Cogan syndrome is defined as a rare autoimmune disorder that is commonly linked with ocular, vestibular and auditory involvement. The involvement is assumed to be from small vessel vasculitis. In the case of Cogan syndrome, many patients often progress from symptomatic syndromes to systemic syndromes. The syndrome may further present with gastrointestinal, neurologic and musculoskeletal manifestations. In some cases, large vessel involvement has been described, for example, aortitis. However, limb ischemia has rarely been reported.
Similarly, treating the syndrome with severe systemic manifestations is based on organ involvement and degree of extension. This case is a classic example of systemic manifestations, systemic vasculitis and subsequent ischemia in a rare autoimmune disorder. In such cases, emergent interventions, for example, specialist involvement, anticoagulation and imaging are required to prevent any unfavourable outcomes.
Case study: Cogan syndrome
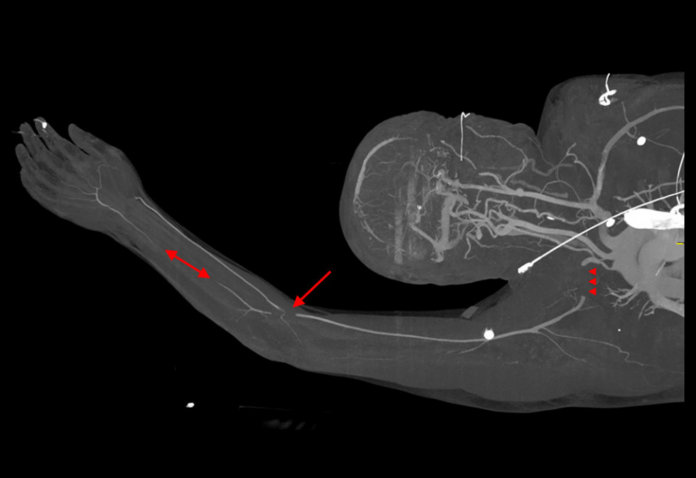
This article describes a rare case of Cogan syndrome in a 50-year-old patient. The syndrome was complicated by acute vascular ischemia of the left upper extremity. The patient presented with complaints of severe acute pain and weakness in the left arm. He was diagnosed with Cogan syndrome 4 years prior to the current presentation, the symptoms included left-sided hearing loss and bilateral uveitis. Physical examination was significant for the pallor of the left arm and wrist pulselessness. Doctors referred the patient for computed tomography. The findings of which were suggestive of vasculitis and concerns of embolic occlusion in several arterial structures of the left upper limb.
After consulting various specialists, the patient was treated with high-dose steroids, anticoagulants and topical nitroglycerin. The patient showed significant improvement post-treatment. On presentation to the emergency department, the patient had concerns of numbness, tingling and severe pain in the left upper extremity that last for 24 hours. Other findings included a dusky discolouration of the left hand and crescendo pain. The findings warranted a visit to the emergency department.
The pain was in the forearm and hand. The dusky discolouration and pain in the left hand are what prompted the patient to visit the emergency department. The patient did not have complaints of fever, peripheral oedema, shortness of breath, chest pain, headache, rash or chills. The patient’s medical history, however, was significant for CS. It was diagnosed 4 years prior in an outside facility.
Investigation findings
Investigation findings showed sensori-neural hearing loss which was followed by bilateral anterior uveitis. Whereas elevated inflammatory markers, C-reactive protein 228 mg/L). As per the outside records, the patient was treated with rituximab and several months later with azathioprine as a steroid-sparing agent. However, a year later, there was a flare of disease with fatigue, tinnitus, uveitis, photophobia and right-sided hearing loss.
The patient was started on oral prednisone 60 mg, daily, whereas the azatioprine was halted. In addition, he had continuous progressive hearing loss and was evaluated for his illness 2 years ago at a quaternary care facility. The diagnosis of CS was confirmed. The patient’s condition then progressed to inflammatory arthritis of major joints and bilateral hearing loss. The patient had no previous history of vasculitis. However, he did have 1 episode of pyoderma gangrenosum that required him to be put on immunosuppressants. Similarly, he currently had no new symptoms ofhearing loss, arthritis or hearing loss. His medications included adalimumab 40 mg which was given every two weeks. 2000 mg PO of mycophenolate daily, atrovstatin 20 mg PO daily and 10 mg PO prednisone, daily with maintenance dosing.
Diagnosis and follow-up
Doctors advised further blood work which showed a mild elevation of inflammatory markers. A CT angiography of the left upper extremity showed multiple areas of embolic occlusion. The findings are consistent with the diagnosis of vasculitis. After consulting the vascular surgery department, the patient was referred to the rheumatology department. He was treated with IV high-intensity heparin drip, 2% topical nitroglycerin to the left upper extremity, vascular mittens and pain control. The patient showed significant improvement after 5 days of treatment. He was discharged on oral warfarin therapy and oral high-dose prednisone steroid taper. Doctors further continued him on his previous medications adalimumab and mycophenolate. He showed no symptoms at 2-month follow-up.
Source: American Journal of Case Reports



