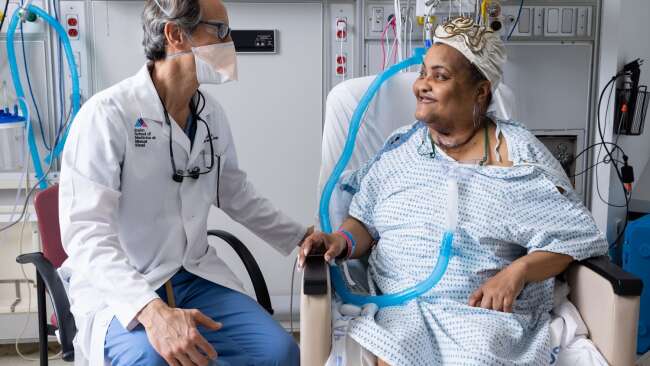
A 56-year-old woman in New York has become a recipient of the world’s first tracheal transplant.
In January, surgeons at Mount Sinai Hospital in New York spent 18 gruelling hours completing a feat never done before. The team of over 50 experts including nurses, anesthesiologists, surgeons, and residents successfully performed the world’s first complete tracheal transplant. Until now doctors had been unable to transplant the trachea because of its complex blood supply; its tiny vessels are almost impossible to surgically reconnect. Thus, leaving patients affected by long-segment tracheal damage with no treatment option. موقع الخيل However, the ground-breaking surgery provides a promising solution to patients with tracheal damage.
For the first time, we are able to offer a viable treatment option to patients with life-compromising long-segment tracheal defects, and this development will change the standard of care.
Dr Eric M. Genden, lead surgeon
Sonia Sein, a social worker from the Bronx, had suffered a severe asthma attack several years ago. As a result, the 56-year-old underwent repeated intubation and developed tracheal damage. The surgical attempts to reconstruct her trachea caused further damage. كيف تربح في القمار Therefore, doctors had to surgically create a hole in her neck and put a tracheostomy tube to help her breathe. The tracheostomy tube not only put her at a higher risk of infections but also suffocation and death.
Therefore, she decided to research tracheal transplants. That is when she stumbled upon Mount Sinai’s Tracheal Transplant Program. For several years she kept calling doctors asking for an appointment but to no avail. كيف تربح في البوكر As doctors had not decided to conduct the risky procedure in humans just yet. However, late last year, Dr. Eric Genden at Mount Sinai called her back telling her he was ready to give it a try.
30 Years of Research Later
Tracheal transplants are one of the biggest challenges in medicine. Dr Genden and his colleagues went over multiple articles to figure out a way to restore the transplanted organ’s blood supply. Inspired by research from the 1800s, the team decided to link the large vessels in the patient’s oesophagus and thyroid gland with the small vessels of the donor’s trachea. Thus, resulting in successful revascularization of the donor trachea.
Moreover, Sonia did not suffer from any complications from the procedure, or any signs of organ rejection. Doctors continue to monitor her progress and reaction to antirejection therapy.
As a result of the procedure, Sonia’s tracheostomy tube was removed, and she was able to breathe through her mouth for the first time in 6 years.
The procedure will hopefully doors for those suffering from tracheal damage as a result of birth defects, diseases, burns, or tumors. Moreover, Dr. Genden and his team believe the procedure can be particularly useful in hospitalized COVID-19 patients who may have suffered tracheal damage from intubation.
It is particularly timely given the growing number of patients with extensive tracheal issues due to COVID-19 intubation. Because of both mechanical ventilation and the nature of the COVID-19-induced airway disease, tracheal airway disease is precipitously increasing, and now we have a treatment
Dr Eric M. Genden, lead surgeon



