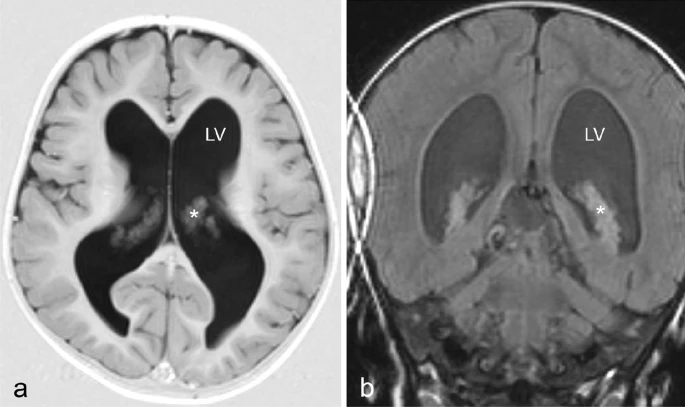
Case of congenital hydrocephalus
Congenital hydrocephalus caused by excessive liquor production as a result of choroid plexus hyperplasia is a rare condition that may necessitate unconventional treatment approaches. It is seen in trisomy 9p, where coexisting congenital heart disease complicates the therapeutic approach, as illustrated in the current case report.
Congenital hydrocephalus due to choroid plexus hyperplasia has been well documented in children with trisomy 9p, along with a variety of phenotypical manifestations such as craniofacial dysmorphic features, growth retardation, mental retardation, hand and foot anomalies, and congenital heart diseases such as ventricular septal defect (VSD), atrial septal defect (ASD), hypoplastic left heart, and cardiomyopathy.
A ventriculoperitoneal (VP) shunt is commonly used to treat hydrocephalus. However, in patients with choroid plexus hyperplasia, CSF production can exceed several litres per day, resulting in CSF accumulation in the abdominal cavity and ascites. To control choroid plexus hyperplasia-derived hydrocephalus in trisomy 9p, treatment options such as ventriculoatrial (VA) shunt, choroid plexus coagulation, and pharmacological treatment may be required. However, as illustrated by the current case report, the known risk of VA shunt-associated cardiovascular complications such as endocarditis, heart failure, intraatrial thrombus, and pulmonary hypertension may preclude this treatment modality in trisomy 9p patients with cooccurring congenital heart disease.
Case presentation: congenital hydrocephalus
This article describes the case of a Caucasian girl with trisomy 9p and a family history of the syndrome in an older brother and twin sister. Twin A was born with a birth weight 1800 g, length 45 cm and displayed dysmorphic characteristics such as a large fontanel, low-hanging ears, and a bulbous nose from birth. Clinodactyly was also observed, such as short fifth fingers with only one flexion joint and palms with a single crease. At birth, the head circumference was smaller than average, similar to twin B.
Doctors discovered an acceleration in head circumference growth to two SD above average at 20 months when compared to her twin sister (average for the age). It was also noted that the girl could not yet walk independently, but there were no signs of neurological problems, pain, or growth retardation. A brain MRI revealed enlarged lateral ventricles with a prominent choroid plexus. Aqueduct stenosis was initially suspected, but ventriculoscopy and ventriculography later disproved this. As a result, the patient was treated with a VP shunt at the age of two. She displayed signs of massive CSF accumulation into the abdominal cavity and fluid leakage through the abdominal cicatrices on the second postoperative day.
A shunt revision revealed no leakage and confirmed the shunt system’s functionality
The clinicians concluded that CSF formation far exceeded the patient’s abdominal absorptive capacity. During the same admission, the VP shunt was replaced with a VA shunt.
Due to a slight psychomotor compromise, the girl was now attending special classes at the age of six, but she had language and independent ambulatory function. However, hydrocephalus was suspected due to irregular episodes of headache and vomiting, resulting in an X-ray image showing displacement of the atrial part of the drain due to growth. The drain was successfully extended surgically, alleviating the pressure symptoms.
Irregular episodes of headache and vomiting reappeared when the patient was 14 years old. Shunt dysfunction was suspected, and a large occipital cyst in contact with the right lateral ventricle was discovered on MRI. The symptoms were successfully relieved by surgical fenestration.
Transthoracic echocardiography (TTE) revealed dilation of the left ventricle and a reduced ejection fraction (EF, 49%) in the patient when he was 16 years old
Her twin sister had been diagnosed with cardiomyopathy several years prior, prompting the TTE. Following that, ramipril pharmacological treatment was initiated. After a few months, the patient was admitted to the neurosurgical ward with signs of shunt dysfunction (that is, headache, vomiting, and tiredness). The neurological examination revealed no specific compromise, but a subsequent ophthalmological examination (fundus photography) revealed papilledema, lending credence to the clinical suspicion of raised intracranial pressure (ICP). A brain MRI revealed a colloid cyst in the third ventricle, possibly occluding the foramen of Monro.
Doctors treated the patient with acetazolamide 100 mg/kg/day and furosemide 1 mg/kg/day. After one and two months, there were no signs of hydrocephalus or ascites. There were no complications or neurological deficits discovered. At a 10-month follow-up, she was more active and less tired in school and at home.
Source: Journal of Medical Case Reports



