A rapidly progressive infection led to the death of a boy who traveled to the US from Europe
A 5-year-old boy presented to the emergency department of a hospital in the US with complaints of high-grade fever, vomiting, progressive lethargy, and rash for the past 18 hours. The boy had traveled from Europe to the US one week back.
Physical examination :
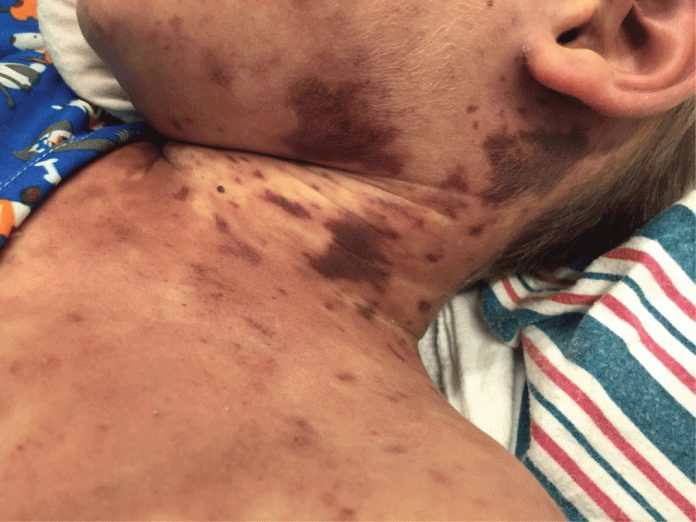
On examination, the patient was obtunded, hypotensive, febrile, with increased heart rate and increased respiratory rate. On skin examination, non-blanchable purpuric rashes were seen on the face and extremities bilaterally.
A working diagnosis of Meningococcemia was made.
A blood sample was withdrawn for culture, and the patient was managed with fluid resuscitation, broad-spectrum antibiotics
The child was started on vasopressor therapy with norepinephrine and he was transferred to the pediatric intensive care unit (PICU).
In the PICU, the vasopressor therapy was stepped up, and the patient was given crystalloids and blood products. Despite aggressive therapy, the patient’s condition worsened, and the purpuric rash became generalized (Figure 1) over the next 2 hours.
Endotracheal intubation was performed, and the patient was kept on a mechanical ventilator.
His serological results showed:
- Leukopenia
- Thrombocytopenia
- Deranged coagulation profile.
The patient’s condition worsened, and he went into cardiac arrest. Despite aggressive treatment, unfortunately, the child passed away within 4 hours of admission.
His postmortem cerebrospinal fluid (CSF) gram stain showed intracellular gram-negative diplococci in neutrophils (Figure 2 with arrows). Neisseria meningitides grew in his blood and CSF cultures.
Meningococcemia is a rare but life-threatening infection caused by Meningococcus or Neisseria. Affected patients may present suddenly with a high-grade fever, headache, sore throat, cough, nausea, vomiting, a petechial or purpuric rash which rapidly progresses to purpura fulminans along with hemodynamic instability. The purpura fulminans is a poor prognostic factor.
Fulminant Meningococcemia or Waterhouse-Friderichsen Syndrome is the most severe form of this infection. Without prompt management, the infection may progress to death.
Aggressive fluid resuscitation, inotropic support, and prompt administration of intravenous antibiotics such as third-generation cephalosporin are essential management steps for a successful outcome.
References:
Chegondi M, Torres A (2018) Purpura Fulminans and Refractory Shock in a Child. Clin Med Img Lib 4:112. doi.org/10.23937/2474-3682/1510112