What is one of the biggest limitations in
the treatment of patients with end-stage heart failure?
The
answer in one phrase is ‘unavailability of the organ.’
The problem doesn’t solve with the availability of organs because there is another speed breaker here, i.e., utilization of the donor organs.
The distance between the donor hospital and the recipient hospital is a limiting factor too.
With the rise in the number of patients requiring heart transplantation, there is a dire need for maximizing the utilization of the available donor heart. Typically, after harvesting the heart, it is transferred to the cold storage where it is exposed to prolonged ischemia, which substantially increases the risk of primary graft failure in the recipient. During the period of prolonged cold ischemia, the donor heart has an increased risk of metabolic acidosis, which consequently increases the risk of graft failure. A maximum of four to six hours of the ischemic period is acceptable before the heart is deemed unsafe for transplantation.
On average, 22 people die each day while waiting for a transplant!
So, how to maximize the utilization of donor heart?
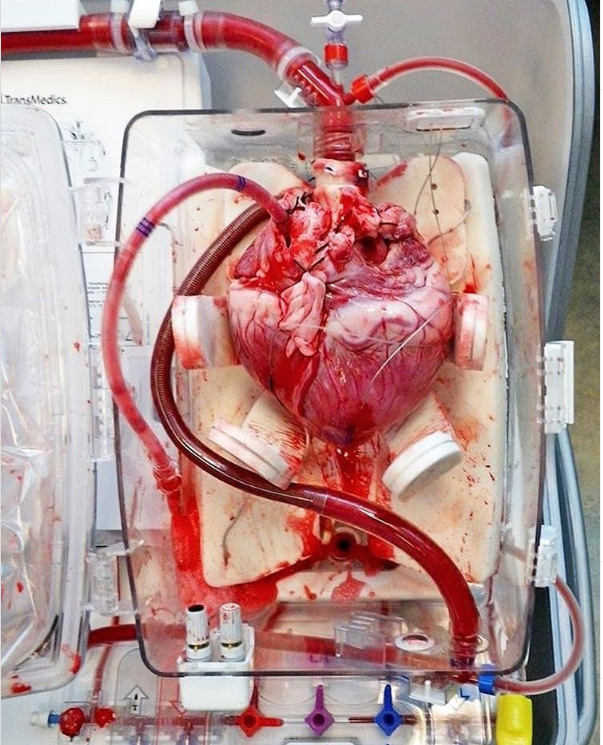
By using a perfusion machine that can maintain a normal temperature and perfuse the beating heart with nutrition-rich, oxygenated blood while it is outside the body!
This perfusion machine, the organ care system (OCS), prolongs the period to a minimum of eight hours.

Organ Care System is the only way to keep the heart perfused ex-vivo. The oxygenated blood is pumped into the aorta and the coronary arteries. From the coronary sinus, the blood enters the right ventricle after passing through the tricuspid valve. From the right ventricle, the blood is ejected into the pulmonary artery cannula, ultimately returning to the blood reservoir. The blood flows in a pulsatile fashion with the help of a diaphragmatic pump generating pulsations. This whole system helps to keep the heart perfused with warm oxygenated blood to shorten the period of cold ischemia, ultimately decreasing the risk of graft failure.

Image Source: ScienceDirect©
The perfusate includes insulin, antibiotics, steroid, sodium bicarbonate, multivitamins, and fresh donor blood.
It is imperative to keep a close watch on the hemodynamic and chemical parameters during the transfer from the donor to the recipient hospital. The standard parameters are maintained by adjusting the maintenance solution, pump flow, gas flow, and pacing rate.
Upon reaching the recipient hospital, 1 L of a cold cardioplegic agent is used to arrest the donor heart, which can then be disconnected from the OCS and implanted into the recipient.
All in all, OCS has unveiled a new ray of hope. With OCS, the ischemic time is prolonged, thus allowing long-distance travel between the donor and the recipient hospitals, thus decreasing the chances of graft failure. Moreover, OCS gives adequate time to the surgeons who are operating on patients with previous cardiac surgery or patients who are undergoing transplantation again to perform adhesiolysis and prepare the cuffs before arresting the heart in the OCS; consequently improving the prognosis.
OCS has carved a new path to a future with an expanded donor pool and best utilization of the existing donor organs.
References:
Masaki Tsukashita, MD, P. Y. (2015, December 12). Organ Care System for Heart Procurement and Strategies to Reduce Primary Graft Failure After Heart Transplant. Retrieved from ScienceDirect: https://www.sciencedirect.com/science/article/pii/S1522294215001701
Sunjaya, A. F. (2019, April 01). Combating Donor Organ Shortage: Organ Care System Prolonging Organ Storage Time and Improving the Outcome of Heart Transplantations. Retrieved from Hindawi: https://www.hindawi.com/journals/cdtp/2019/9482797/
Popov, A. F., García Sáez, D., Sabashnikov, A., Patil, N. P., Zeriouh, M., Mohite, P. N., Zych, B., Schmack, B., Ruhparwar, A., Kallenbach, K., Dohmen, P. M., Karck, M., Simon, A. R., & Weymann, A. (2015). Utilization of the organ care system – a game-changer in combating donor organ shortage. Medical science monitor basic research, 21, 29–32. https://doi.org/10.12659/MSMBR.894020