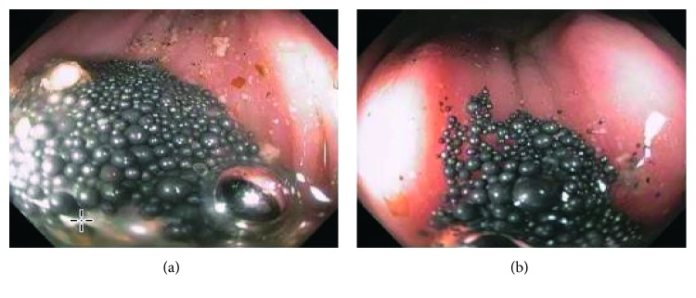
Symptoms of weakness, fatigue, outburst of temper, irritability and imbalance caused by acute mercury toxicity in 54-year-old.
This article describes a case of acute mercury toxicity in a 54-year-old male patient with a past medical history of degenerative joint disease, polysubstance dependance and major depressive disorder. The patient presented to the emergency with a 5-day history of weakness, fatigue, outburst of temper, irritability and imbalance. The symptoms presented after he ingested 5 ounces of mercury in an attempt to kill himself. On questioning, he denied experiencing any tremors or changes in vision and hearing. There were no signs of nausea, vomiting, diarrhoea, abdominal pain or shortness of breath. The symptoms were a result acute mercury toxicity.
Physical examination showed no signs of obvious distress. The patient appeared oriented to time, person and place, alert and developed. The patient’s blood pressure was 144/96, Heart rate 74, respiratory rate 16 and temperature 96.3. Neurological examination showed that the patient’s cranial nerves were intact with normal motor function and no sensory deficits. In addition, abdominal examination was significant for distended and nontender abdomen with normoactive bowel sounds. The rest of the physical examination was unremarkable.
Doctors advised laboratory tests on admission. The tests showed normal haemoglobin, platelet count and WBC. However, results showed a slight elevation in creatinine level with low potassium. Urine drug screen was positive for cannabinoid, benzodiazepine and amphetamine. Similarly, toxicology workup showed elevated levels of mercury. Abdominal x-ray visualised a diffuse radiopaque material throughout the colon.
Doctors transferred the patient to the intensive care unit because of the toxic mercury levels and neurological signs and symptoms.
The patient’s vital signs, neurological checks and electrolytes were measured regularly. On admission, the patient was also referred to the poison control team. The team recommended for the patient to be started on chelating agent, succimer. To enhance GI motility, the patient was also started on intravenous fluids and continuous replacement of electrolytes. The neurology team further evaluated the patient and advised a head CT. However, the CT findings showed no intracranial abnormalities.
The psychiatry team evaluated the patient as nonsuicidal at the time and started him on escitalopram and discontinued bedside sitter. The patient showed improvement during his stay, however, remained hemodynamically stable. Follow-up X-rays showed a continued decrease in the amount of mercury in the descending colon and hyperdense material in the cecum and ascending colon.
References
A Challenging Case of Acute Mercury Toxicity https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5835301/