An 82-year-old man developed an amebic brain infection (granulomatous amebic encephalitis) and presented to the emergency with a 2-week history of generalised weakness. The diagnosis was confirmed through an autopsy that was performed after the patient’s death. لعبة مباشر
An 82-year-old male patient with history of B-cell lymphoma presented to the emergency department with generalised weakness that had started 2 weeks ago. كيف تلعب القمار The patient’s cancer had been in remission for more than 10 years. Patient’s presenting symptoms were indicative of an amebic brain infection.
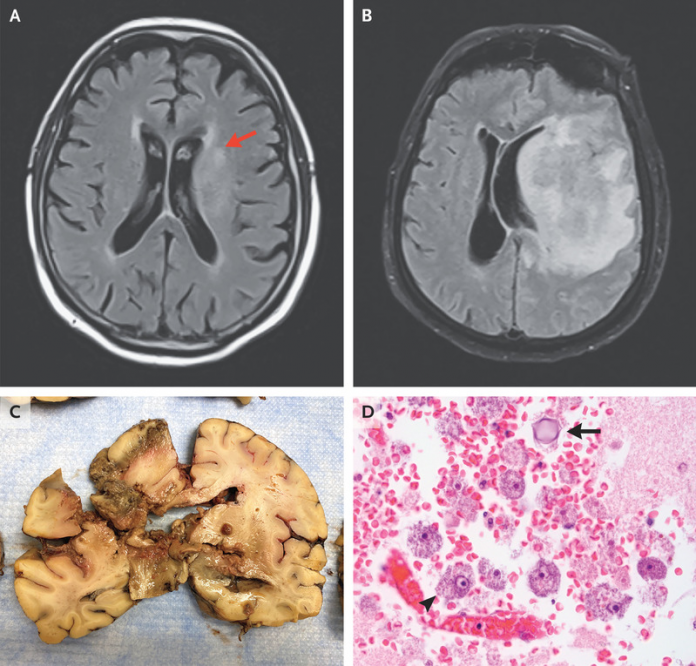
Physical examination showed diffuse weakness without any focal findings. One day after the patient was admitted, he delivered aphasia and weakness on the right side and exhibited an altered mental status. The patient was advised an MRI (Magnetic resonance imaging) which was evident of a nonenhancing signal abnormality in the left paramedian frontal lobe (Panel A, arrow).
A lumbar puncture was performed to remove a sample of the cerebrospinal fluid (CSF). Analysis of the CSF showed a protein level of 159 mg per deciliter (reference range, 15 to 45) and 455 nucleated cells, with 22% neutrophils and 46% lymphocytes. The cultures were negative with no malignant cells in the cytological analysis. Similarly, despite having received treatment for bacterial, viral and fungal meningitis, the patient became more drowsy and started having seizures.
The MRI was repeated after two days which showed a large lesion in the frontal, parietal and temporal lobe, associated with mass effect (Panel B). لعبة بينجو However, unfortunately, the patient died 9 days after presenting to the emergency clinic.
After the patient’s death, an autopsy was performed which was evident of liquefactive necrosis (Panel C). In addition to this, trophozoites and cysts were visible through microscopic evaluation (Panel D). Similarly, polymerase chain reaction identified acanthamoeba species, confirming the diagnosis of granulomatous amebic encephalitis.
Granulomatous encephalitis or amebic brain infection is a rare infection of the nervous system caused by free-living amebas and has a high mortality rate. The infection is particularly caused by acanthamoeba species and is transmitted via contact with soil or fresh water. The patient’s wife later revealed that the only soil he was exposed to was from potted-plant maintenance.
References
Schimmel, M., & Mehta, I. (2020). Granulomatous Amebic Encephalitis. New England Journal of Medicine, 383(13), 1262-1262.