A team of researchers have successfully used a single bacteriophage to treat an antibiotic-resistant infection in an immunocompromised patient.
The World Health Organization (WHO) has labelled antibiotic resistance as one of the top 10 global public health threats. The misuse and overuse of antibiotics, poor infection control strategies, and natural mutation of microorganisms are all to blame for the emergence of drug-resistant strains. Malaria, tuberculosis (TB), typhoid, HIV, and influenza have all developed resistance to the commonly used drugs. These resistant strains make it harder to treat infections and increase the disease burden. Therefore, scientists are busy working on developing more effective drugs. Now, for the first time, researchers have successfully treated an antibiotic-resistant infection using a single bacteriophage.
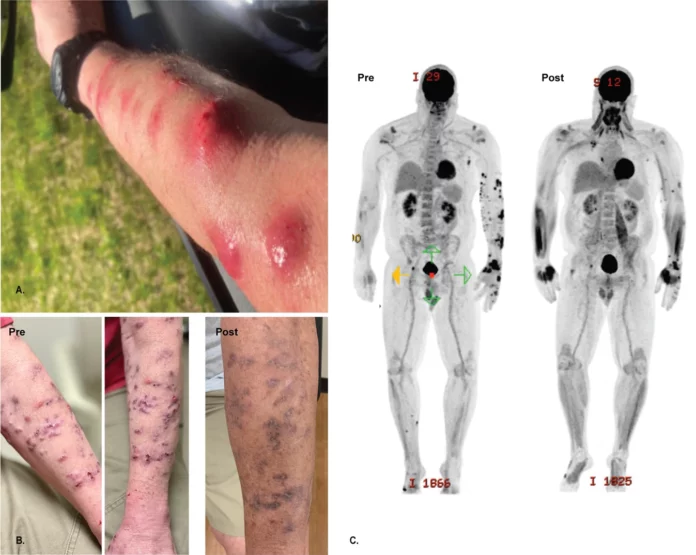
In January of 2020, the 56-year-old man developed large nodular lesions on his left upper arm along with muscle pain, weight loss, night sweats, and fatigue. He did not report any trauma or injury to the region of the lesions. He also suffered from stage II chronic kidney disease and had undergone a mitral valve repair in 2014. Furthermore, in 2019, he was diagnosed with arthritis for which he received multiple immunologic drugs along with steroids. At the clinic, doctors performed a skin biopsy to confirm the organism.
According to the study published in the journal Nature Communications, the rheumatoid arthritis patient had developed a Mycobacterium chelonae infection. This particular bacterium is widespread in the environment and causes opportunistic infections in humans. It causes skin and bone infections, more commonly after surgery or trauma. تنزيل العاب اندرويد Moreover, septic arthritis, bloodstream infections, and osteomyelitis can also occur from Mycobacterium chelonae infections. Similar to other Mycobacterium species, it has over time developed a multidrug-resistant strain.
Despite multiple antibiotic regimens, the patient’s skin lesions continued to persist and spread to other parts of the body. He also developed resistance or toxicity to several medications. Therefore, doctors considered him a good candidate for bacteriophage therapy.
Muddy, the Phage
Bacteriophages, or phages, are types of viruses that can infect bacteria and ultimately kill it. These organisms are present abundantly in the environment Since their discovery in the 1930s, scientists have used phages for treating bacterial infections. Moreover, bacteriophages are also used in the food industry to prevent spoilage from bacteria.
Researchers at the University of Pittsburgh have spent decades collecting phages as part of their SEA-PHAGES project. According to team member Professor Graham Hatfull, they’ve gathered more than 20,000 samples in their lab. As part of the study, the team tested multiple phages against a sample of the patient’s infected skin until they stumbled upon Muddy. Next, they cultured a sample of the phage and sent it to the hospital in Boston.
We’ve got a large collection of phages, and we’ve sequenced over 4,000 of their genomes, so we understand their genomic profiles and relationships in exquisite detail.
Professor Graham Hatfull, University of Pittsburgh
Prior to administration of the phage, doctors removed as much of the infected skin as possible and prescribed the patient antibiotics. Just a few weeks after the treatment, the patient’s skin lesions began to clear up and after two months, he tested negative for M. chelonae.
The patient developed neutralizing antibodies against the bacteriophage but continues to have stable improvement of disease with negative biopsies and no evidence of bacterial resistance to the phage.
study authors
The patient received the treatment over a course of eight months and his biopsies continued to test negative for the antibiotic-resistant bacteria. According to the study authors, this is the first study that has demonstrated the successful use of a bacteriophage in treating an immunocompromised individual with antibiotic-resistant infection. لعب قمار حقيقي Previous studies have mostly relied on a cocktail of various phages.
Bomb Survivor with Antibiotic-Resistant Infection
Earlier this year, a team of doctors in Belgium treated a 30-year-old bomb survivor’s superbug-infected wound using bacteriophages. According to the study, the woman had received extensive damage to her left leg as a result of an explosion at the Brussels Airport in 2016. Due to complications, she had to undergo several procedures to stabilize her condition. However, four days after the procedure, she developed an infection in her surgical wound that tested positive for Klebsiella pneumoniae.
Despite extensive antibiotic therapy, her condition worsened, and she developed widespread necrosis. Moreover, the skin graft used for her wound also became infected. Therefore, after exhausting all other options, doctors turned to bacteriophage therapy.
A team at the Eliava Institute in Tbilisi out the patient’s bacteria strain and isolated bacteriophages in a petri dish. After a few rounds, they were able to identify the most effective phages for the superbug. كازينو أون نت The 30-year-old received a solution containing the bacteriophages directly to her infected wound. Just three months after the treatment, her wound stopped discharging pus and her left thigh muscle regained function. And after 3 years, she was back to walking again. Furthermore, neither the wound nor the bones tested positive for K. pneumoniae.
These cases prove that bacteriophage therapy could be an important tool in the fight against drug-resistant bacterial infections. A clinical trial of phage therapy could soon become a reality as scientists explore the treatment further.
Reference:
Jessica S. Little et al, Bacteriophage treatment of disseminated cutaneous Mycobacterium chelonae infection, Nature Communications (2022). DOI: 10.1038/s41467-022-29689-4



