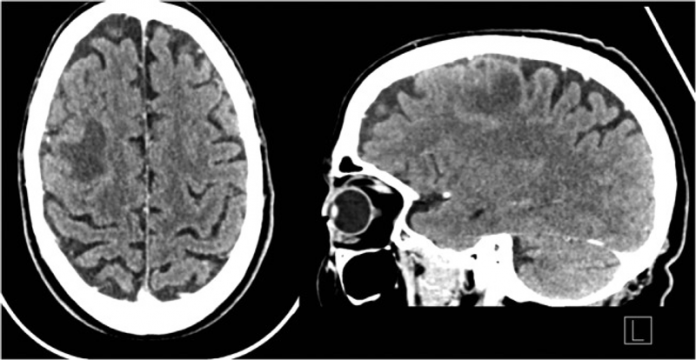
65-year-old patient with a history of prostate carcinoma reported to the hospital with generalised epileptic seizures. Imaging showed intracerebral abscess secondary to a tooth infection.
A 65-year-old male patient was admitted to the hospital after a generalised epileptic seizure. The patient’s wife also reported that he was increasingly confused in the preceding days. His medical history revealed that he had epilepsy of unknown origin during childhood, in addition to, hypercholesterolaemia, hypertension and type 2 diabetes.
The patient was prescribed with gliclazide, metformin, lixisenatide, rosuvastatin, medoxomil and olmesartan. He was also treated with valproate recently, which was tapered off 6 months earlier since the patient was seizure free for over 20 years. Similarly, there were no intracranial anomalies reported in previous imaging reports.
The clinical neurological examination of the patient was normal with Glasgow Coma Scale (GCS) of 15/15. Similarly, blood tests of the patient were also unremarkable with a slightly raised C-reactive protein (CRP) of 5.9 mg/L (reference <5.0 mg/L). EEG of the patient was also normal. For further evaluation, a CT scan of the skull was performed which showed a hypodense, contrast enhanced lesion in the right frontal lobe, surrounded by oedema. There was no evidence of midline shift or ventricular anomalies.
The patient was further advised an initial initial oncologic screening with imaging of the chest and abdomen because of his medical history. However, there were no signs of recurrence or primary malignancies. An MRI with diffusion weighted imaging (DWI) was performed after neurosurgical counsel. The findings of the MRI were consistent with the diagnosis of brain abscess with pachymeningitis. There were no signs of infection or cardiac vegetation on the transthroacic ultrasound.

Initial treatment consisted of systemic valproate, ceftriaxone, ornidazole, vancomycin and levetiracetam. Stereotactic drainage was done and spectrometry of the pus showed P. gingivalis as the causative bacteria. A further intraoral inspection showed several missing teeth with marked parodontitis. Previous CT imaging showed apical periodontitis the right upper first molar, left upper canine and right lower first premolar. However, the sinus cavities appeared normal.

The antibiotic regimen was altered to intravenous ceftriaxone and ornidazole.
19 days after the initial drainage, hemiparesis and hemineglect developed on the left side with an increase in epileptic seizures. In addition, the patient deteriorated further with a need for intravenous sedation and intubation. Imaging showed that the intracerebral abscess extended to the subdural space and formed a subdural empyema, spreading to the occipital and parietal regions.
Incision and drainage was done in addition to extracting the remaining teeth because of the clinical instability of the patient. Antibiotic treatment was continued for a total of 43 days until improvement was seen in clinical, radiological and biochemical examinations.
The patient was discharged from the neurosurgical ward after 59 days with no neurologic deficit. Similarly, he was referred to in-hopsital physiotherapy for regaining full motor function.
References
Van der Cruyssen, F., Grisar, K., Maes, H., & Politis, C. (2017). Case of a cerebral abscess caused by Porphyromonas gingivalis in a subject with periodontitis. Case Reports, 2017, bcr2016218845.



