Case Report
Shewanella putrefaciens is a rod-shaped, Gram-negative, nonfermenting, facultatively anaerobic bacterium with the ability to form biofilms. It is typically found in aquatic and marine settings, as well as food processing and storage facilities. S. putrefaciens, a member of the marine microflora, produces hydrogen sulfide (H₂S). That aids in the breakdown of organic matter like dead fish and algae.
These bacteria survive in a variety of environmental circumstances, including temperature, salinity, barometric pressure, and oxygen levels. They can also reduce a variety of metals and compounds, including nitrate, nitrite, thiosulfate, and trimethylamine-N-oxide.
Although uncommon, it can cause opportunistic infections in humans, including skin and soft tissue infections (SSTIs), such as cellulitis and wound-related infections, bacteremia, intra-abdominal infections, hepatobiliary disorders (due to the bacterium’s lipophilic nature), and otitis. It can also cause joint and bone problems like osteomyelitis and arthritis.
Antibiotic therapy, guided by antimicrobial susceptibility tests, is usually combined with local therapies, such as surgical debridement or drainage.
Case Presentation
A 74-year-old white Italian female came to our clinic in October 2024 with a recurring soft tissue illness. The patient had previously undergone a hysterectomy for benign pathology. But had no history of chronic diseases or immunosuppression, and was not taking any home medications.
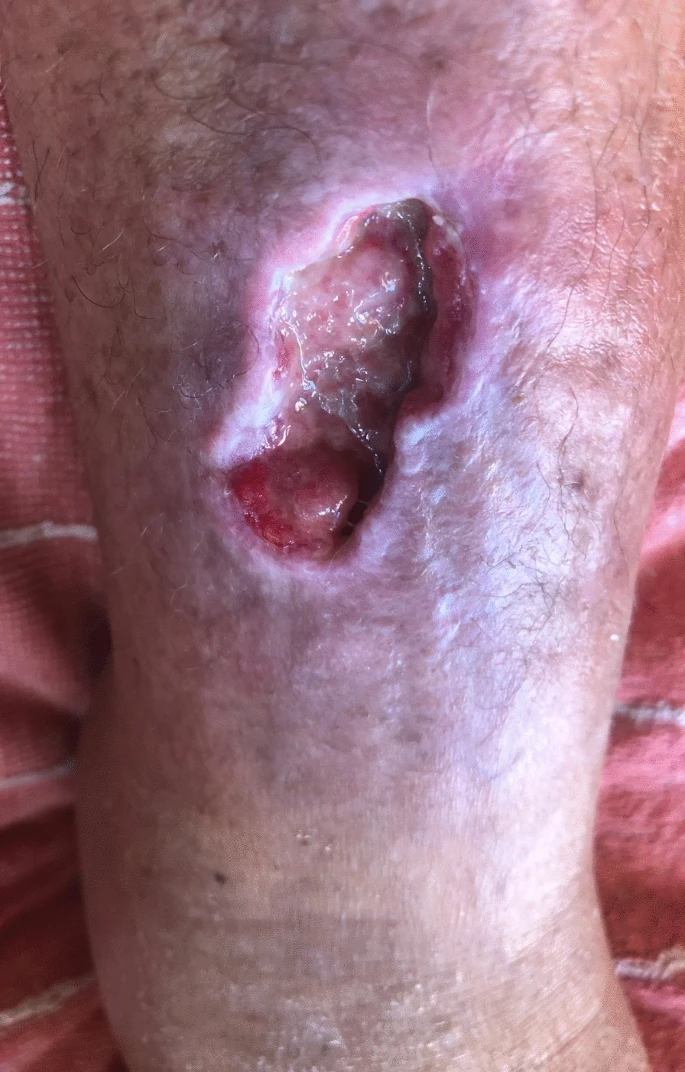
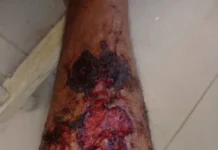
In early July, she damaged her right tibial crest by sliding and falling on a rock, resulting in an open cut; two weeks later, after bathing in shallow sea waters in Valencia, Spain, the lesion began to exhibit symptoms of infection.
A patient was treated with oral amoxicillin/clavulanic acid for 10 days, followed by a wound debridement procedure. The collected material tested positive for Shewanella putrefaciens and Bacteroides fragilis.
Despite medication, her symptoms continued after a month. Although there has never been a case of fever, an ultrasonography was conducted because of the lack of wound healing and the lingering evidence of local inflammation. The results showed a hypoechogenic region (8 x 11 × 24 mm) beneath the fascial plane that showed no indications of local infiltration. Significant stenosis or thrombosis was also ruled out by arterial and venous Doppler ultrasonography of the lower extremities.
Management
Examining the patient revealed severe edema of the right foot along with localized swelling and persistent erythema. A second course of antibiotic treatment was started with high-dose oral ciprofloxacin (750 mg every 12 hours) based on the antibiogram, along with a supplement for tendon protection, because the prior treatment was deemed sufficient for Bacteroides fragilis. After five days of receiving antibiotics for myalgia and sleeplessness, the patient stopped taking them on their own.
At treatment interruption, a follow-up ultrasound was performed: no significant fluid or fluid-debris collections were observed at the site of the reported lesion; there was a thickened and hypoechoic appearance of the immediately supra-fascial tissue, measuring ~ 2 mm in thickness, with a transverse extension of ~ 3–4 cm and a longitudinal extension of approximately 10 cm. At the site of the wound, this hypoechoic tissue reaches the skin surface through a short tract, with an extension of ~ 1–2 cm.
The tissue that was described was thought to be granulation tissue that had formed as a localized inflammatory lesion healed. The lesion healed normally throughout the course of the next month, showing no symptoms of local inflammation or erythema. Due to lymphatic insufficiency, the patient’s ankle continued to have hard edema.
Discussion and Conclusion
Chronic lower extremity ulcers and, more frequently, traumatic lesions exposed to seawater are risk factors for Shewanella spp. infections. Furthermore, because Shewanella can form biofilms, the bacterium mostly affects immunocompromised people, such as dialysis patients with severe renal failure, making hemodialysis or peritoneal catheters possible entry routes for infection.
The bacterium’s pathogenicity and clinical significance were confirmed in our instance by the full resolution that resulted from high-dose quinolone treatment. Antibiotic resistance may be influenced by wastewater that is released into the sea from treatment facilities and plants. This wastewater contains heavy metals and antibiotics. Antibiotic resistance and bacteria’s capacity to evade infections are closely related to climate change.