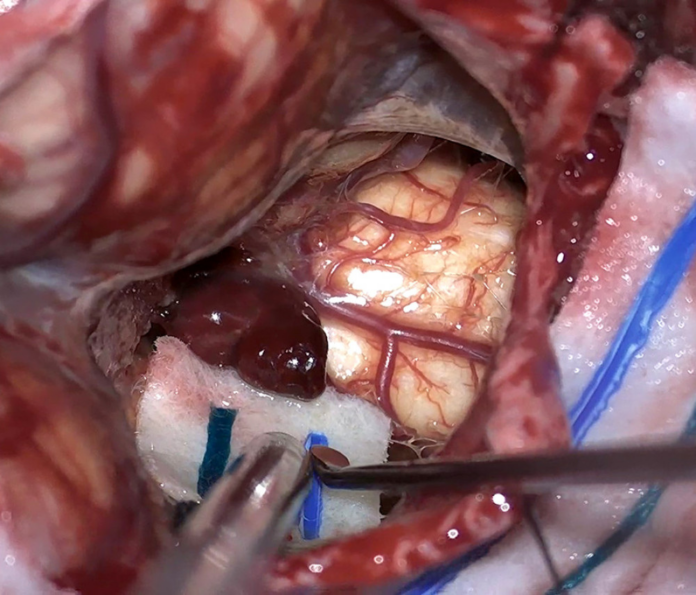
Case study: cavernous hemangioma
This article describes the case of a 42-year-old man who presented to a rural hospital with the complaint of a headache that increased in intensity with age. According to the patient, the pain affected his frontal region. Doctors diagnosed the patient with haemorrhaging of a cavernous hemangioma of the brainstem.
The patient initially presented to the hospital with a fever and a headache. For examination, doctors advised tests to check inflammatory markers. Findings of which were within normal range and started the patient on treatment with empirical antibiotics. After being hospitalised for 2 days, the patient was transferred to the Internal Medicine Department for further investigations. In addition, his symptoms continued during his stay at the hospital. The fever did not subside and he complained of a continuous waning headache. However, with no signs of nausea, vomiting or meningeal irritation. Similarly, because the patient’s symptoms did not subside, doctors decided to broaden the antibiotics and added antiviral agents.
Investigations and diagnosis
Doctors advised several lumbar punctures, all of which showed a bloody appearance of the CSF with red blood cells. Further findings included an increase in white blood cells which is consistent with a traumatic tap. He was also referred for a CT scan which showed a small round hypodense mass that was attached to the fourth ventricle floor. In addition, he was subsequently referred for an MRI which confirmed the presence of a lesion, characterised as a thrombus. Although, the patient’s symptoms continued and he was referred for a serial CT scan which showed an increase in the size of the lesion. He was transferred to the neurosurgical ward for further evaluation.
According to the study, he was in a good neurological state. Cerebral digital angiography was performed which showed no abnormal findings. A repeat CT showed a further increase in the size of the lesion with a protruding clot into the fourth ventricle. Based on these findings, doctors suspected bleeding of the underlying cavernous hemangioma in the floor of the brainstem. The patient’s symptoms were attributed to a ruptured cavernous hemangioma. Given that the patient was at a high risk of bleeding, a suboccipital craniotomy was suggested for the removal of the ruptured cavernoma.
Prognosis and follow-up
After the procedure, the patient developed left facial nerve palsy, xerostomia and left abducens palsy. However, 2 days after the procedure, the abducens palsy and xerostomia resolved. He was afebrile post-operatively and was discharged with left-sided facial palsy, 6 months into the procedure the patient was called for a follow-up and there was no recurrence of the headaches or signs of neurologic deficit.
Source: American Journal of Case Reports



