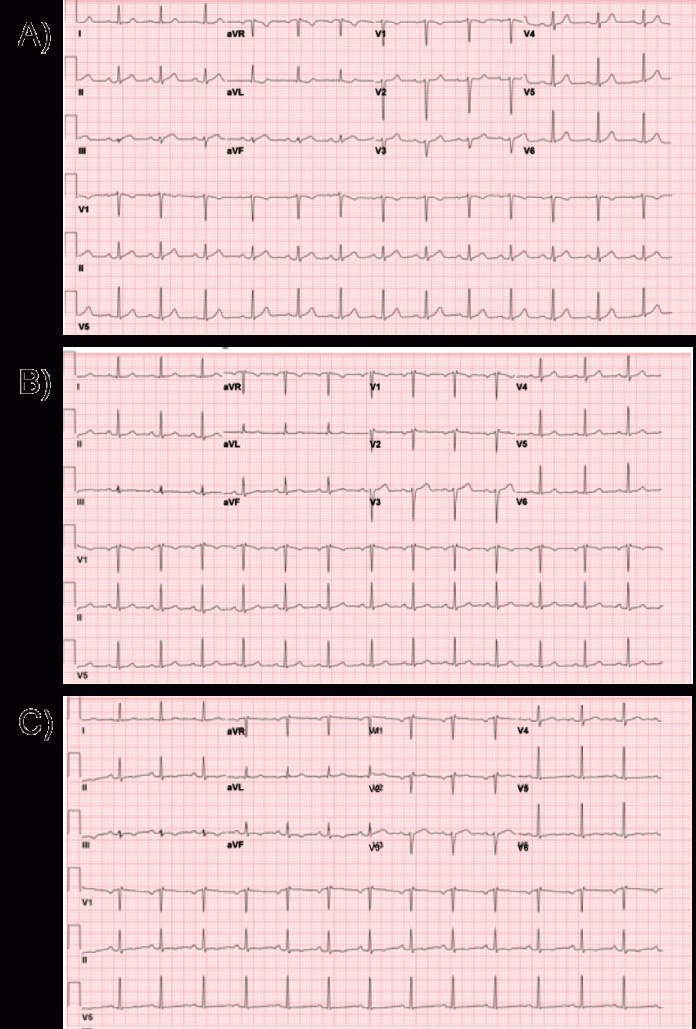
A 48-year-old woman, who was taking Lisdexamfetamine for attention deficit hyperactivity disorder, presents with sudden onset chest pain.
A 48-year-old woman, known case of ADHD (attention deficit hyperactivity disorder), presented to the emergency department with complaints of severe chest pain which awakened her at night. 888 sport In the ER, her heart rate was 88 and her blood pressure was 147/53. There was intermittent ventricular bigeminy. Although initially the troponin I was undetectable, after 6 hours, the levels elevated to 1.7 ng/mL, followed by a gradual decline.
She had started taking 30 mg of Vyvanse (lisdexamfetamine) PRN (as needed), 2 months prior to the presentation. Although during the past 2 months, she was not taking this medication regulary, in the last 3 days she took lisdexamfetamine once daily. Besides Vyvanse, her regular medications included famotidine and dexlansoprazole for gastroesophageal reflux disease.
The rest of the history was unremarkable. The patient was a non-smoker with no other chronic illnesses or illicit drug abuse. There was no history of premature coronary artery disease in the family.
In the ER, the doctors performed an electrocardiogram (ECG) during angina which showed normal sinus rhythm with <1 mm ST elevation in the inferior leads. However, the ECG readings obtained after the chest pain subsided showed ST-segment elevation. Later the same leads showed T wave inversion.
Thereafter, she underwent echocardiogram which showed normal global left ventricular wall motion and ejection fraction. الالعاب التي تربح المال
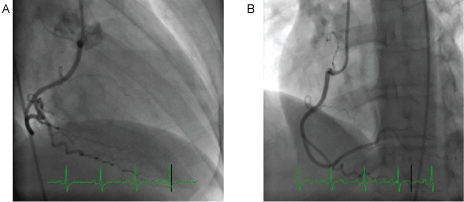
During cardiac catheterization, which was done to evaluate NSTEMI, angiographically normal vessels were observed. However, left ventriculography showed mid-inferior wall hypokinesis.
Cardiac magnetic resonance imaging (MRI) showed normal ejection fraction and left ventricular wall motion. Moreover, it showed absence of late gadolinium enhancement and increased T2 signal hyperintensity. روليت اون لاين
A computed tomography (CT) coronary angiogram was normal. The doctors advised the patient to discontinue Lisdexamfetamine. Since she discontinued the drug, she had no recurrence of chest pain for over a year after the initial presentation.
Lisdexamfetamine
Lisdexamfetamine, sold under the brand name, Vyvanse, is an amphetamine-derivative, prescribed for ADHD. It is a central nervous system stimulant which has abuse potential. The common side effects include anxiety, irritability, dizziness, decreased appetite, gastrointestinal complaints including diarrhoea, upper abdominal pain, nausea, and vomiting. Serious adverse effects include visual changes, stroke, heart problems including high blood pressure, chest pain, and dyspnoea, and neurological abnormalities including seizures.
Prior to prescribing Lisdexamfetamine, a thorough history is indispensable especially the patient’s past medical history and his medications. For instance, patients who are taking or have taken an MAO inhibitor in the past 14 days, should not use Vyvanseto avoid fatal drug-drug interaction.
Source: Gandhi HV, Skolnick AH, Reynolds HR (2017) A Case of Coronary Artery Spasm Associated with Lisdexamfetamine Use. Int J Clin Cardiol 4:095. doi.org/10.23937/2378-2951/1410095



