Eosinophilic granulomatosis with polyangiitis
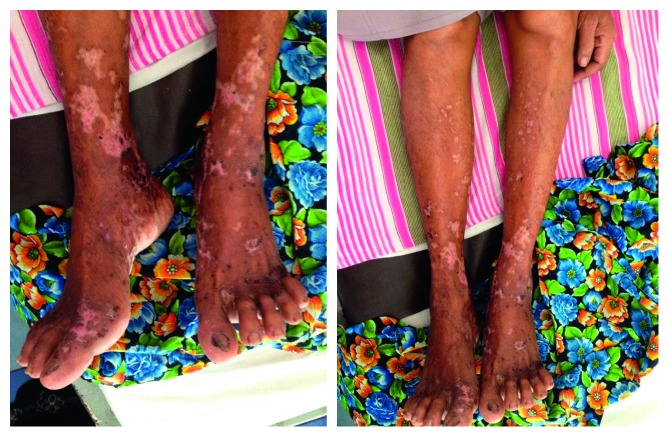
This article describes the case of a 49-year-female patient diagnosed with eosinophilic granulomatosis with polyangiitis. The patient presented to the hospital with a 2-week history of skin rash on the lower limbs. She was otherwise healthy but developed a skin rash that began as a painful vesicle on the left food. The vesicle enlarged in size and crops of new vesicles appeared on bilateral lower limbs. Similarly, the vesicles enlarged forming a bullae which then ruptured, causing scarring,
Some vesicles enlarged to bullae and then ruptured and healed with scarring. However, she did not complain of any weakness in her muscles or difficulty walking. Examination was significant for progressive bilateral ankle oedema and frothyuria. She also complained of reduced urine output and hematuria, in addition to other symptoms including low-grade fever and generalised malaise. Her medical history revealed wheezing for which she was prescribed inhalers. Although, there were no signs of epistaxis, sinusitis or cough. There were no joint symptoms, ulcers, gangrene or gastrointestinal symptoms.
Examination and investigations findings
Lower limb examination showed an erythematous rash with small blisters measuring 2 to 4 cm. In addition, hypo-pigmented lesions with marked involvement were also seen around the ankle. A few small, hyperpigmented lesions were also present on the palmar surface of the patient’s left hand. There were no evident lesions in the trunk, face or mucosa. Neurological exam showed reduced bilateral lower limb reflexes and a sensory impairment at the level of the knee. However, with no motor weakness. Vibration and joint position sense was intact. Upper limbs did not show any neurologic deficit. Other systemic examinations were also normal.
Further investigations showed an elevated C-reactive protein level. And her skin biopsy showed leukocytoclastic vasculitis with few perivascular eosinophilic infiltrates. Doctors diagnosed her with eosinophilic granulomatosis with polyangiitis. The patient was discharged on low-dose prednisolone and oral azathioprine after achieving complete remission. She showed improvement 4 weeks after discharge.
References
A Rare Case of Eosinophilic Granulomatosis with Polyangiitis Associated with Cryoglobulinemia Presenting with a Bullous Skin Eruption of the Lower Limbs https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5822773/