Many of the times, flu and sore throat are home-treated. Herbal and home remedies form elders of the family or previously taken medicines by family members apparently resolve the disease. But that doesn’t always happen. Sometimes there is more to it!
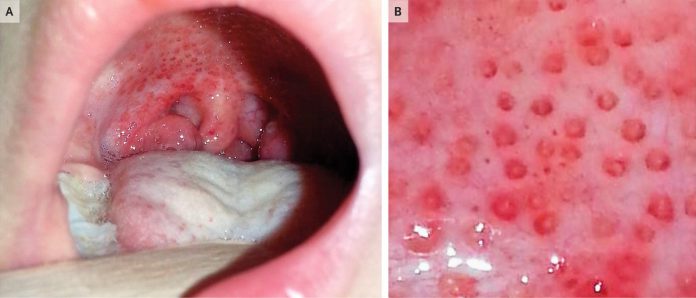
A 9-year-old girl presented to the clinic with complaints of fever and sore throat. There were no other associated symptoms, and the patient had been healthy previously. On examination, she had a temperature of 38.5°C, an inflamed uvula, enlarged tonsils, swollen and tender cervical lymph nodes, and erythematous papules with pale centers, i.e., “doughnut” lesions were seen on both the hard and soft palates (Panels A and B).
A rapid streptococcal antigen for group A streptococcus was positive. A throat culture was performed to confirm the diagnosis.
Group A beta-hemolytic streptococcus grew on the culture.
These doughnut lesions are a characteristic clinical sign group A streptococcus pharyngitis.
Oral amoxicillin was started and continued for 10 days. The patient recovered without any complication.
The pharynx has been a victim of many viruses and bacteria. Mostly, viruses are the culprits, but bacteria are not uncommon either.
A gram-positive coccus, streptococcus pyogenes, which is also known as group A streptococcus, causes acute pharyngitis, transmitted via respiratory secretions. It is clinically presented as an abrupt onset of fever, pain on swallowing (odynophagia), and throat irritation/pain. Headache and gastrointestinal symptoms may also accompany. Usually, a history of exposure to an infected person is present within the previous 2 weeks of presentation.
Cough, runny nose (rhinitis), hoarseness, and redness of the eyes (conjunctivitis) are characteristics of viral sore throat and are usually absent in GABHS.
Physical examination clues that are suggestive of GABHS infection include palatal petechiae, cervical node lymphadenopathy, uvular edema, inflamed erythematous uvula, tonsillar exudates, and pharyngeal inflammation.
The history and physical examination are insufficient in diagnosing GABHS infection, definitely as the clinical presentation overlaps with many other pathogens. Therefore, investigations are mandatory.
The best initial, first-line investigation is the rapid antigen detection test (RADT). This test is highly specific; therefore, it doesn’t necessarily need to be followed by a throat culture. However, when the test is negative in children, but there is strong clinical suspicion, throat cultures should be performed
The primary management goal is to reduce the severity and duration of the disease—this aids in preventing complications and spread to other individuals.
Oral penicillin or amoxicillin for a total of 10 days with or without NSAIDs/acetaminophen are recommended for the treatment of GABHS. If oral treatment is not possible, intramuscular benzathine penicillin G can be given.
What if the patient is allergic to penicillin?
If the patient has a rash with penicillin, second-generation cephalosporins can be given. If the patient has anaphylaxis, then clindamycin, clarithromycin, or azithromycin can be prescribed.
How soon are the effects of treatment seen?
Resolution of symptoms usually occurs within 1 to 3 days, and affected individuals can return to school or work after 24 hours of treatment.
Should the test be repeated after treatment?
A test of cure is not recommended. In special circumstances, like acute rheumatic fever or other complications, the test may be repeated.
References
Akira Kobayashi, M. a. (2019, March 07). “Doughnut” Lesions. Retrieved from The New England Journal of Medicine: https://www.nejm.org/doi/full/10.1056/NEJMicm1810556
BETH A. CHOBY, M.U.–C. (2009, March 01). Diagnosis and Treatment of Streptococcal Pharyngitis. Retrieved from American Family Physician: https://www.aafp.org/afp/2009/0301/p383.html
Ashurst JV, Edgerley-Gibb L. Streptococcal Pharyngitis. [Updated 2020 May 16]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK525997/