A 13-year-old boy presented to the ophthalmology clinic with complaints of progressively increasing black spot in the center of his vision involving both eyes. There were no other associated complaints, nor any of the family members had a similar complaint. At presentation, the visual acuity was 20/40 and 20/50 in his right and left eye, respectively.
Fundus examination was performed on both eyes, which showed diffuse, yellow, pisciform (fish-shaped) flecks.
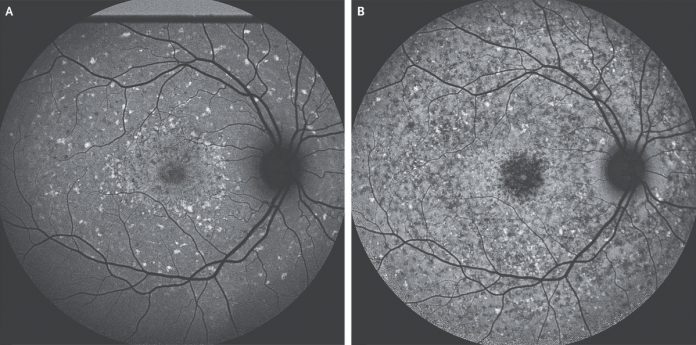
Non-invasive retinal imaging, called the short-wavelength autofluorescence, was performed to evaluate further. It showed diffuse, increased fluorescence, also described as hyperautofluorescent lesions, suggestive of bisretinoid accumulation, and patchy central areas of atrophy of the retinal pigment epithelium with peripapillary sparing (Panel A).
A diagnosis of Stargardt juvenile macular degeneration was made, and ABCA4 sequencing further confirmed the diagnosis.
The patient was advised to avoid vitamin A supplementation, which may accelerate bisretinoid accumulation.
After 6 years, the degeneration had progressed, with worsening central scotomata. He complained of an even enlarged central blind spot. Visual acuity of the right eye worsened to 20/70 from 20/40, but that of the left eye remained the same, i.e., 20/50.
Autofluorescence imaging showed peripapillary sparing and progressive atrophy in the previously identified areas of pisciform flecks. (Panel B).
Stargardt’s disease, also called fundus flavimaculatus, is an autosomal recessive disorder, is the most common inherited macular degeneration. It is caused by mutations in the gene encoding ATP-binding cassette subfamily A member 4 (ABCA4), which consequently leads to photoreceptor cells’ degeneration in a part of the central retina, also called the macula. The loss of photoreceptor cells is manifested as a slowly progressive loss of central vision, which begins during childhood or adolescence.
Usually, the peripheral vision remains unaffected. Some patients have seen to have their peripheral vision affected in their older ages.
Both the types of photoreceptors, rods and cones, are affected in Stargardt’s disease, but for unknown reasons, cones are affected more than the rods.
Vitamin A is known to improve vision, why can’t these patients take vitamin A?
The metabolites or byproducts of vitamin A are known to have harmful effects in patients with Stargardt’s disease. One theory is that the responsible gene (ABCA4) for washing away these harmful byproducts in normal eyes is mutated in individuals with Stargardt’s disease, thereby making vitamin A rather harmful.
How can Stargardt’s disease be treated?
There isn’t a treatment for this inherited disease; however, patients are advised to wear sunglasses when stepping into the sunlight and avoid smoking, both active and passive.
There are trials and studies underway to find a cure/treatment for macular degeneration. Let’s keep our fingers crossed for gene therapy or successful stem cell therapies that can repair and regenerate the damaged retina and photoreceptor cells.
References
Jin K. Oh, B. a. (2020, June 11). Stargardt Juvenile Macular Degeneration. Retrieved from The New England Journal of Medicine:https://www.nejm.org/doi/full/10.1056/NEJMicm1913388
Stargardt Disease. (2019, July 10). Retrieved from National Eye Institute: https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/stargardt-disease