- HIV/AIDS predisposes patients to several opportunistic infections of the brain including tuberculosis and toxoplasmosis. On imaging, the lesions often present as ring-enhancing lesions.
- Treatment for toxoplasmosis helps resolve the lesions, as was the case with a 54-year-old patient.
Toxoplasmosis in AIDS is a leading cause of disease in the central nervous system. It is usually a complication of the late phase of disease. The lesions are typically found in the brain, presenting with symptoms of brain disease. In a similar case, a 54-year-old female patient presented to the emergency with generalised weakness with a 1-month history and altered sensorium for 2 days. The patient also was also responding poorly to verbal commands with repetitive speech. Other symptoms included headache and vomiting.
Neurological examination was unremarkable and did not show any signs of focal, sensory or cerebellar abnormalities. 12 years before his presentation, doctors had diagnosed him with AIDS because of HIV stereotype I. The patient was noncompliant to antiretroviral therapy and was found with a low CD4 count and viral load of 50 000 copies/mL. Doctors suspected the patient of having an opportunistic infection involving the central nervous system. The patient’s lumbar puncture showed normal cerebrospinal fluid (CSF) pressure, an elevated leucocyte count and protein, whereas, low glucose.
A thorough microbiological evaluation of the fluid ruled out the diagnosis of an infection involving the central nervous system.
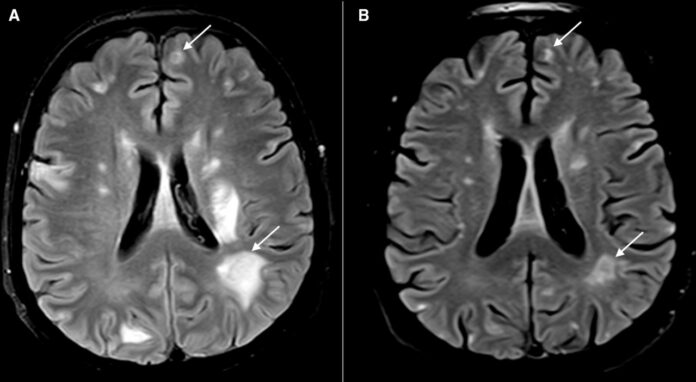
Brain MRI showed multiple ring-enhancing lesions (RELs) with signs of perilesional oedema, with the largest lesion in the left basal ganglia. Other areas of oedema included the cervicomedullary junction and both cerebral hemispheres. Doctors treated the patient with co-trimoxazole, steroids and antitubercular therapy. 2 weeks after treatment repeat MRI showed resolution oedema and RELs. Doctors started her on ART after 3 weeks.
The patient was doing well on 2 months follow-up.
References
Toxoplasmosis and tuberculosis: brain lesions in HIV/AIDS differentiated by response to therapy https://casereports.bmj.com/content/14/5/e243470



