Retroperitoneal liposarcoma and ischaemic colitis
This article describes the case of a 76-year-old woman who presented with intermittent colicky pain in the left iliac fossa. She also complained of diarrhoea and rectal bleeding. However, there was no history of weight loss, tenesmus and melaena. Her medical history was consistent with hypothyroidism and gallstone pancreatitis. Examination showed that the patient had low-grade fever and tenderness in the left iliac fossa. Further investigations showed raised lactate levels, white cell count and C-reactive protein. Whereas stool culture was negative for any bacterial growth. Doctors diagnosed the patient with retroperitoneal liposarcoma.
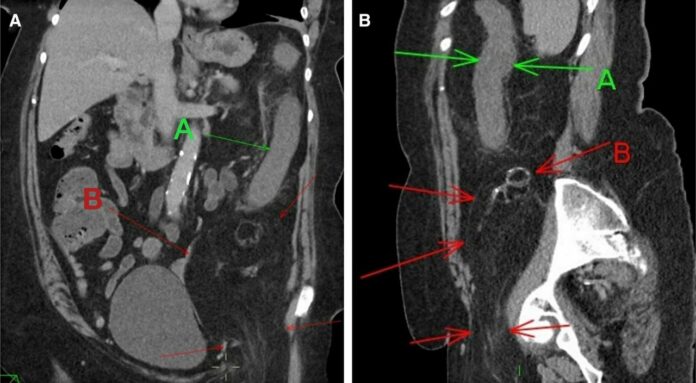
For further evaluation, the patient was referred for CT abdomen and pelvis which showed findings of oedema of the wall of the descending colon, a large intra-abdominal fatty lesion and small calcifications in the left iliac fossa that extended through the inguinal canal. She was given intravenous antibiotics and fluids, however, despite it, she reported minor rectal bleeding. Doctors further advised a flexible sigmoidoscopy which showed the presence of neutrophils infiltrating the surface of the epithelium and congestion of the lamina propria.
The findings were consistent with the diagnosis of ischaemic colitis, caused because of an extrinsic compression of vasculature by the liposarcoma
The patient underwent laparotomy and excision of the left retroperitoneal mass, measuring 140 mm x 70 mm x 70 mm. The biopsy was consistent with viable adipose tissue with scattered stromal nuclear atypia. This led to the diagnosis of liposarcoma stage pT3 which resulted in the secondary ischaemic colitis.
Patients presenting with diarrhoea, mild rectal bleeding and colicky abdominal pain are common in both general medicine and surgical admissions. However, ischaemic colitis is an uncommon cause with an incidence of only 22.9 cases per 100,000 presentations in a year. It is often related to hypotension and cardiovascular diseases. Therefore, it is important for clinicians to investigate secondary causes, for example, a tumour compressing the vasculature. Especially in cases where there is no history of hypotension.
Source: BMJ