Case Presentation: Tularemia
A 59-year-old woman presented to the emergency room with a squirrel bite on the right ring finger and the left index finger, for seven days. According to a woman she encountered an immobile squirrel, who attacked her when she tried to help it. She presented with malaise, fever, chills and swelling in the right elbow. Moreover, she gave a history of hypothyroidism and lupus erythematosus. At this stage, the doctors did not have Tularemia as one of the differential diagnoses.
Examination
The doctors examined the patient’s right ring finger and found a small bite mark, which was reddened with no local inflammatory signs. Although signs of lymphadenitis were positive on the ulnar side of the elbow, no other signs were seen. Furthermore, the peripheral sensitivity, as well as movement skills and blood flow, were intact. Doctors further examined the left index finger, which had a minor bite, with no signs of inflammation. Her vital signs were normal and mild sinus tachycardia was noted.
Investigations
The doctors sent some blood tests along with an X-ray of the right ring finger, CSF and urine culture, and CT brain scan. Moreover, PCR for coronavirus and influenza A and B were also sent.
These tests revealed a raised CRP of 28.6 mg/L, however, there was no leukocytosis. The rest of the investigations were non-significant. The X-ray and CT scan showed no pathological findings. Additionally, CSF and urine culture were also negative. The woman was also negative for coronavirus and influenza.
Treatment
The doctors initially treated her with the antibiotic cefuroxime 500 mg orally twice a day. They also cleaned her wounds and bandaged them.
The next day, they added intravenous antibiotics to the regimen which included ampicillin and sulbactam, 2g and 1g respectively, 3 times a day. However, the patient’s condition did not improve and her fever increased up to 39.2 degrees Celsius. This lasted for 6 days. Additionally, CRP also increased to 185 mg/L. Therefore, the doctors further intensified the treatment regimen, with the addition of a combination antibiotic regimen of piperacillin and tazobactam, 4g and 0.5g respectively. After doctors administered this antibiotic regimen, her CRP fell to 74 mg/L.
Diagnosis
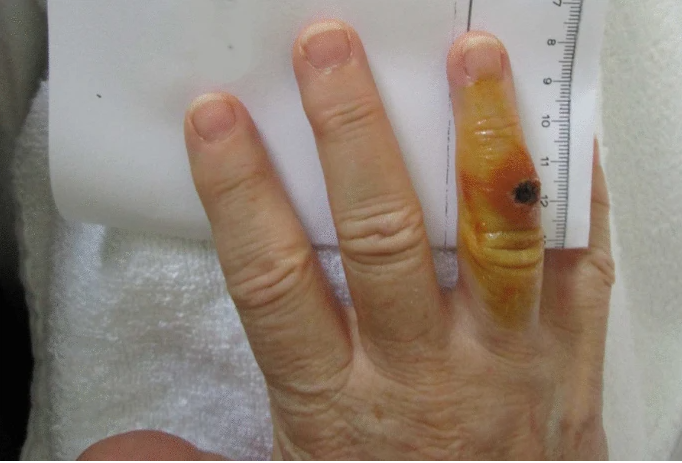
The lesion on the patient’s right hand developed into an ulcer-like lesion, with a reddened and swollen appearance. At this stage, the doctors suspected tularemia as a possible diagnosis. They made the decision to send a wound sample from the right-hand ulcer for microbiological examination. Furthermore, a serum sample of A-1825/2 was also sent for antibody detection, along with ELISA. ELISA demonstrated antibodies against F. tularensis Igpoly, immunoglobulin (Ig)G and IgM.
On the basis of this diagnosis, doctors administered 500 mg of ciprofloxacin, twice a day for fourteen days. With this treatment regimen, the CRP dropped to 15 mg/L.
Prognosis
On day 17th of the squirrel bite, the patient showed significant improvement, due to the specified treatment against tularemia. She had no fever on day 17, and her CRP had also dropped to 15 mg/L. Therefore, the doctors discharged her.
This case highlights the importance of correct diagnosis of animal bites, such as rabbits, dogs, squirrels and cats. The animal bites should not be managed with routine management. Such cases should include wound irrigation, wound debridement, rabies and tetanus prophylaxis. Moreover, if doctors don’t observe any improvement, they should consider a diagnosis of tularemia.
Tularemia: What is it?
Tularemia refers to an infectious disease caused by the bacteria Francisella tularensis. It is also known as rabbit fever or deer fly fever. The disease primarily infects rabbits, hares, rodents, birds, sheep, dogs, and cats.
Tularemia is transmitted to humans in many forms such as insect bites and exposure to an infected animal. It carries a poor prognosis, with high fatality rates. Although, it can be managed if diagnosed early.
Symptoms of Tularemia
The bacteria that causes this disease has an incubation period of 21 days, although symptoms can manifest within 3 to 4 days. There are many types of tularemia, and the classification is based on where the bacteria enter the body. Each type has different symptoms. The ulceroglandular type is the most common type. The symptoms include skin ulcer, swollen and tender lymph nodes, fever with chills, headache and malaise. The glandular type of tularemia has similar signs and symptoms as that of ulceroglandular although, there are no skin ulcers. The oculoglandular type affects the eyes causing eye pain, eye redness, eye swelling, eye discharge, increased sensitivity to light and ulcer on the eyelid. Other types include oropharyngeal and typhoidal tularemia which are less common types.
Prevention, Diagnosis, and Treatment
There are certain jobs that may increase the likelihood of developing these diseases such as hunting, farmer and wildlife manager. Such people should use preventive techniques such as using gloves while handling animals, avoiding sick and dead animals, using insect repellents, and drinking water.
Tularemia can be diagnosed with the help of tests that help detect the bacteria in the body. These include ELISA and CSF or urine culture. Although, it may be difficult to diagnose due to the similarity of symptoms with other diseases.
The management of Tularemia is directed at the eradication of the bacteria, by antibiotics. Moreover, doctors can use supportive management to manage complications.
.