Medical conditions found incidentally are the only kind of surprises no one wants.
Imagine finding out a disease or lesion or mass when it is least expected.
This happened with a 45-year-old woman who unexpectedly surprised by multiple hepatic lesions that were incidentally noted on imaging that was done for an unrelated reason. She neither had any relevant symptoms, nor the physical examination revealed any positive findings.
Serological tests were also normal with normal alanine aminotransferase, alkaline phosphatase, bilirubin, and a normal international normalized ratio, thus no hepatic dysfunction.
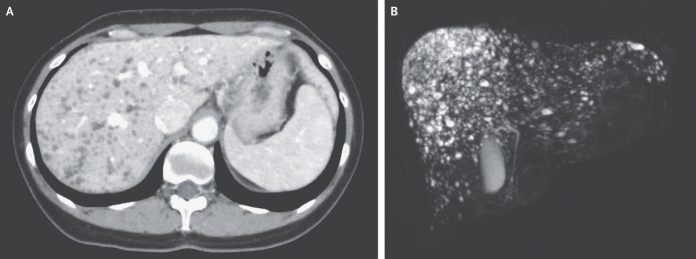
Further imaging studies were conducted to evaluate the lesions. Enhanced computed tomography of the abdomen revealed numerous, small, hypodense, non-enhancing nodules spread across the liver (Panel A). Magnetic resonance imaging with cholangiopancreatography revealed a “starry sky” appearance with multiple, small, T2-weighted, hyperintense cystic nodules throughout the liver, with no biliary duct communication (Panel B).
A diagnosis of biliary hamartomas was made.
No specific treatment is required; therefore, the patient was given none. At 2 year-follow-up, the imaging findings were unchanged.
Von Mayenburg complex (VMCs), also called biliary hamartomas are benign congenital malformations of the intrahepatic biliary ducts due to failure of embryonic involution. These are found incidentally on ultrasound and require further evaluation to be sure of the diagnosis as it can be confused with extra-hepatic metastatic disease, polycystic liver disease, abscesses, and diffuse hepatocellular carcinoma. In some cases, a histopathological evaluation may be necessary too.
Biliary hamartomas show no enhancement on the CT scan and are well-defined with distinct margins.
Biliary hamartomas may be single or multiple and are usually asymptomatic. Larger lesions may produce a compressive effect exhibiting as jaundice and portal hypertension. Usually, they measure less than 5mm in size, but the sizes may vary from 1mm to 15mm.
Biliary hamartomas can be classified according to the degree of hamartoma consistency/biliary dilatation, into the following three classes:
Class 1: Solid pattern with narrow bile channels
Class 2: Intermediate pattern
Class 3: Marked cystic dilatation of bile ducts within the lesions
If the diagnosis is confirmed and the patient is asymptomatic, no treatment is required. If need be, the lesions can be followed up to look for any changes in the sizes and severity.
References:
Zheng RQ, Zhang B, Kudo M, Onda H, Inoue T. Imaging findings of biliary hamartomas. World J Gastroenterol. 2005;11(40):6354‐6359. doi:10.3748/wjg.v11.i40.6354
Barboi OB, Moisii LG, Albu-Soda A, Ciortescu I, Drug V. Biliary Hamartoma. Clujul Med. 2013;86(4):383‐384.
Takafumi Taguchi, M. P. (2020, April 16).“Starry Sky” Appearance from Multiple Biliary Hamartomas. Retrieved from The New England Journal of Medicine:
https://www.nejm.org/doi/full/10.1056/NEJMicm1909482