The best technological advancement is aimed at serving the
need of the era. The primary step is to identify an emerging problem and then devise
a solution.
In the world of organ transplantation, an emerging problem
is a huge gap between the number of donors and the number of recipients. In other
words: the unavailability of donor organs.
This gap is further lengthened by the limitations of the effective
storage of the procured organs, the geographical distances, and the ischemic
injury due to prolonged periods in cold storage, subsequently affecting the
functionality.
This means that not only the unavailability of donor organs but
also the effective utilization of the available organs is a major concern.
Similarly, lungs, when procured from the donor have to pass
through multiple steps before the donor lungs can be safely transplanted. Some donor
lungs are deemed unfit for transplantation either due to advanced age, prolonged
preservation time, or reduced lung function. This problem was identified, and a
solution named Organ Care System came to light.
Gabriel Loor, M.D., surgical director of the lung transplant
program at Baylor St. Luke’s Medical Center, said:
“Bridging
the divide between a donor and a recipient has always been at the cornerstone
of transplantation.”
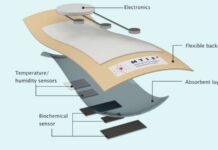
TransMedics® Organ Care System is one of its kind. Lung OCS,
a portable medical device, mimics the human body to temporarily provide a safe
haven where the procured lung is kept under optimal conditions, similar to the human
physiological environment, to maintain appropriate temperatures, respiration,
and perfusion, consequently improving post-transplant outcomes.
How Does OCS work?

After the lung is procured from the donor, it is typically
kept in cold storage. With the advent of OCS, the procured lung is now kept in
an OCS, which maintains normothermia, adequate perfusion, and breathing until
the lungs are removed from the system to be transplanted to the recipient.
Maintaining adequate nutritious perfusion and breathing has two-fold benefits: it minimizes the ischemic injury, which otherwise is part and parcel of being kept in cold storage, and it prolongs the preservation time. This subsequently increases the donor organ availability (expands the donor organ pool), minimizes the deleterious effects on the functionality, and improves post-transplant outcomes substantially.
Prolonged ischemic time has a magnificent impact on the incidence of primary graft failure. العاب ربح المال من الانترنت With OCS, the incidence of primary graft failure has been reduced, approximately, to 50%!

It doesn’t end here, Transmedics lung OCS not only preserves
the lung but also allows the healthcare professionals to continuously monitor
the functionality of the donor lungs, from the very first minute till the last
minute before transplantation.
Moreover, the donor lungs that have been initially deemed
unacceptable can now be used for transplantation!
How can a rejected organ be used for transplantation?
Rejection doesn’t always mean that the organ is
non-functional or diseased. Some rejections are benign, based on the limitations
of preservation techniques and resources.
As Loor said:
“It doesn’t necessarily mean that they are not
good organs to use, it just means that it would be nice if we had a little bit
more information on them before we committed our recipients to a transplant
with them.”
With OCS, there is a way around this limitation.
“I can place the organ on this device,
evaluate it for several hours, and have a glimpse of how it will function in
the recipient.”
Quite recently, the FDA has approved the expanded
use of OCS to include the previously unacceptable donor lungs.

“Many of us believe that now we have an ideal setting to manipulate the organ,” Loor said.
“Maybe administer gene therapy, stem cells, anti-inflammatory drugs. العاب بوكر للكبار Maybe we can change the blood type of the organ and offer more organs to more recipients. Maybe we can genetically modulate the organ, so it doesn’t reject. We really believe that we have a platform that we need to start looking at more creative ways to utilize for the advancement of quality organs and the quantity of organs. تعلم كيف تلعب الروليت ”