean fever (FMF), and psoriatic arthritis.
As seen in bone histopathology, the lesions seen in this condition are related to the lamellar osseous tissue containing the Haversian system, as well as focal condensation of compact lamellar bone in the spongy bone. The prevalence of bone involvement is as follows: phalanx (100%), carpal bone (97.4%), metacarpal (92.5%), toes (87.2%), metatarsus (84.4%), tarsus (84.6%), pelvis (74.4%), femur (74.4%), radius (66.7%), ulna (66.7%), sacrum (58.9%), humerus (28.2%), tibia (20.5%), and fibula (2.8%). The most common anatomical locations for bone involvement are the epiphysis or metaphysis regions of the long bones. Differential diagnoses for the disease include osteoblastic metastasis, primary bone tumours, mastocytosis, tuberous sclerosis, synovial chondromatosis, osteopathia striata, and melorheostosis. Technetium-99m bone scans usually do not show any specific abnormalities and are often normal. However, the absence of irregularities in the scan does not definitively rule out a diagnosis of osteopoikilosis. To date, only four cases of osteopoikilosis with abnormal bone scans have been reported.