An 8-day-old neonate gets a near-fatal infection after a water birth.
Water birth is when labor, delivery, or any part of either occurs when the mother is immersed in a tub of warm water. Water birth helps reduce pain and relaxes the mother during delivery thereby relieving stress which could alter the uterine activity. The buoyancy and hydrostatic pressure by the water improve uterine perfusion and also helps maintain the upright position of the mother.
But there is another side of the picture too. Water birth exposes the infant to water and water-borne pathogens.
A case of a Canadian infant is an example of a water-related infection in a newborn.
Parents of an 8-day-old baby girl brought her to the hospital with complaints of fever, irritability, and poor feeding for the past 1 day. There were no complaints of drowsiness, vomiting, seizures, or rash. The baby was born at full term vaginally during a water birth. The prenatal course was unremarkable.
Labour:
The mother had a rupture of membranes approximately 3 hours before the vaginal delivery but had no fever. She delivered the neonate under the care of a midwife in a hot tub of water at home. The mother had opted for a water birth. She had filled the tub with hot water 3 days before the delivery day.
Postnatally after water birth:
The baby girl weighed 3.49 kg. she had no post-natal complications until a day before the presentation. The baby breastfed well and was active at- and after birth.
During the current presentation, the examination of the baby revealed a body temperature of 39.1°C, a heart rate of 172 beats/min, respiratory rate of 60 breaths/min and oxygen saturation of 97% on room air.
Physical examination revealed no remarkable findings except mildly increased work of breathing.
A plain radiograph of the chest showed right upper lobe pneumonia.
Management:
The treating physicians ordered blood samples for serological workup of sepsis after which they started the baby on ampicillin and cefotaxime. The baby’s condition deteriorated so her physicians shifted her to the neonatal intensive care unit for intubation.
The baby suffered a multiorgan failure, acute respiratory distress syndrome, hematologic abnormalities, and hemodynamic instability. The intensivists started her on inotropes at high doses and vasopressors. They changed her antibiotic regimen to meropenem, vancomycin, azithromycin, and acyclovir.
Azithromycin showed no response; therefore, it was discontinued after seven days.
Blood cultures and endotracheal aspirate cultures were negative, but the endotracheal aspirate’s Gram stain showed a marked inflammatory response, although no organism grew.
The working diagnosis of Legionella infection was made.
On day 13 of hospital admission, the baby’s limbs developed an erythematous macular rash, which gradually became generalized to involve the other parts of the body over the next four days.

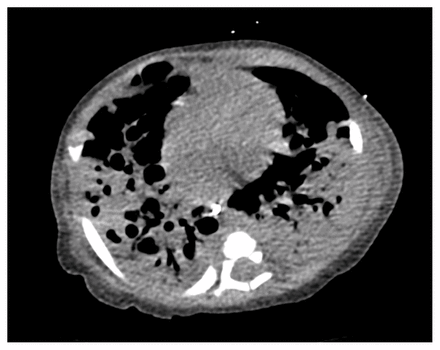
A computed tomography scan showed necrotizing pneumonia. Respiratory cultures grew pan-sensitive Pseudomonas aeruginosa, Legionella pneumophila serotype 6, and meropenem-resistant, piperacillin-tazobactam–sensitive Cupriavidus gilardii.
Doctors started her on Azithromycin and rifampin, which resulted in the improvement of the baby’s condition, and ultimately the intensivist extubated her within 48 hours of this regimen. The baby remained on mechanical ventilation for five weeks.
The infant improved substantially so the doctors discharged her at 2 months of age with home oxygen and advice to follow-up.
In this case, the most probable source of legionella was the prefilled water tub. It was not possible to test the water from the tub as they had already emptied and disinfected the tub.
References:
Michelle Barton, Brianna McKelvie, Aaron Campigotto, Tara MullowneyCMAJ Oct 2017, 189 (42) E1311-E1313; DOI: 10.1503/cmaj.170711