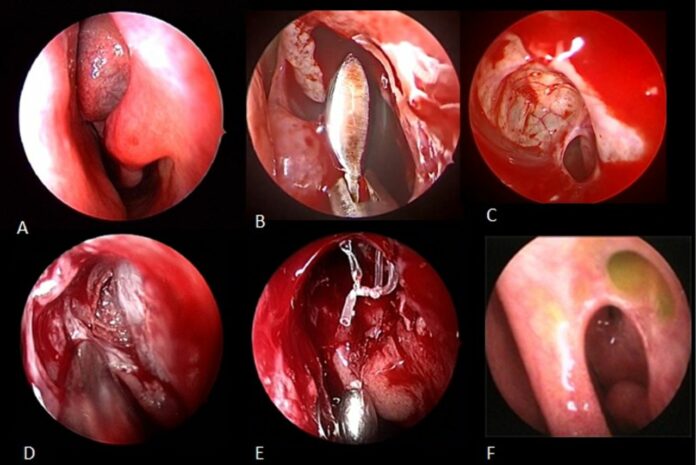
Rare presentation of agger nasi mucocele associated with nasolacrimal duct obstruction
Acquired nasolacrimal duct obstruction (NLDO) can be because of various causes, for example, tumours of the nasal cavity, trauma or surgery to the paransal sinuses, nasolacrimal ducts mucoceles and idiopathic stenosis of the nasolacrimal duct. However, there are not any cases of NLDO associated with agger nasi mucocele reported in literature. The first symptom of NLDO includes paranasal sinuses and tumours of the nasal cavity.
This article describes the case of a 28-year-old male patient with left-sided epiphoria and chronic dacryocystitis. The patient had no history of head trauma or any previous surgery of the nose or paranasal sinuses. Doctors advised a nasal endoscopy which showed bulging of the left lateral nasal wall in the area of the agger nasi. Although, there were no other abnormalities. Neither did the patient have any orbital symptoms, such as, nasal symptoms, limited orbital movement or visual disturbances. His history further revealed that he has been suffering from recurrent episodes of dacryocystitis for which he was initially treated with catheterisation. Although despite treatment the disease did not resolve.
Based on clinical examination, the patient was diagnosed with postsaccal NLDO.
Doctors performed an endonasal endoscopic dacryocystorhinostomy (DCR) under general anaesthesia. During DCR there was no sign of macroscopic erosion of the surrounding bone. An ophthalmologist also investigated the functionality of the nasolacrimal duct during the procedure. However, even after the mucocele was removed, there was longstanding obstruction which caused a plug formation and extensive fibrosis within the nasolacrimal duct. After the procedure was completed, left anterior ethmoidectomy and sphenoidectomy was also performed. The postoperative period was unremarkable. Doctors advised 5 days of oral antibiotics on the day of the surgery, discharging him the next day.
References
Agger nasi mucocele cause nasolacrimal duct obstruction and chronic dacryocystitis: clinical profile, management and outcome https://casereports.bmj.com/content/14/5/e242140



