Case Presentation
A 45-year-old lady was admitted to the emergency department of a secondary medical facility due to recurring attacks of epigastric discomfort. It was accompanied by fever, nausea, vomiting, and hypotension. Her medical history was notable for having type II diabetes, hypercholesterolemia, asthma, gastric reflux disease, and obesity. Moreover, the patient denied any prior trauma or endoscopic retrograde cholangiography. However, she stated that the only previous surgical procedure she had was an endometrial ablation. The results of her physical examination were normal. Her family doctor approved an abdominal scan and normal blood testing.
Investigations
In the emergency room, the patient was revived, and a parenteral broad-spectrum antibiotic was administered for a possible intra-abdominal infection. Except for an elevated white blood count of 25000×10*9 per litre and abnormal liver function tests with aspartate aminotransferase of 456 U/l. With an alanine aminotransferase of 654 U/l and an alkaline phosphatase of 345 U/l, the haematological panel showed normal values. In addition to chest and abdomen radiograms, which were not contributing, blood and urine cultures were also taken.
An immediate abdominal ultrasound indicated a normal gallbladder and intrahepatic and extrahepatic bile ducts. Except for a 4-cm-diameter lesion in the left hepatic lobe, indicating an abscess. The abscess was elongated, with a linear echogenic structure in the center, measuring 4.1 cm in length and a few centimeters in width. The patient developed respiratory distress a few hours after arriving at the emergency department, and she was admitted to the intensive care unit, where she was treated for multiorgan failure (MOF) due to sepsis, and her blood cultures were positive for polymicrobial infection (Klebsiella, Escherichia coli, Streptococcus, and Enterococcus).
The patient was treated for several weeks with parenteral antibiotics (ampicillin, cefuroxime, and metronidazole) before being discharged. In addition to a follow-up appointment at a tertiary medical center for a surgical opinion on a possible intrahepatic-infected foreign body.
The patient’s CT abdomen revealed the presence of an elongated structure across the left lateral hepatic segments. However, with an almost complete clearance of the abscess chamber.
Treatment
The patient was scheduled for an elective exploratory laparoscopy and possibly foreign body removal. She had inflammation and adhesions between the omentum and the gallbladder at the time of the operation. A cholecystectomy was performed laparoscopically. There were no clear symptoms of GIT perforation.
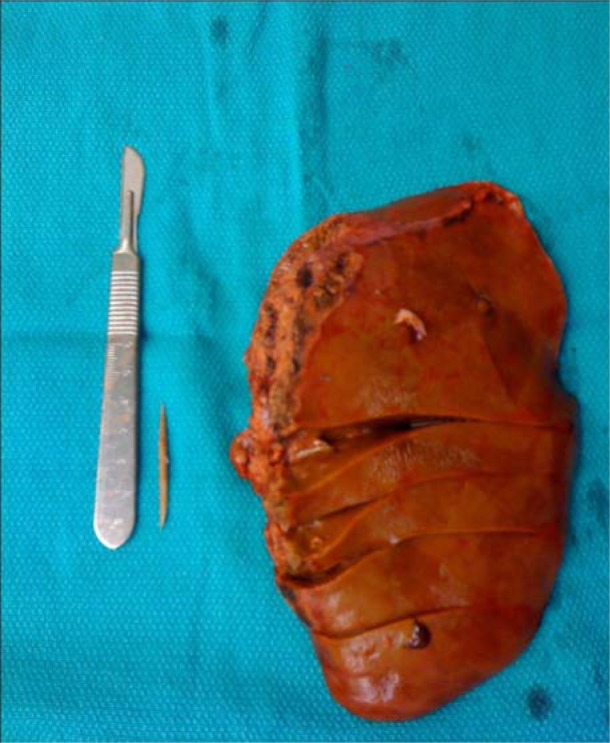
A laparoscopic hand-assisted left lateral segmental resection was performed. The presence of a hard object akin to a toothpick about 4.5 cm in length was discovered during an examination of the surgical material. The final pathological diagnosis revealed that the foreign body was made of wood. Moreover, it supported the assumption that the patient had a hepatic abscess caused by an ingested toothpick that had migrated from the GIT into the liver parenchyma.
Follow-up
The treatment was well tolerated by the patient, and her postoperative course was uncomplicated. The patient is still feeling well six months after her surgery and denies that any of her pre-operative problems have returned.
Discussion
In less than 1% of instances, ingested foreign substances induce GIT perforation. The stomach and duodenum are the most common perforation sites. There have only been 46 reported cases of foreign substances penetrating the GIT wall and migrating into the liver, causing abscess cavities to develop. In most cases, the ingested object lodged in the left hemiliver after migrating from the intestinal lumen.
The majority of patients have non-specific symptoms, making diagnosis difficult, especially when the foreign body is not evident on abdominal radiographs. When there is clinical suspicion for this unusual diagnosis, ultrasonography (US) and CT are the preferred methods. At the same time, MRI is usually contraindicated when metallic items cannot be entirely ruled out. These items are typically hyperechoic on ultrasonography and have high-density features on CT.
A survey of the literature identified only 17 occurrences of hepatic abscesses induced by the migration of an ingested toothpick. To our knowledge, this is the first case of a patient who underwent intraoperative ultrasonography and laparoscopic hepatic resection for a hepatic tumor that caused sepsis and MOF.