1 in every 2000-5000 live births has a congenital diaphragmatic hernia, where the mediastinum shifts to the opposite side. In addition, an abnormality is seen in the arterioles, and the lungs become hypoplastic, which results in pulmonary hypertension. There is also a severe impairment in the respiratory and cardiac functions at birth. It results in significant mortality and morbidity, which has an association with malformations.
What is Congenital Diaphragmatic Hernia?
Congenital diaphragmatic hernia is a posterolateral muscle defect of the diaphragm. In most cases, the location is on the left side, and it allows the abdominal viscera to pass to the thoracic cavity.
Approximately 70% of the cases are of by Bochdalek hernia, occurring in the left posterolateral part of the muscle. 27% of cases are of Morgagni hernia, which occurs in the anteromedial retrosternal portion of the diaphragm. Moreover, the septum transversum accounts for 2-3% of the cases.
Although the cause of congenital diaphragmatic hernia is unclear, 2% of cases are familial, which have chromosomal abnormality association; detected in 15% of patients.
Case Presentation
This case is of a nine-year-old boy who came to the emergency department of the children’s hospital with a complaint of pain. The pain was constant in the left lower quadrant and started three days ago. In addition to an episode of non-bilious and non-bloody vomiting. He was born after a c-section without any complications and has a history of underlying diseases.
He has a history of two hospital admissions. Once for pneumonia at the age of eleven and once for fever and left side cervical lymphadenopathy. He was five years old at that time. However, doctors discharged him in a good condition both times. In his previous admissions, there was no sign of diaphragmatic herniation on his chest x-ray.
Examination
When the doctors examined him, they noticed a marked decrease in his lung sound on the left side. However, the right lung showed no abnormality while auscultation. Moreover, his heart sound was typical and louder on the right side. Abdominal examination revealed no abnormality. It was not tender, with no palpable masses. The rest of his systemic examinations were also normal.
The doctors requested CXR and other initial lab tests. They saw a round-shaped lesion with clear boundaries and air-fluid levels on the CXR. In addition to a shift in the mediastinum towards the right side. Furthermore, hydatid cyst and lung abscesses were the initial differentials of the doctors based on the CXR.
Since the boy had mild hypotension and tachypnea, the pediatric ICU admitted him immediately. His doctors gave him oxygen through a nasal canula, and he was nil per os with continuous monitoring using a pulse oximeter and a cardiac monitoring device.
Treatment
The treatment included IV hydration, ceftriaxone, clindamycin, and vancomycin administration. His blood tests were within normal ranges. However, a request for surgical consultation was underway.
Radiological Findings
The doctors also did chest sonography that showed a dilated stomach with nutrients in the left hemithorax. It indicated that half of the patient’s stomach was in the thorax. The abdominopelvic ultrasound revealed mild free abdominal and pelvic fluid. However, the rest of the findings were not remarkable.
A Spiral CT scan of the lungs with IV contrast reported that the heart and the mediastinum shifted to the right side. It was due to the pressure effect of the dilated stomach and colon. It was noted, that the loop of the colon had occupied major parts of the left hemithorax. There was dilation on the distal third of the oesophagus, which was significant for oesophagal hernia and gastric volvulus.
Emergency Intervention
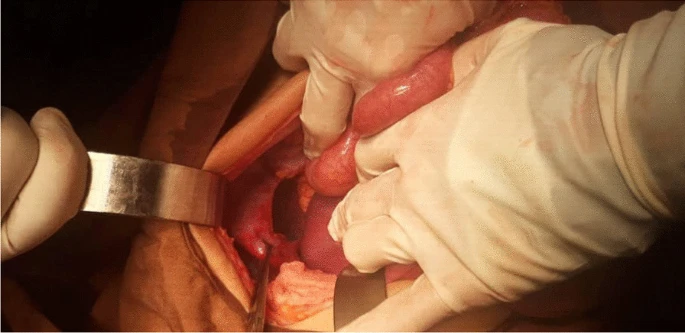
During diagnostic evaluations, the patient was suffering from recurrent vomiting. Consequently, the nasogastric tube insertion didn’t pass to the stomach during decompression of the stomach. It coiled in the oesophagus. Doctors did an emergency laparotomy due to the hypotension and tachypnea using a subcostal incision on the left side. There was also a wide defect on the left posterior part of the diaphragm, about 3 cm. The stomach, colon, and spleen were inside the thorax. It was accurately repaired using nonabsorbable sutures.
The Shape of the Defect: Congenital Diaphragmatic Hernia
The location of the defect was the muscular segment of the diaphragm along with the edge and the shape of the defect was in resemblance to a congenital diaphragmatic hernia. However, no other abnormalities could be detected, for example, malrotation.
Treatment Outcome
The patient was stable post-surgery. The doctors continued his antibiotic and hydration treatment. To prevent stress ulcers, he was taking pantoprazole. His nasogastric tube was removed after two days of the surgery and he started a liquid diet. For the rehabilitation of his pulmonary function, doctors started chest physiotherapy and incentive spirometry.
He was discharged uneventfully, and no complications were seen upon his three-month follow-up.
Conclusion
It is essential to suspect herniation of abdominal contents through the diaphragmatic hiatus in patients with right side mediastinal shift and tachypnea. Early diagnosis and surgical treatment can prevent the condition from becoming life-threatening.