Rhabdomyolysis followed by severe hypercalcaemia
According to recent data, rhabdomyolysis has been found to be a complication of COVID-19 infection. In a similar case, a 22-year-old Black British woman with a history of asthma presented to the local hospital with complaints of sore throat, myalgia and a 24-hour history of anuria. There were no other symptoms including fever, dyspnoea or cough. Neither did the patient have a history of tetany or gaining weight. Doctors diagnosed the patient with severe hypercalcaemia secondary to rhabdomyolysis.
She had no history of intense exercising and other than 3 doses of ibuprofen she hadn’t taken any other medications. Her medical history did not reveal anything significant and there were no signs of electrolyte disturbance. Her family history was clear of any autoimmune conditions. On questioning, she also denied using any illicit drugs and drank alcohol occasionally.
Laboratory investigations showed increased creatinine kinase levels and acute kidney injury.
The patient’s test results, as stated in the study were as follows: “Urine dipstick was positive for protein 3+ and blood 3+. She had a creatine kinase (CK) level of 764 470 IU/L (0–159) with a creatinine (Cr) 719 umol/L and acidosis, pH 7.23. She had severe hypocalcaemia with corrected value 1.28 mmol/L and a phosphate level measuring 4.49 mmol/L. A total of 30 mL of 10% calcium gluconate was administered for immediate correction”.
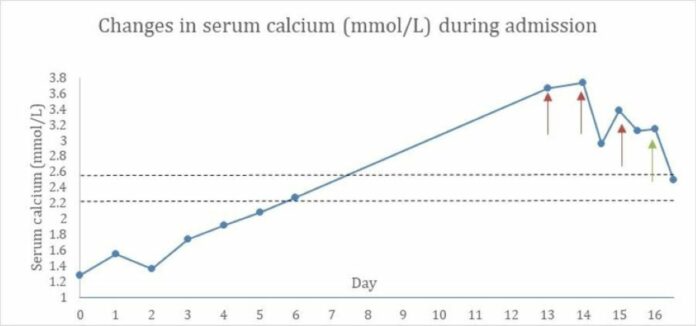
Doctors advised haemodialysis. The patient also suffered from a biphasic calcaemic response with initial severe hypocalcaemia which was followed by severe hypercalcaemia. The condition remained persistent despite haemodialysis. Calcium levels were controlled with continuous haemofiltration. Other causes of hypercalcaemia include malignancy, such as, squamous cell carcinoma. However, the patient’s history and examinations showed no signs of malignancy. There were also no findings of malignancy in detailed chest imaging. Her medications history ruled out the use of any medications that would implicate to hypercalcaemia.
Doctors diagnosed the patient with SARS—CoV 2 infection with associated rhabdomyolysis, given the raised levels of CK and renal impairment. For treatment doctors transferred her to a tertiary care unit for haemodialysis and renal replacement therapy. This, however, showed only temporary improvements in calcium. Therefore, doctors switched her to continuous haemofiltration with ultra-low calcium dialysate on the 17th day, requiring a total of 35 hours. There was no specific management for covid-19 and conservative measures were adequate because the infection occurred very early during the first wave.
References
Rhabdomyolysis and severe biphasic disturbance of calcium homeostasis secondary to COVID-19 infection https://casereports.bmj.com/content/14/5/e239611