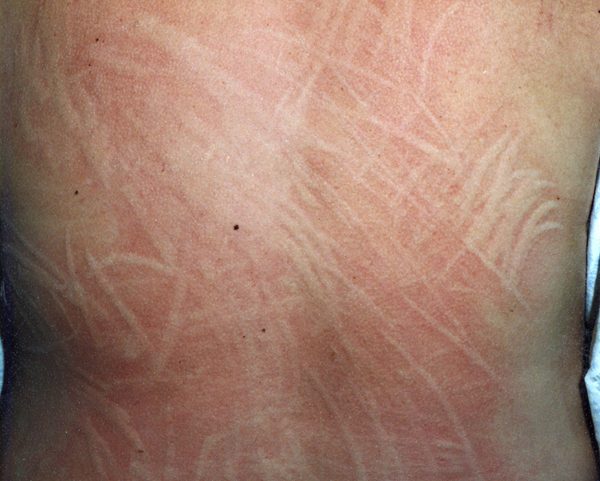
After getting up from a deep sleep, have you ever noticed creases on your skin? That’s due to prolonged pressure. But some individuals develop skin rash along these creases. That’s called dermographism.
This case describes a 32-year-old Scottish woman, known case of dermographism, was referred for another cycle of ultraviolet phototherapy three times a week for the recurrence of her condition. Eight months earlier, the patient had undergone similar ultraviolet therapy which completely resolved her dermographism. Pharmacological treatment with antihistamines showed minimal benefit.
On examination, her fingers exhibited erythematous rash, hyperkeratosis and dilated capillaries of the nail fold. proximal muscle weakness was observed.
Her lab results showed mildly increased alanine aminotransferase (ALT) and alkaline phosphatase. Muscle enzymes were also elevated. With this triad of muscle weakness, skin changes and lab results suggested a diagnosis of dermatomyositis. Results of histopathology and electromyography confirmed the diagnosis, therefore, oral systemic corticosteroids were started. Over the time effects of steroid blunted, thus, high-dose intravenous immunoglobulin (IVIG) therapy was initiated. Her symptoms showed a rapid recovery and ultimately complete resolution was possible.
The patient is
the discussion here had a combined disease. She was diagnosed with both
dermatomyositis and dermographism, the latter may or may not be directly
associated with the former. However, the severity of her dermographism can be
attributed to the generalised itching forcing the patient to scratch and rub
the skin, hence triggering dermographic urticaria.
What is dermatomyositis?
It is a rare, acquired inflammatory myopathy i.e. disease of the muscles, that also displays cutaneous findings. Rarely, the involvement of joints, heart, oesophagus, etc, is also seen.
What is dermographism?
The word ‘dermographism’ means writing on the skin. This condition that affects approximately 5% of the population, is an exaggerated tendency to get wheals and urticaria upon stroking or rubbing the skin. When the skin is stroke, suppose with a pen, the underlying local capillaries dilate causing delineated erythema, followed by arteriolar dilation and local oedema. This whole process imprints a graphic image on the skin along the lines where the skin was stroked.
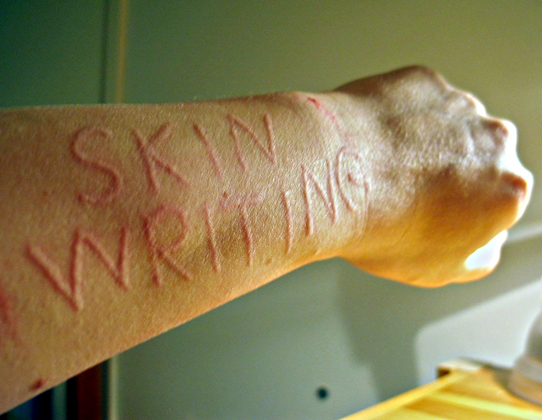
Although dermographism is an autoimmune condition, the exact cause remains unknown. Mast cells and eosinophils have been found to be at the centre of the process. Patients with simple dermographism, the most common type, usually remain asymptomatic. When symptomatic, wheals appear within 5 or 10 minutes of stroking and resolve spontaneously within 30 minutes. This can be triggered by the normally harmless stimuli, for example, clothing, hot bath, wiping with a towel, exercise, etc.
Diagnosis of dermographism is usually clinical. Laboratory tests may show increased levels of histamine and eosinophils. ESR may also be elevated.
Uncommonly, skin responses can be recorded using a dermographometer which applies (spring-loaded stylus) reproducible pressure in a graded fashion.
Rarely, the skin sample is taken for a biopsy which shows inflammatory infiltrates, dermal oedema and perivascular mononuclear cells.
Management is dependent upon the severity of the symptoms, spanning from avoidance of triggers, antihistamines, monoclonal antibodies and light therapy.
References:
Rahim, K. F., & Dawe, R. S. (2009). Dermatomyositis presenting with symptomatic dermographism and raised troponin T: a case report. Journal of medical case reports, 3, 7319. https://doi.org/10.4076/1752-1947-3-7319
Deacock S. J. (2008). An approach to the patient with urticaria. Clinical and experimental immunology, 153(2), 151–161. https://doi.org/10.1111/j.1365-2249.2008.03693.x
Grimm V, Mempel M, Ring J, Abeck D. Congenital symptomatic dermographism as the first symptom of mastocytosis. Br J Dermatol. 2000 Nov. 143(5):1109. [Medline].