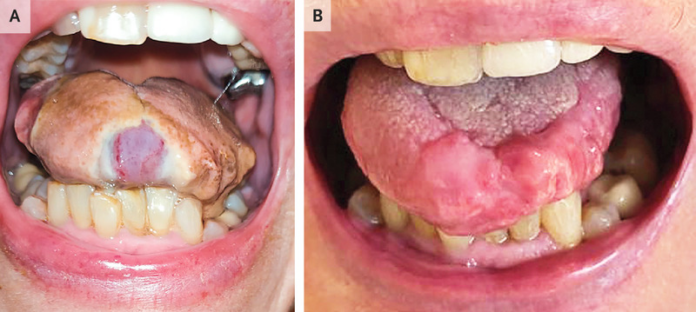
Case study: tongue necrosis
A 74-year-old female patient presented to the ER with a history of headache and swelling in her tongue for three days. It was associated with pain and blindness in the right eye that lasted for several hours. Doctors diagnosed the patient with tongue necrosis in giant cell arteritis.
Doctors did a physical examination which revealed discolouration and ulceration of the tongue. In addition, the right temporal artery had thickened. The labs showed an increase in the ESR (erythrocyte sedimentation rate), which was 42 mm per hour compared to the normal reference value of <42. Furthermore, the C-reactive protein level was 169mg per litre, based on the 0 to 5 reference range. The temporal artery biopsy specimens of the 74-year-old showed giant cells and inflammatory infiltrates throughout the vessel wall.
Diagnosis
These examination findings confirmed the diagnosis of giant cell arteritis. However, lingual infarction is a very rare complication of the disease. Literature suggests that despite its rarity it should be taken into consideration in patients presenting with tongue necrosis.
Treatment
She was admitted to the hospital and for treatment, the doctors prescribed her tocilizumab along with high dose glucocorticoids. After a few days of treatment, her vision returned and she was discharged. Doctors further advised her to continue using glucocorticoids and to taper the dose off slowly.
The patient was called back for a follow up two months after the initial presentation. Examination showed that the tongue necrosis had subsided with no further complications.
Giant cell arteritis is a systemic vasculitis of the arteries that affects the external carotid artery mainly. Similarly, it is prevalent in the elderly and presents with low-grade fever, claudication of the jaw, temporal tenderness, and loss of vision in some. The diagnosis is difficult in cases where it presents with atypical manifestations, which delays the treatment and leads to irreversible complications.
Lingual Necrosis is a severe complication of giant cell arteritis. To prevent complications, steps should be taken for immediate diagnosis, and it should be treated using prompt therapy.
Source: NEJM