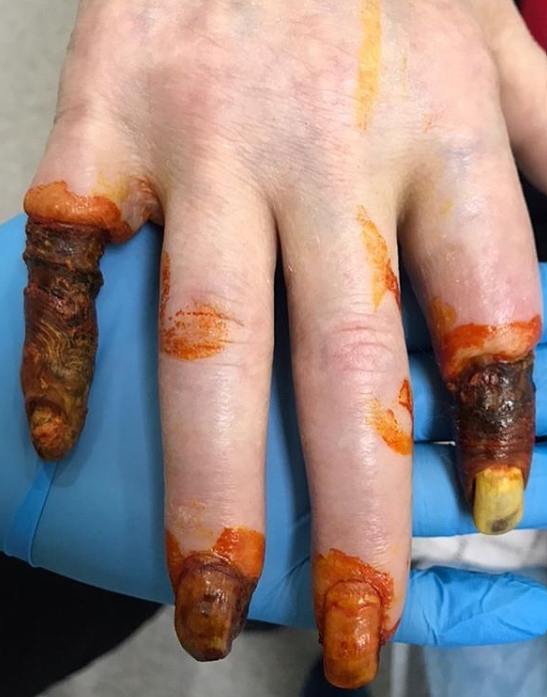
Gangrene Images
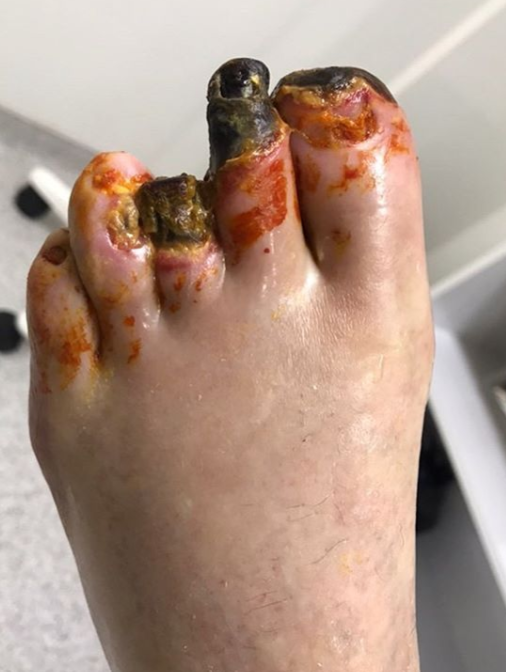
The attached pictures show gangrenous fingers and toes in a patient with type II diabetes mellitus along with a severe peripheral arterial disease.
Many of us are already aware of Diabetes due to its increased prevalence, but fewer people know about complications of diabetes if left untreated. Long-term untreated diabetes can have horrible consequences and can virtually affect all the main organs sooner or later. Vessels being one of the targets of prolonged hyperglycemia.
Gangrene occurs secondary to a decreased blood supply, ultimately leading to tissue destruction or necrosis. It can result due to multiple reasons: trauma, infection, wounds and some health conditions like diabetes, to count a few. It can be of three types:
- Dry gangrene
- Wet gangrene
- Gas gangrene
How is gangrene transmitted?
Gangrene forming as a result of diabetes is of mostly dry type, involving mostly the fingers and the toes. Due to prolonged hyperglycemia and ischemia, the blood supply to these parts is insufficient, therefore the tissue eventually dries up, darkens and mummifies. Not only diabetes but arteriolosclerosis, high cholesterol and smoking can be the culprits too.
The necrosed tissue becomes darker, harder, drier and cooler than the surrounding skin, with a clear demarcation between the gangrenous and the unaffected tissue. Dry gangrene, if left untreated can either complicate further leading to infections or the dead tissue can eventually fall off – autoamputation.
Patients with uncontrolled diabetes have a highly hyperglycemic environment, which makes it a suitable habitat for bacterial growth, hence wet gangrene can also be a complication.

Source: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5987754/
Why diabetics are advised closed footwear and special foot care?
The reasons are two-fold:
One being nerves, other being blood vessels.
Around 70% of the patients with diabetes face diabetic neuropathy, a condition which affects the peripheral nerves, especially of the legs and feet, rendering patient’s feet insensitive or less sensitive. This may result in unnoticed injuries. Also, because of the poor blood circulation secondary to peripheral arterial disease, the healing of those unnoticed wounds is negatively affected, thus causing non-healing ulcers, infections, gangrene, etc.
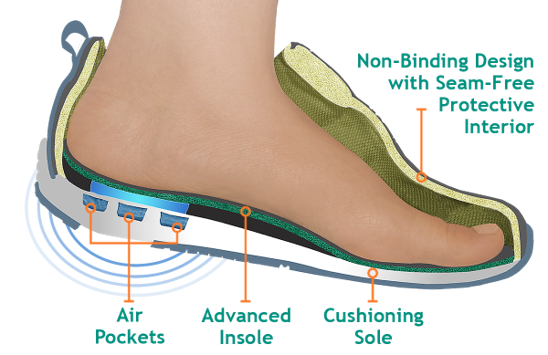
Therefore, with protective, non-binding, seam-free, spacious, closed and comfortable footwear, there are lesser chances of injury, hence fewer foot complications.
A thorough history and a proper physical examination is the first step to a fruitful treatment of dry gangrene.
Few tests may be necessary for the gangrene, such as a culture of the pus/scrapings from the wound, tissue culture, imaging studies.
Can gangrene be cured?
Optimal wound care and strict glycemic control are the building blocks.
Apart from hypoglycemic agents, other drugs may be required i.e. non-opioid analgesics or opioids for pain, anti-platelets drugs for blood circulation and lipid-lowering drugs like statins for dyslipidemia. Other non-pharmacological management strategies for improving blood circulation include exercises, intermittent walking, light massage of the affected limb, etc. Dietary modifications are a must!
Reperfusion therapy and surgical amputation are the options if the case is severe. The former is the option when the limb is ischemic but not yet necrosed. After gangrene, reperfusion therapy is of no use, therefore, surgical amputation is the treatment of choice for a rapid and smooth recovery. Although some patients do opt for autoamputation but that has a variable and a painful course with less rapid and incomplete recovery.
Are you an advocate of auto-amputation of dry gangrene or elective amputation?
References
Gangrene. (2019, January 15th). Retrieved from Diabetes.co.uk: https://www.diabetes.co.uk/diabetes-complications/gangrene-and-diabetes.html
Al Wahbi A. (2018). Autoamputation of diabetic toe with dry gangrene: a myth or a fact?. Diabetes, metabolic syndrome and obesity : targets and therapy, 11, 255–264. DOI:10.2147/DMSO.S164199
The Expert Committee on the Diagnosis and Classification of Diabetes Mellitus: Follow-up report on the diagnosis of diabetes mellitus. Diabetes Care 26:3160–3167, 2003