A 31-year-old man presents with skin lesions and fever. Gets a diagnosis of HIV and Talaromycosis!
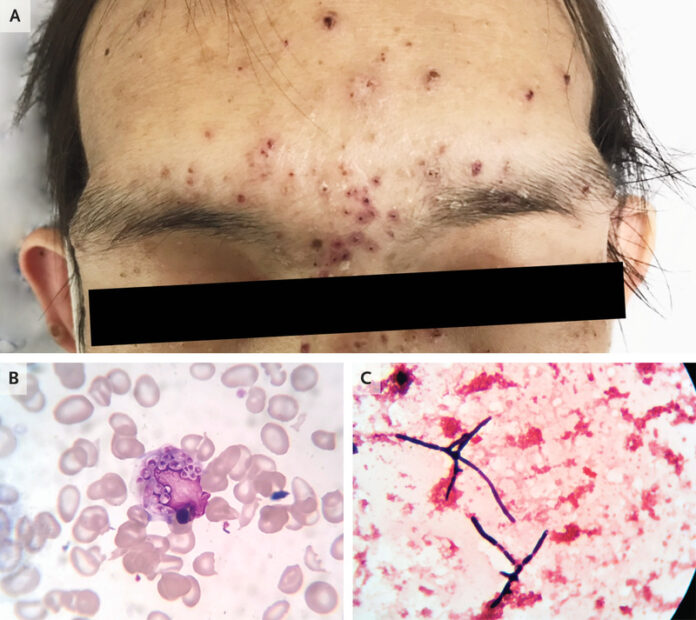
A 31-year-old man presented to the emergency department with complaints of fever and papular skin lesions for 1 month. Moreover, he reported a 10 kg weight loss in the past month. On examination, he was cachectic and febrile, with a body temperature of 38°C. Skin examination revealed umbilicated papules on his face, body, and extremities. Serological investigations showed a haemoglobin level of 8.3 g/dL, a white-cell count of 9200/mm3 with 88% neutrophils, and 4% lymphocytes. His platelet count was 80,000/mm3. Testing for human immunodeficiency virus (HIV) was positive. CD4 T-cell count was 10 cells/mm3. قانون البوكر
A peripheral blood smear revealed several intracellular and extracellular yeast-like organisms. These organisms measured 2 to 4 μm in diameter. Gram’s staining showed septate hyphae fungus. The investigations confirmed the diagnosis of Talaromycosis (formerly called Penicillosis), caused by Talaromyces marneffei (formerly Penicillium marneffei). bet 365
Talaromycosis is seen mostly in patients with HIV infection. تكساس بوكر However, non-HIV patients may acquire the infection when they have an immunocompromised state and/or in endemic areas.
T. marneffei, the culprit fungus, is a dimorphic fungus that can lead to rapidly progressive, life-threatening infection. Patients may have a fever, weight loss, fatigue, bone-marrow involvement ) anaemia, thrombocytopenia), respiratory symptoms, gastrointestinal symptoms, lymphadenopathy, altered mental state/confusion, agitation, etc.
The diagnosis in non-HIV patients is often delayed. Culture is the gold standard but slow, as it takes 2–4 weeks. Yeasts may be visible on microscopy of a peripheral blood smear or skin or lymph node biopsy.
The treating physicians diagnosed the patient and started him on amphotericin B. However, the patient, unfortunately, died 4 days after the initial presentation.
Reference:
Thamonwan Norasethasopon, M. a. (2021, April 01). Talaromycosis. Retrieved from The New England Journal of Medicine: https://www.nejm.org/doi/full/10.1056/NEJMicm2032478