Dagmar Turner, a 53-year-old violinist with the Isle of Wight Symphony Orchestra, was diagnosed with a brain tumor in 2013 after she suffered a seizure during one of her concerts. Over the years cancer grew more aggressive despite multiple rounds of radiotherapy thus, requiring surgery.
The tumor was in Turner’s right frontal lobe and dangerously close to the part of her brain responsible for controlling intricate movements of the left hand, which are required to regulate a violin’s pitch and timbre.
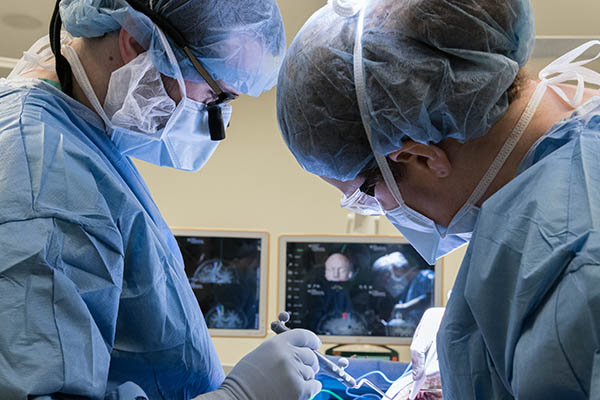
Dr. Keyoumars Ashkan, a consultant neurosurgeon at King’s College Hospital in London, came up with the idea to awaken Dagmar midway through the surgery so she can play the violin and be monitored, to make sure her coordination was not being affected. The team was successful in removing over 90% of the tumor without damaging her fine motor skills.
This particular procedure is called awake craniotomy or awake brain surgery and has been used multiple times in the past. Awake craniotomy is mainly used for brain mapping and removal of tumors in important brain areas mostly parts of the brain that controls vision, movement, and speech.
The violin is my passion… The thought of losing my ability to play was heart-breaking
Dagmar Turner
There are multiple benefits of awake craniotomy. Due to intraoperative brain mapping, the functional areas of the brain can be protected and there can be more extensive tumor resection. Studies indicate that there’s a reduced need for post-op intensive care monitoring, fewer neurological deficits, shorter hospital stay, and longer survival. Patients also generally have less pain and reduced postoperative nausea and vomiting.
However, no innovative procedure comes without added risks. Some of the risks associated with awake craniotomy include vision changes, loss of memory, meningitis, stroke, seizures, speech or learning difficulty and impaired balance.
Patients are usually kept sedated using general anesthesia for the craniotomy and closure but awakened for mapping and tumor resection. Numbing medication is applied to the scalp to ensure comfort. The anesthesiologist’s aim in awake craniotomy is to transition the patient smoothly from sedation to the awake state without any confusion or drowsiness. For the awake phase, all anesthetic agents are stopped, although sometimes small doses of fentanyl may be kept running for analgesia. Pain is usually managed via local anesthetics along with intravenous acetaminophen.
Researchers now aim to look at the long-term outcomes (tumor recurrence, survival, quality of life) of using different forms of anesthesia and analgesics for awake brain surgery.
References:
Zhang K, Gelb AW. (2018). Awake craniotomy: indications, benefits, and techniques. Colombian Journal of Anesthesiology, 46-51.
https://www.kch.nhs.uk/news/public/news/view/31290